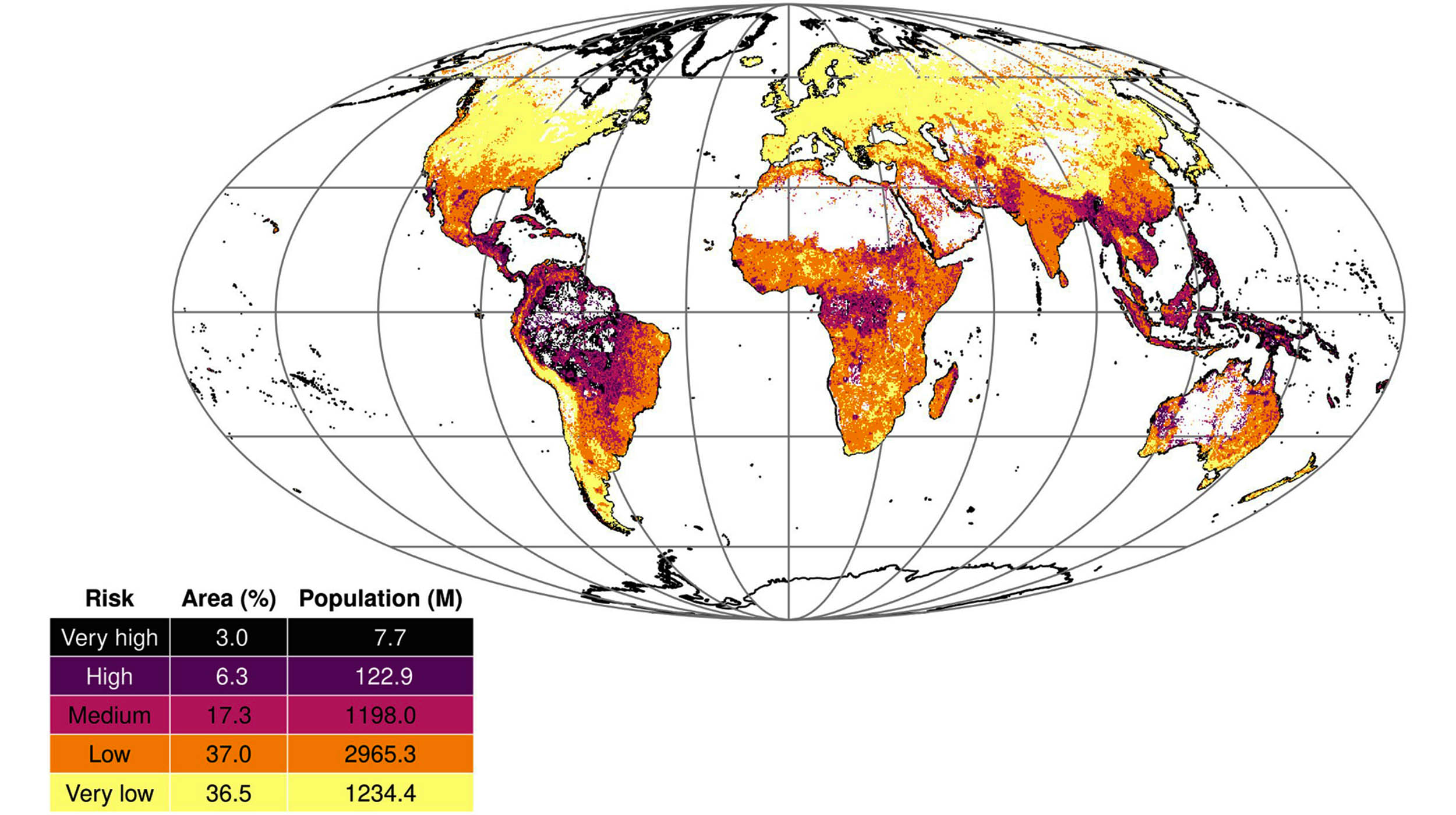
Global Land Vulnerability to Disease Outbreaks
Recent global modeling suggests that roughly 9.3% of the world’s land is at a high risk for disease outbreaks. This risk is particularly evident in regions of Latin America and Oceania, areas already struggling with the impacts of climate change and development pressures.
