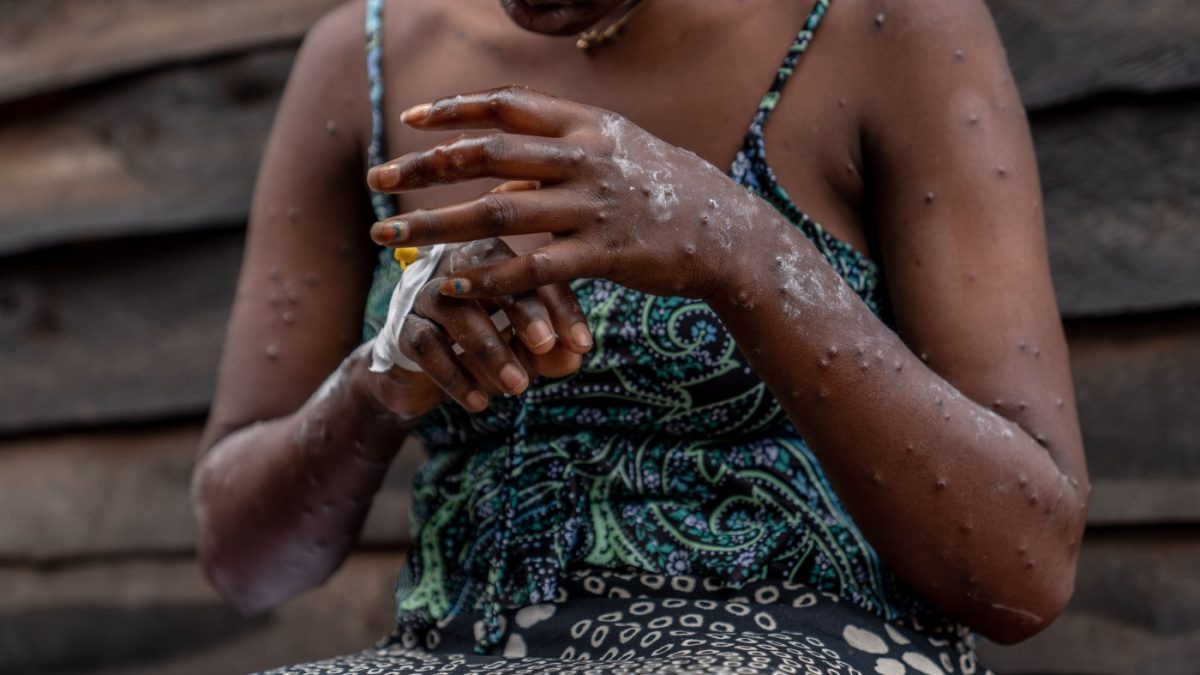
Mpox created quite a stir in 2022 and 2023, with reports of tens of thousands of cases globally and around 30,000 in the U.S. alone within just one year. This was amid reports of painful symptoms and extensive vaccine mobilization efforts.
Now, in 2025, you’d think it was just a distant memory. But it’s not quite that simple.
Caroline Mugun, a nurse at an mpox isolation ward in Mombasa, Kenya, remarks, “You see the agony the patient goes through. It’s on another level.”
The virus has continued its rapid spread across Africa. Currently, 24 African nations are experiencing mpox outbreaks, up from just 13 last year, as reported by the Africa Center for Disease Control and Prevention. For many of these nations—from Gambia to Kenya and Uganda to South Sudan—this marks their first encounter with mpox.
Today, August 14, marks a year since the World Health Organization declared mpox a Public Health Emergency of International Concern, a designation signaling utmost alertness. Critics, however, argue that the global response has not lived up to expectations, despite a pledge of $1.1 billion from various countries, foundations, and organizations to aid mpox control.
So where does the mpox crisis currently stand, and what could that imply for future outbreaks of serious diseases?
“Walking blind”
Traditionally, mpox was linked to isolated forest regions in West and Central Africa, where the virus occasionally jumped from small wild animals to hunters, often children. It was initially named monkeypox due to cases observed in primates, but the primary carriers are now believed to be other infected animals, like rodents. The name changed in 2022.
When the WHO raised the alarm last year, mpox had taken on a different character from its earlier forms.
A new strain, designated Clade 1b, had emerged and was spreading quickly, particularly among sex workers and their clients. The outbreak’s epicenter, the war-torn eastern region of the Democratic Republic of Congo, attracted laborers due to its vast mineral resources. Soon, the new strain began appearing in nearby countries like Burundi, Kenya, Rwanda, and Uganda.
