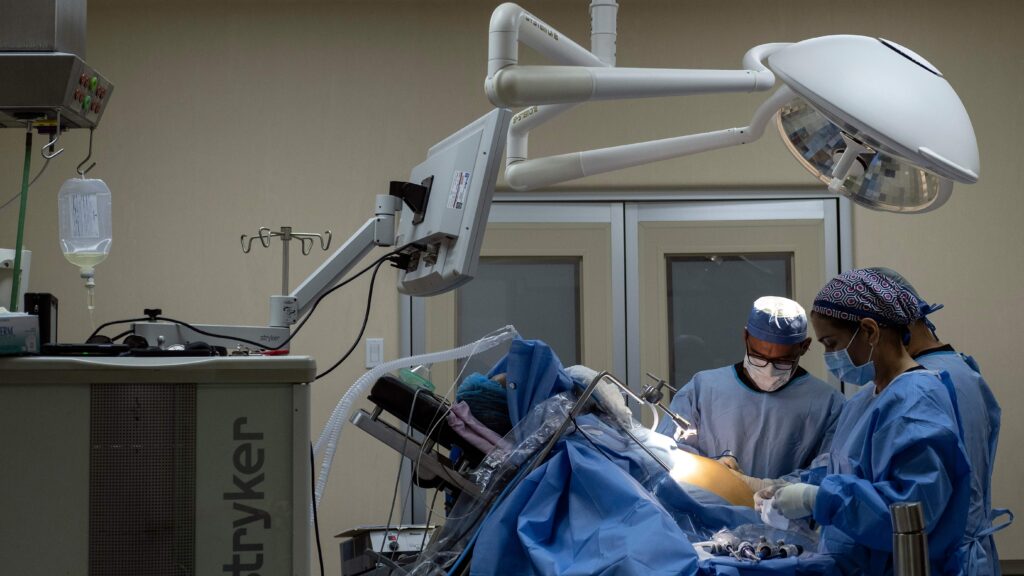
Understanding Bariatric Surgery in Type 2 Diabetes Treatment
When Dr. Mary Elizabeth Patti, an endocrinologist, evaluates a patient with type 2 diabetes who may benefit from weight loss, she looks beyond just their body mass index and blood glucose numbers. She also considers the challenges that come with social vulnerability—things like low income, food insecurity, and limited healthcare access can significantly influence treatment decisions. These elements are closely tied to the onset of type 2 diabetes and obesity.
For over a dozen years, Patti has been a key figure in conducting long-term randomized clinical trials in four U.S. cities, which compared bariatric surgery with medication and lifestyle management for type 2 diabetes. In 2024, one such trial revealed that bariatric surgery led to notably better outcomes, including lower blood glucose levels, greater weight loss (28% versus 10%), reduced dependence on diabetes medications, and decreased cardiovascular risk factors.
A recent secondary analysis, published in the Annals of Internal Medicine, explored how various social determinants of health affected outcomes after bariatric surgery as opposed to medical therapy for individuals with type 2 diabetes and obesity.
The study found that bariatric surgery outperformed medical therapy across different social backgrounds, not just in more deprived areas. However, the analysis was smaller, and some participants switched from medication to surgery and vice versa. The authors recognized these limitations, especially in light of the faster development of more effective obesity drugs not thoroughly covered in the study.
Patti pointed out that “bariatric surgery remains an underutilized option.” Even when compared to the newer, effective medications available, she believes surgery presents a more sustainable treatment for diabetes and obesity. “I’m not a surgeon,” she admits, but she urges that the surgical option shouldn’t be overlooked.
During the initial stages of the overall study, which took place in Boston, Cleveland, Pittsburgh, and Seattle, 355 participants were assigned either to medical therapy or one of three surgical methods: gastric bypass, sleeve gastrectomy, or adjustable gastric lap banding. Patients in the medical and lifestyle intervention group received personalized nutrition counseling and education about exercise and glucose monitoring.
As the study progressed, fewer participants opted for lap band surgery, which has lost popularity, while newer obesity medications became increasingly available. Some participants from the medication group eventually chose surgical options, while others who had surgery began using obesity drugs. By the twelfth year of the study, over a third of participants in the medical group and more than a quarter in the surgical group were on incretin-based therapies, including both older and newer GLP-1 medications.
This secondary study evaluated data from 258 adults with type 2 diabetes, who had either undergone surgery or received medical and lifestyle therapy. Participants were categorized by their ZIP codes to determine the Area Deprivation Index of their neighborhoods, and their weight and hemoglobin A1c levels were monitored for seven to twelve years.
Although surgery seemed to yield better outcomes for individuals in high deprivation areas, the results were not statistically significant, according to Patti.
Managing diabetes alone can be incredibly challenging, particularly amidst socioeconomic difficulties. For example, making dietary changes can strain family budgets, and exercising can be unrealistic for those juggling multiple jobs. Even those who are insured can struggle to consistently access necessary medications and keep up with healthcare processes. “If you lack an advocate in the healthcare system, navigating approvals and prior authorizations is tough when you’re dealing with social and financial pressures,” Patti explains.
Even as enthusiasm for GLP-1 medications increases, patients might not prioritize surgery, regardless of their social situations. Neither route is necessarily easy. A key difference arises when considering significant weight loss; surgery generally presents a more viable option for those aiming to shed 100 pounds.
Melanie Jay, a professor of medicine and population health at NYU, remarked in an interview—though she wasn’t involved in the study—that the growing options are beneficial. However, managing obesity often requires a long-term approach, and a one-size-fits-all solution does not yet exist.
Interestingly, the success mechanisms behind surgery and medical therapy exhibit remarkable similarities, which can sometimes be overlooked amid the excitement about new pill alternatives to injections.
Bariatric surgery can suppress appetite and alter the way nutrients interact with the intestine, boosting the secretion of GLP-1 hormones after meals, further enhancing diabetes control.
Patti noted that with surgery, patients aren’t halting medications due to side effects or insurance issues, providing a more persistent means to trigger similar appetite and metabolic changes.
Jason Samuels, a surgery professor at Vanderbilt, expressed his view that obesity therapies are still underutilized. Despite the proven safety and effectiveness of bariatric surgery, it reaches only a fraction of patients who could benefit. He acknowledged the importance of the study, even as new drugs emerge.
“In the future, next-gen incretin-based agents may help some patients catch up, but practical concerns like durability, side effects, compliance, affordability, and access will be crucial in matching surgical results within diverse populations,” he noted in an email about obesity medications. “More comprehensive, long-term studies are essential to determine the best treatment for each patient.”
Patti emphasizes the need for surgery to remain a topic of conversation in treatment planning. “Epidemiology and population studies consistently show that bariatric surgery is more effective in enhancing diabetes control, achieving remission, reducing complications, and extending life expectancy. Yet, when discussing options with individual patients, the focus must always be on finding the best personal fit,” she concluded.