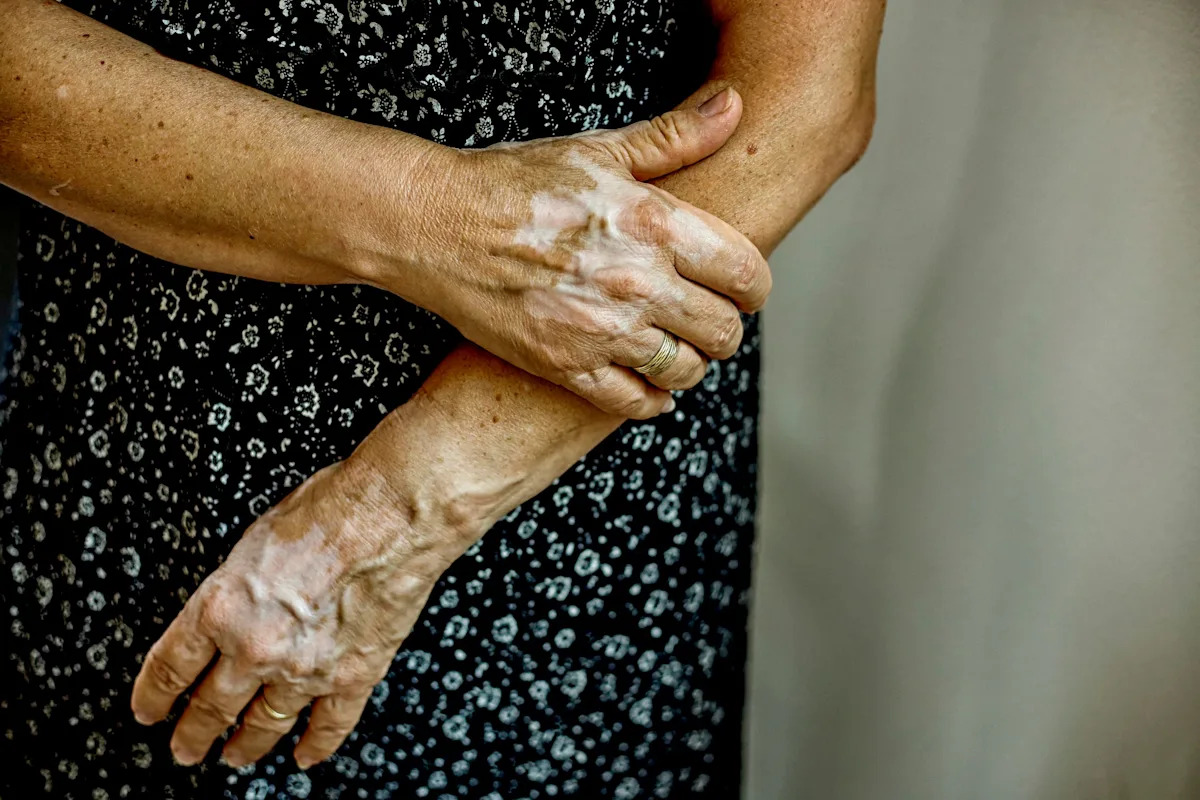
Imagine waking up feeling completely drained, like you didn’t even sleep. Or perhaps you’ve noticed that your hands are stiff and swollen, making even simple tasks—like opening a jar or typing—difficult.
Sure, it’s easy to attribute these feelings to stress or just a rough week. But for about one in ten Americans, these seemingly minor changes could signal something more serious.
Many people dealing with autoimmune diseases have often lived with their symptoms for months, if not years, before they receive a proper diagnosis. The reason? Symptoms can be intermittent, overlap with other conditions, or simply lack clear defining characteristics that might raise alarms initially.
This means autoimmune diseases can sometimes be easy to overlook. Once they do make an appearance, they can impact daily activities significantly—making work, choosing foods, or even self-care a challenge, as noted by Dr. Stephanie Sasha De La Guarda from Baptist Health South Florida.
