Measles Exposure Warning in Clackamas County, Oregon
CLACKAMAS COUNTY, Ore. — Health officials from the Oregon Health Authority (OHA) and Clackamas County have issued a notice regarding potential measles exposure.
Individuals who were at the following location during the specified date and time might have been exposed to the virus:
- Kaiser Permanente Sunnyside Medical Center Emergency Department, located at 10180 Southeast Sunnyside Road in Clackamas, between 11:28 a.m. and 1:53 p.m. on Monday, January 26, 2026.
People at this location are advised to reach out to their healthcare provider and inform them of their potential exposure to measles. Healthcare professionals can assess immunity levels based on vaccination history, age, or lab evidence of past infection.
This potential exposure is linked to a new measles case in Clackamas County, marking the second instance this year. The first case was reported on January 16.
While Clackamas County has reported new cases, Linn County has already confirmed two cases in early January. During that time, health authorities identified two locations where public exposure could occur:
- Lebanon Community Hospital Emergency Department on January 6 from 8:53 p.m. to 7 a.m. on January 7.
- Albany General Hospital Emergency Department on January 7 from 4:59 a.m. to 8:15 a.m.
Measles Cases in Oregon
The first confirmed measles case in Oregon for 2025 occurred in June, involving a person hospitalized in the Portland area after contracting the virus while traveling internationally.
Last May, the OHA noted a record high of nonmedical vaccine exemptions for kindergartners. Surprisingly, many families still opted to vaccinate their children.
In the state, a record 9.7% of kindergartners claimed nonmedical exemptions for the 2024-2025 school year, which is the highest rate ever recorded. This trend has increased from 8.8% in 2024, during which Oregon had one of the highest nonmedical exemption rates in the country according to the CDC.
Understanding Symptoms and Complications
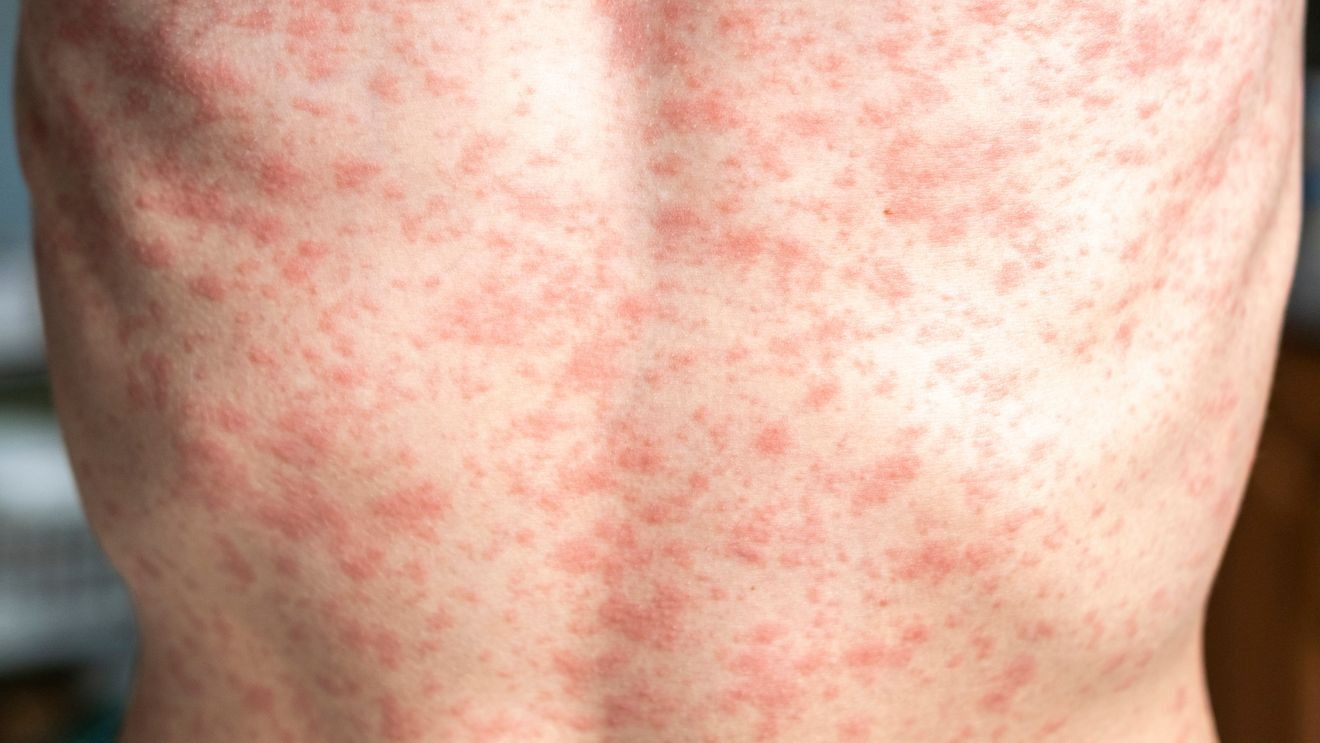
Measles is transmitted through the air, often from coughing or sneezing, and can remain airborne for up to two hours. Individuals are contagious from four days before a rash appears, continuing up to four days after.
Symptoms can manifest seven to 21 days after exposure, generally beginning with a fever, cough, runny nose, and red eyes, followed by a rash. Complications may include ear infections, lung infections, and, in rare cases, brain swelling.
Measles is notoriously contagious and poses serious risks, especially for infants, young children, adults over 20, pregnant women, and individuals with weakened immune systems.
Historically, developed nations have seen one or two fatal cases per 1,000 reported measles cases. The virus has a concerning aspect known as “immune amnesia,” where an infected person’s immune system may reset, losing prior disease immunity.
Statistics indicate that in a group where measles is present, about 90% of unvaccinated individuals will contract the virus, which can remain airborne for an extended period.
Even in generally healthy individuals, measles can lead to severe complications:
- 1 in every 1,000 measles cases may result in acute encephalitis, potentially leading to lasting brain damage.
- 1 to 3 out of every 1,000 infected children may die from related respiratory and neurological issues.
Subacute sclerosing panencephalitis (SSPE) is a rare but fatal neurological disease that can emerge, characterized by:
- Behavioral and cognitive decline.
- Seizures typically developing 7 to 10 years post-infection.
Health authorities urge those experiencing symptoms of measles not to arrive at medical facilities without prior notification. Instead, they should call ahead to ensure safe and non-exposing entry.
The measles vaccine, particularly the MMR vaccine, offers a high level of protection with two doses resulting in 97% effectiveness against the virus.
The recent resurgence of measles cases is attributed to worldwide increases in outbreaks, raising concerns about unvaccinated travelers reintroducing the virus to the U.S.
In the past, measles posed a significant health risk in the U.S., especially for children, with numerous cases and fatalities prior to the 1960s. The introduction of the measles vaccine in 1963 drastically reduced case rates, deaths, and severe complications.
By 1981, less than 1% of historical case numbers were recorded, with only a minority of U.S. counties reporting any instances, according to the CDC.