Millions of adults will experience permanent tooth loss, with many losing multiple teeth over time. In the U.S. alone, it’s estimated that around 178 million individuals are missing at least one tooth, which explains the prevalence of dentures and titanium implants.
However, dentistry is now looking for something more advanced—a living replacement that behaves like natural teeth. This concept is transitioning from theoretical animal studies into carefully controlled human trials.
Pamela C. Yelick from Tufts University School of Dental Medicine is part of a team working to bring this innovative idea closer to reality. A recent study by her and colleague Weibo Zhang has elevated the discussion significantly.
Dentures as Tooth Replacements
Tooth loss isn’t uncommon, and the likelihood increases with age. Statistically, about 7% of individuals aged 20 and older have lost all their teeth, a figure that rises to 23% among those aged 60 and above.
Modern implants are fused directly to the jawbone through a process known as osseointegration, a technique that originated with Per Ingvar Brånemark’s mid-20th-century work. This historical context helps explain both the stability of implants and their lack of sensitivity compared to natural teeth.
Natural teeth are held in place by periodontal ligaments, which provide sensation and enable slight movements—qualities that implants miss. This difference affects tactile sensitivity, making implants feel less responsive.
Additionally, the way forces are transmitted through an implant differs from a tooth root cushioned by ligaments. Over time, this can lead to bone loss around the implant and other biological complications.
Two Routes to Living Teeth
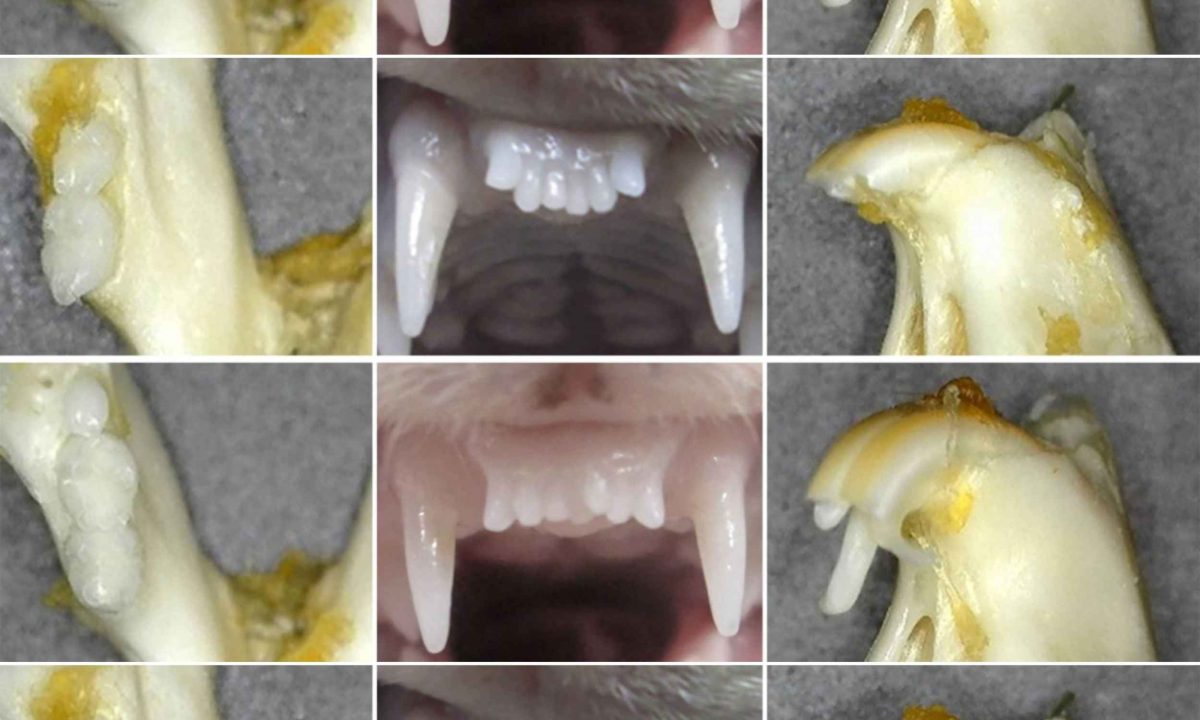
One method involves growing a replacement tooth from tissue using a scaffold that guides cells into forming a tooth structure. A significant animal study used decellularized tooth bud scaffolds filled with human dental pulp and epithelial cells, which were implanted in adult minipig jaws, successfully forming tooth-like tissues, including ligaments.
The alternative approach focuses on stimulating tooth development directly in adults by delivering the right signals to cells. Teams are exploring the intricacies of early human tooth formation to identify the necessary cues for organized growth.
Tooth Roots and Ligaments
The scaffold method is significant because the resulting structures aren’t just static. They develop supporting ligaments and mineralized tissues over several months, moving this approach closer to practical human applications.
“Creating a living tooth root that can accommodate an artificial crown, complete with dental pulp and secured by ligaments instead of being attached rigidly to the jaw, would represent a considerable improvement to oral health—and, by extension, overall health,” Yelick noted.
Protein Aids Tooth Replacement
Another avenue of research is focused on a protein called USAG-1 that inhibits tooth formation. Blocking this protein in mice has led to the regrowth of missing teeth, and similar results were seen in ferrets, which have a tooth replacement pattern akin to humans.
“A single treatment was sufficient to regenerate an entire tooth,” explained Katsu Takahashi, whose team reported these findings while at Kyoto University.
The development of a humanized anti-USAG-1 antibody is underway, and preparations for phase 1 trials are in progress. This marks a crucial shift from proving concepts in animals to safety and efficacy testing in humans.
Funding updates show aims to conduct initial human studies and potentially expand to pediatric trials if early outcomes are promising.
Defining Success
A functional living tooth would restore sensory capabilities, allowing individuals to adjust bite force and sense irregularities. These teeth could also better connect to bone through proper tissues, potentially minimizing pain and reducing bone loss compared to traditional implants.
Long-term, such advancements might extend the lifespan of replacements compared to current solutions, which often require repair or replacement after significant wear.
Cost and Complexity Considerations
Cell-based therapies must be reliably produced and affordable to compete with existing prosthetic options. Sourcing compatible epithelial cells at the appropriate developmental stages poses a challenge, which is why researchers are currently using young pig tooth buds to refine methods for utilizing a patient’s own cells.
Progress is also being made with induced pluripotent stem cells to create enamel-forming cells and address enamel defects. As techniques improve, vital concerns will include safety, quality control, and cost-effectiveness relative to implant procedures.
Future of Tooth Replacement Technology
Research on human fetal tooth development has outlined specific epithelial subpopulations and their signaling pathways. This resource can guide researchers in nudging adult cells toward creating new tooth structures.
If these signals can be delivered effectively—either through staged therapy in the jaw or constructs that complete their development in the tooth socket—we may one day see dentists replacing lost teeth with living ones that integrate seamlessly and function naturally.
This study has been published in Stem Cells Translational Medicine.