Getting a grasp on autoimmune diseases, what triggers them, and how they’re managed can be an essential first step towards understanding, better care, and eventually, relief.
James Van Der Beek, Celine Dion, and others share their health challenges
Celebrities like Selma Blair, Jada Pinkett Smith, Selena Gomez, and Justin Bieber have been open about their ongoing health battles, encouraging their fans to speak up as well. For instance, James Van Der Beek revealed last November that he’s fighting Stage 3 colorectal cancer.
A year after that, the 48-year-old actor announced an auction featuring memorabilia from his earlier days as a teen heartthrob, scheduled for December 5–7, 2025.
Understanding autoimmune diseases
Having an autoimmune disease essentially means the immune system, which usually defends the body against infections and illnesses, mistakenly turns on healthy tissues, according to Dr. Alexandra Reese from the Cleveland Clinic.
Instead of recognizing various organs, joints, or glands as part of itself, the immune response is triggered, leading to a continuous state of inflammation. Over time, this can result in tissue damage and organ dysfunction.
Autoimmune diseases are quite common, with between 80 and 150 distinct types identified, affecting different body parts. Notable examples include rheumatoid arthritis (targeting joints), lupus (affecting skin, kidneys, and more), multiple sclerosis (damaging nerve coverings), type 1 diabetes (destroying insulin-producing cells), and inflammatory bowel diseases like Crohn’s disease.
Each condition presents varying symptoms, but generally, those living with an autoimmune disease might struggle with fatigue, joint pain, and organ issues, which could severely impact physical capabilities, social life, and work. Symptoms like muscle weakness, swelling, rashes, and brain fog are also commonly reported, all of which can disrupt daily life.
Moreover, while some autoimmune diseases may be mild or sporadic, others can be progressive and even threaten life, especially if they impact vital organs.
Causes of autoimmune diseases
Autoimmune diseases result from a complex mix of genetics, environmental elements, and imbalances in the immune system.
It’s rarely just genetics at play. Environmental factors—like smoking or exposure to certain pollutants—are crucial too, as highlighted by Dr. De La Guarda. Additionally, infections from viruses and bacteria can act as significant triggers.
Hormonal factors also contribute notably, particularly since autoimmune diseases often emerge in women, frequently during childbearing years or after significant hormonal changes.
In many cases, several factors interplay. For instance, rheumatoid arthritis may come from a “two-hit phenomenon,” where someone who has a genetic predisposition faces an environmental trigger.
Chronic stress, poor sleep, and disruptions to the gut microbiome are other potential contributors. Research increasingly indicates that gut health plays a vital role in immune function, potentially affecting inflammation and the propensity for autoimmune responses.
Treatment options for autoimmune diseases
Whatever the cause, autoimmune diseases typically cannot be fully cured. However, many treatment options can help manage symptoms, aiming to enhance the quality of life for patients.
Treatments are personalized based on the specific conditions and severity of symptoms. The primary goal in medical care is often to control inflammation, regulate immune system activity, and prevent long-term damage, frequently through medication. This may include insulin, hormone replacement drugs, anti-inflammatories, corticosteroids, and others.
Sometimes, particularly in severe cases, hospitalization could be necessary to stabilize organ function or treat complications. Long-term care typically involves regular check-ups and tests to track disease activity.
On a personal level, lifestyle strategies are crucial. Getting enough sleep, managing stress, and engaging in regular low-impact exercise can help mitigate inflammation and support overall wellness.
Many also find that physical or occupational therapy and counseling can be beneficial, as chronic illnesses affect both body and mind. While there’s no singular diet that addresses autoimmune diseases, maintaining balanced nutrition that supports gut health—while limiting overly processed foods—can be advisable for enhancing well-being.
Thanks to advancements in diagnosing and managing these diseases, many individuals can lead fulfilling lives by adhering to prescribed therapies, recognizing triggers, and making healthy lifestyle choices. It’s challenging to live with an autoimmune disease, yet it’s essential to remember you’re not alone; millions are navigating similar experiences.