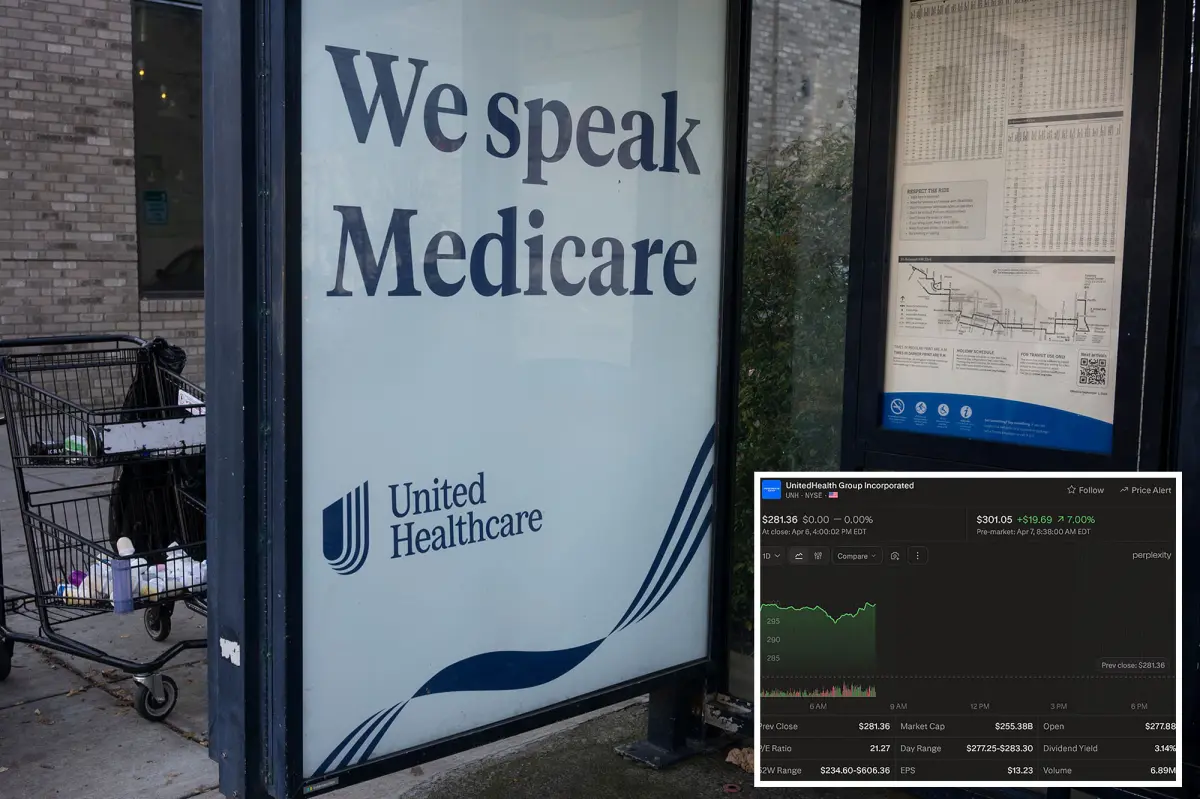
UnitedHealth Group Inc. experienced a notable surge in its shares, climbing over 8% after federal officials revealed Medicare Advantage payment increases that exceeded expectations. This news is a boost not just for UnitedHealth, but for the entire managed care industry.
The stock jumped from a closing price of $281.41 on Monday to more than $305 during intraday trading, marking a gain of about 8.5% in just one day.
This rally follows a period of robust stock price growth.
Earlier, UnitedHealthcare had seen its stock decline following the untimely death of CEO Brian Thompson in December 2024. Analysts note that ongoing reputational issues, rising expenses, and regulatory pressures have further contributed to challenges for the company.
The Centers for Medicare and Medicaid Services (CMS) recently announced an increase in Medicare Advantage payments, averaging 2.48% for 2027. This is a stark contrast to the mere 0.09% increase initially proposed earlier in the year.
When accounting for the estimated risk scores, the total payments are expected to rise by 4.98%, according to CMS.
This sharp shift from a near-zero offer to a significant upward adjustment has sharply boosted the insurer’s stock price.
As the largest Medicare Advantage insurer by enrollment, UnitedHealth is especially impacted by government reimbursement levels; even minor adjustments can lead to significant financial implications.
UnitedHealth collects a fixed monthly payment from the federal government for every enrolled member.
CMS forecasts that the final rate will lead to over $13 billion in additional payments to insurance companies by 2027.
The year started with a more pessimistic view on the outlook for managed care.
Concerns had emerged over the initial proposal, which suggested insurers might encounter increased margin pressure due to rising healthcare costs.
A key turning point was CMS’s decision to abandon a proposed review of the risk adjustment model.
Regulators had been contemplating updating these models with newer data, a move that could have decreased payments to insurers. Instead, CMS opted to keep the current model through 2027, recognizing the need to allow the Medicare Advantage market some breathing room.
This choice significantly alleviated the potential negative effects of proposed risk model changes and played a major role in the upward revision of the final rate.
It reflects a more cautious stance from regulators, who are working to sustain the program while ensuring payment accuracy.
The ripple effect was also felt among other managed care stocks, as investors adjusted their revenue and profitability expectations for 2027.
However, the impact on UnitedHealth is particularly pronounced due to its expansive reach.
As the company serves millions of Medicare Advantage enrollees and gains a considerable portion of its revenue from CMS payments, any shifts in federal reimbursement rates will have a significant influence on its financial projections.