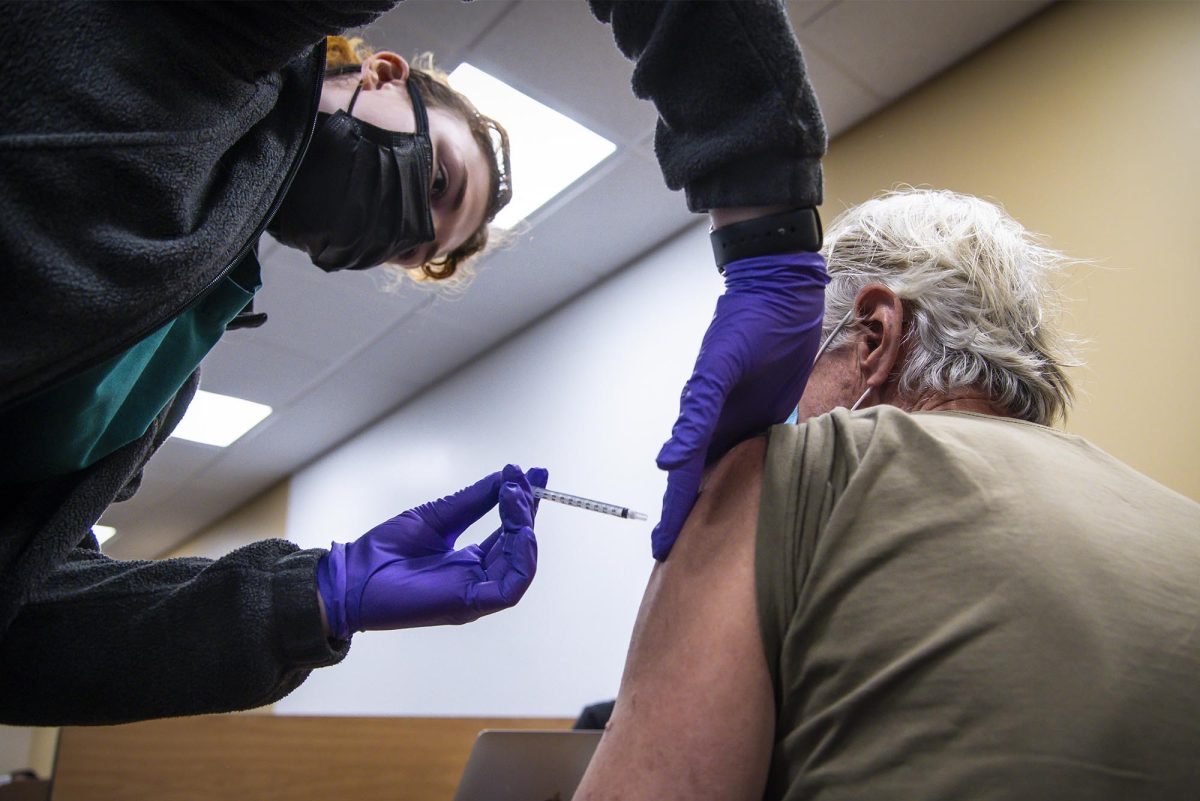
Vermont’s Covid-19 Booster Access Amid New Federal Regulations
Even with recent federal restrictions on Covid-19 vaccinations, many residents in Vermont can still access booster shots. However, some details regarding Medicare reimbursement and federal guidelines are still unclear.
In a post from late August, Health and Human Services Secretary Robert F. Kennedy Jr. announced that the FDA has authorized Covid-19 booster shots, but only for those aged 65 and older or individuals with underlying health issues.
Vermont’s health officials are now waiting for guidance from the Centers for Disease Control and Prevention, which usually influences public health policies and insurance coverage for those seeking a booster shot this fall.
“I suggest checking online for appointment availability or contacting local pharmacies,” said Julie Arel, the interim health commissioner for the state.
Pharmacies in Vermont, including Kinney Drugs and CVS, are moving forward with administering the latest Covid vaccines, as they order directly from manufacturers. In contrast, healthcare providers like doctors’ offices typically acquire vaccines through the state, which hasn’t yet received orders from the CDC.
According to Kinney Drugs’ spokesperson, Alice Maggiore, the pharmacies are permitted to administer updated vaccines to individuals over 65 and those aged 12 to 64 who confirm having specific qualifying conditions as outlined by the CDC.
CVS allows anyone over five years old who meets eligibility requirements under the same CDC conditions, or anyone older than 65, to receive the vaccine, as stated by company executive Amy Thibault.
The CDC’s qualifying risk factors include various health concerns, ranging from asthma to mental health issues. Notably, a doctor’s prescription is not required to confirm these underlying conditions at Kinney or CVS.
Typically, insurance plans cover vaccinations administered in pharmacies. However, there are uncertainties about whether private and government insurers will cover these vaccines this time around. There’s some confusion, and as Arel mentioned, “It’s a little bit mind-boggling.”
Blue Cross Blue Shield of Vermont, the state’s largest private insurer, has confirmed that it will continue covering the vaccine without additional cost or prior approval for its members. This coverage is expected to extend through 2026. Meanwhile, MVP, another private insurer in the state, doesn’t foresee any changes in its vaccine coverage policy, according to spokesperson Elizabeth Boody.
The coverage policies of employer-sponsored insurers and military health systems like Tricare remain uncertain.
Given that the FDA has approved the vaccine for those aged 65 and over, it is likely that Medicare will cover it too. Vaccine policy expert Dorit Reiss suggests that once the FDA authorizes a vaccine, Medicare usually follows suit.
Typically, a Covid vaccine goes through three stages of approval: initial FDA authorization, a recommendation from a CDC panel called ACIP, and the actual rollout. ACIP is scheduled to meet soon to make its recommendations, and many are waiting with bated breath, especially after recent changes within the panel that have raised some concerns.
Vermont is now considering how to navigate this situation and is exploring what existing state laws might allow for adjustments to the usual process.
Jumping into this uncertain arena isn’t common for vaccines, although healthcare providers often have some flexibility in prescribing medications. The ambiguity regarding what defines an underlying condition adds another layer of complexity.
“There’s some flexibility. But because of this lack of clarity, we can expect some hesitancy,” Arel commented. “This confusion could potentially lead to lower vaccination rates, and we want to avoid that.”
The Department of Health is also looking toward neighboring states for guidance on handling the situation. Recently, Vermont joined a regional health coalition to collectively address potential shifts in federal health guidance. Although there’s no unified approach yet, Arel suggests it’s a step towards enhancing confidence in public health decisions across the Northeast.
For instance, in Massachusetts, the governor has mandated local insurance providers to cover vaccines recommended by the state’s health department, even if they deviate from federal guidelines. This flexibility reflects a willingness to adapt to evolving circumstances.
Arel concluded with a call for simplicity in communication regarding vaccinations. “It’s vital that our messaging is clear,” she emphasized, expressing commitment to navigating the current challenges effectively.