Fast forward to now, and that new strain has proliferated, with notable outbreaks of the other mpox strain as well. According to the Africa CDC, about 97,000 suspected mpox cases have been reported across the continent this year, along with nearly 600 deaths. Experts caution that these numbers may be significantly underestimated.
Anne Rimoin, an epidemiology professor at UCLA and an mpox researcher, explains, “Your case counts are kind of like shadows on a wall — they’re not telling you that very precise picture.” Stigma around sexually transmitted diseases, along with many affected individuals living in remote areas with limited detection capacity, means that many patients likely remain untreated and unrecorded.
Another factor affecting the accuracy of these figures is funding cuts to foreign aid during Trump’s presidency. The DRC ranked among the largest recipients of U.S. aid, some of which was directed towards the mpox response, including transporting samples for testing.
Dr. Chris Beyrer, an epidemiologist and director at Duke University, states, “We have really gone off a kind of data cliff. We are flying blind.” He adds that the stalled response feels less like flying and more like “walking blind.”
The available data indicates that while the virus’s geographic reach has expanded, the caseload appears to be decreasing in recent months. This trend has made Dr. Olivier le Polain, a unit head at WHO’s Health Emergencies Programme, cautiously optimistic. “When all the information points toward the same types of trends, it gives us some confidence that the trend is genuine,” he mentions.
“Three steps backward”
Despite some decline in cases, many mpox experts express serious concerns about the global response.
“This has basically been a very frustrating year,” comments Dr. Boghuma Titanji, an infectious diseases professor at Emory University. “For every two steps of progress, it seems we have taken three steps backward.”
Reasons for the ongoing challenges are numerous. The epidemic’s epicenter in eastern DRC is embroiled in a brutal conflict, with many key cities under rebel control and limited medical care available. Compounding this situation is a significant drop in global health aid from both the U.S. and various European countries.
Rimoin notes that mpox serves as a case study of how a global health crisis can unfold when biological risks collide with political and economic issues.
Vaccines
Many experts view the vaccine response as particularly inadequate.
Mpox is preventable through vaccination, yet only about 886,000 people have been vaccinated across a dozen African nations. Just over 3 million doses have reached the continent, far short of the targeted 10 million doses by the end of 2025, as per the Africa CDC.
The challenges began even before the WHO declared the health emergency, as it had not yet approved the mpox vaccine.
Beyrer recalls, “It’s like: ‘Well, you either have an emergency or you don’t.’” At that time, WHO director-general Tedros Adhanom Ghebreyesus pushed back against criticisms of inaction, citing incomplete information on the vaccines’ efficacy and safety. “We will not take shortcuts,” he emphasized.
Former President Biden’s pledge to send 1 million doses of the vaccine to Africa in September 2024 also exemplifies unmet commitments. As of July 2025, only about 90,000 doses had been delivered, and almost half of the remaining doses may be too close to expiration for shipping, according to Yap Boum, deputy head of Africa CDC’s mpox response.
Boum notes, “They can no longer be sent to the continent, which is a huge loss, because that one dose of vaccine is $100.”
Nurse Mugun from Doctors Without Borders reports that while interest in the mpox vaccine is strong, Kenya hasn’t yet begun its immunization program.
The U.S. Centers for Disease Control and Prevention and the Department of Health and Human Services did not respond to inquiries regarding the U.S. vaccine commitments.
What about the future?
Researchers and medical professionals warn that the lackluster global response may have significant implications for both the future of mpox and emerging disease threats.
Titanji fears that ineffective responses could undermine the WHO alert system’s value. The same applies to Africa CDC’s emergency declaration, which marked the first time the organization issued a Public Health Emergency of Continental Security. “If we’ve had the highest level of alert for 12 months and it hasn’t really impacted containment, how effective is this alert system?” she questions.
Dr. Jean Kaseya, director-general of Africa CDC, disagrees, asserting that tangible progress has been made in containment efforts. “Africa didn’t have this capacity. It’s now that we are building capacity,” he explains.
He highlights that a year ago, no African country had approved the mpox vaccine the U.S. sought to distribute, whereas now 17 nations have granted approval. Additionally, the laboratory network for testing suspected mpox cases has expanded dramatically in hotspot areas; for instance, Burundi has grown from two labs to 56.
Kaseya adds that this is the first time cross-continental collaboration has taken shape with an African entity leading resource allocation and coordination. He acknowledges, however, that substantial work remains.
Titanji agrees, expressing concern that the world is witnessing the virus becoming entrenched among humans. “The virus will evolve the more opportunities it is given,” she cautions.
Rimoin notes that while the U.S. has largely avoided the impacts of mpox so far, that situation could change. “Diseases we ignore abroad can quickly land on our doorstep,” she observes. “We’ve been lucky so far. I don’t know how long that luck will last.”