The research highlighted which countries are most susceptible to outbreaks and noted those that lack the necessary tools to detect and manage them.
Insights from the Disease Risk Map
Using machine learning along with satellite data, researchers created a comprehensive map of diseases that are prone to outbreaks across nearly every nation. Angela Fanelli, a veterinary epidemiologist at the European Commission’s Joint Research Centre (JRC), led the study. Her focus centers on how environmental changes driven by human activity influence epidemic risks and challenge countries’ crisis response capacities.
The findings indicate that 6.3% of the global land area is classified as high risk for disease, with an additional 3% in the very high-risk category. About 20% of the population lives in areas of medium risk, while 3% are located in high or very high-risk zones.
Zoonotic Diseases and Associated Risks
A significant number of diseases identified in this mapping are zoonotic, meaning they are transmitted from animals to humans. Research suggests that up to 75% of new human infections originate in other animals. Expanding human settlements into forested areas or wildlife markets increases the likelihood of such diseases spilling over into human populations.
On this risk map, diseases prioritized by WHO are included among the monitored zoonotic threats.
Climate Influences on Disease Outbreaks
Changes in temperature and rainfall affect where various animals, insects, and viruses can thrive—essentially reshaping the landscape of infectious diseases. The modeling indicates that rising temperatures, heavier rains, and intensified droughts elevate outbreak risks. Studies have linked climate change to shifts in migration patterns, breeding habits, and habitats that bring wildlife closer to human populations. This can create breeding grounds for disease-carrying mosquitoes and ticks, enabling tropical diseases to spread to higher latitudes.
The Impact of Human Land Use
Activities such as deforestation for agriculture, roads, and mining increase contact between humans and wildlife that might carry harmful viruses. Denser populations and industrial farms can accelerate the rapid spread of diseases. Moreover, a decline in biodiversity can sometimes favor species that harbor dangerous pathogens. Notably, population density emerged as the predominant factor influencing outbreak risk, surpassing any specific environmental condition.
Preparedness and Infrastructure Disparities
To transform hazard levels into tangible risks, researchers created an epidemic risk index that pairs the likelihood of outbreaks with each region’s ability to respond. Countries like Papua New Guinea and the Republic of Congo face severe risks paired with limited health infrastructure. This framework doesn’t assign blame; rather, it highlights where healthcare facilities and personnel might struggle during fast-paced outbreaks.
Many wealthier nations show low outbreak risks yet have robust health capacities, which could allow them to offer assistance in vaccine production and laboratory support.
Understanding the Implications of High Disease Risk
Even if one resides far from a recognized hotspot, the occurrence and timing of outbreaks can significantly impact travel patterns and trade. Quick air travel can transport infected individuals across continents in mere hours, but the ability of health systems to respond effectively plays a crucial role in managing such risks. Many individuals live in areas assessed as having moderate risk, which implies that local healthcare resources could be stressed during a severe outbreak. Being prepared encompasses more than just having hospital beds; it also involves early detection of diseases, clear communication, and dependable vaccine access.
Predictive Models for Anticipating Crises
Computer modeling that analyzes past outbreaks can pinpoint regions where dangerous viruses are likely to emerge. In this study, algorithms utilizing satellite data, climate records, and land use maps estimated potential future outbreak locations. Another investigation assessed virus families by their pandemic potential, aiding governments in discerning which vaccines might need to be developed proactively. While these tools cannot specify which virus will surface, they help narrow down possibilities to focus surveillance efforts and stock supplies.
Preparing for Unknown Threats
The WHO consistently revises its priority list to include unforeseen threats, referred to as Disease X, and promotes flexible preparedness strategies. In Europe, the Health Emergency Preparedness and Response Authority emphasizes climate-sensitive threats such as Ebola and Zika. Collaborative efforts in surveillance data, vaccine platforms, and rapid financing can allow protective measures to be taken quickly in response to outbreaks arising in one country.
This ominous map serves as both a warning and a planning tool, indicating where preventive support is necessary before outbreaks take hold. The research has been published in the journal Science Advances.