AI Integration in Medicare Raises Concerns
Beginning January 1, several states will start using artificial intelligence to help make Medicare coverage decisions. However, not everyone is on board with this change. Some experts are voicing skepticism, suggesting that the system’s incentives may lead to even more denials of care. “Show me the incentives and I’ll show you the results,” a quote that some advocates have pointed out, emphasizes this concern. They argue that the initiative is designed to cut down on fraud and inefficiencies.
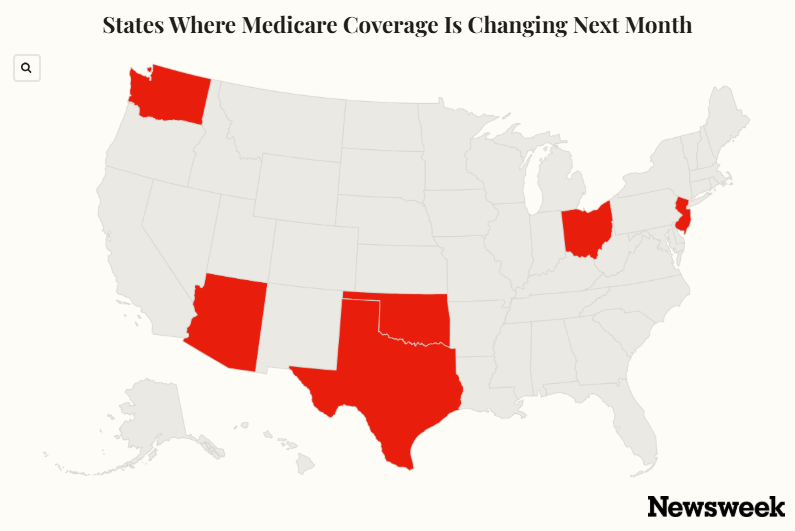
This transition will kick off in states like Washington, Arizona, Ohio, Oklahoma, New Jersey, and Texas, where traditional Medicare recipients will participate in federal trials using AI.
Why This Matters
The launch of this new program has spurred pushback among certain Medicare users and industry experts. There are worries that AI could lead to increased coverage denials, which might, in turn, strain finances and impact health outcomes in the years to come.
Many beneficiaries already grapple with prior authorization processes, which often delay necessary treatments or procedures until approvals are granted.
Key Information
Six states are implementing pilot programs referred to as “Eliminate Wasteful and Inappropriate Services.” These states include Washington, Arizona, Ohio, Oklahoma, New Jersey, and Texas.
The aim is to cut fraud and waste through AI-driven pre-approval processes for certain outpatient treatments labeled as “low-value services.”
“For the first time, seniors will have to get prior approval from a private contractor, who will be compensated based on how many claims they reject,” noted Michael Ryan, a financial expert. He added that traditional Medicare has functioned without such requirements for six decades.
Roughly half of all Medicare recipients utilize traditional Medicare, and prior authorization has mostly been associated with Medicare Advantage, the privatized alternative.
Procedures where AI might dictate pre-authorization include nerve stimulation treatments, steroid injections for pain relief, cervical fusings, knee surgeries, treatments for impotence, and certain skin replacements.
Chris Fung, CEO of Smile Insurance, highlighted the novelty of using AI for pre-authorization in this context. He pointed out that while private insurers may already use AI in their pre-approval processes, there’s typically a more human-driven appeals system in place. The uncertainty lies in whether Medicare will have a similarly structured appeals process for these new AI-driven decisions.
Concerns are emerging that extending AI capabilities could harm Medicare beneficiaries in the long term, particularly because AI firms are financially incentivized to save money by denying claims.
“If the incentives support denying care, that’s precisely what will happen,” remarked Kevin Thompson, CEO of 9i Capital Group. He believes that these AI systems are likely to reject claims more readily due to their design. While the goal is to tackle overbilling and fraud, this could lead to prolonged waiting periods and more denied treatments.
Public Reactions
The CMS has emphasized its commitment to eliminating fraud, waste, and abuse, with Dr. Mehmet Oz stating that this new model aims to modernize Medicare by testing a more efficient pre-approval system while also safeguarding beneficiaries against unnecessary procedures.
Financial literacy instructor Alex Bean expressed apprehension about the AI pilot program. He emphasized that if the technology accelerates claims denials, beneficiaries could face increased obstacles in obtaining necessary healthcare services.
Thompson also cautioned that what is being promoted as a solution to fraud might actually lead to more denied legitimate claims, which is clearly not ideal for those who rely on timely access to care.
Ryan added that this move could normalize a profit-oriented approach in Medicare. If the pilot succeeds within its six years, it could potentially expand nationwide, effectively transforming Medicare into a system more akin to commercial insurance, with corporate interests complicating patient access to care.
Looking Ahead
This new model may indeed reduce fraud and waste, but it also risks denying valid claims. While proponents believe these updates can help combat problems within the program, they might turn contentious if many legitimate claims are rejected. Bean stated, “A successful pilot could help mitigate challenges before any further expansion.”