In Washington, some parents in Denver received texts this winter featuring videos that highlighted why families in their neighborhoods opted for flu vaccinations for their children. It was part of a unique study aimed at understanding trust and vaccine uptake in a historically Black community.
However, the project faced an abrupt stop when the Trump administration canceled it before researchers could analyze the collected data. Many, including those involved in the study, are frustrated by this decision.
“For someone like me from the Black community, particularly from the lower-income side, we often feel voiceless,” shared Denver mother Chantyl Busby, a community advisor for the study. “Losing funding for this project sends a really bad message. It’s like being reminded that our opinions don’t hold much weight.”
The urgency around discussing vaccines is clear—this flu season has seen at least 216 children in the U.S. succumb to the virus, marking the highest pediatric death toll in fifteen years, according to the CDC. Moreover, unvaccinated kids are contributing to significant measles outbreaks, with another vaccine-preventable illness, whooping cough, also on the rise.
Compounding concerns, Health Secretary Robert F. Kennedy Jr. is raising doubts about vaccines that have long been validated as safe and effective. The moves by the Trump administration create uncertainty over the availability of COVID-19 vaccines for the upcoming fall and have drastically cut funding for public health and medical research, abruptly halting investigations into vaccine hesitancy.
“We need to grasp what’s driving this resistance to vaccines and why,” remarked Michael Osterholm, who leads the Center for Infectious Disease Research and Policy at the University of Minnesota. He fears the country is slipping into a “scientific dark age.”
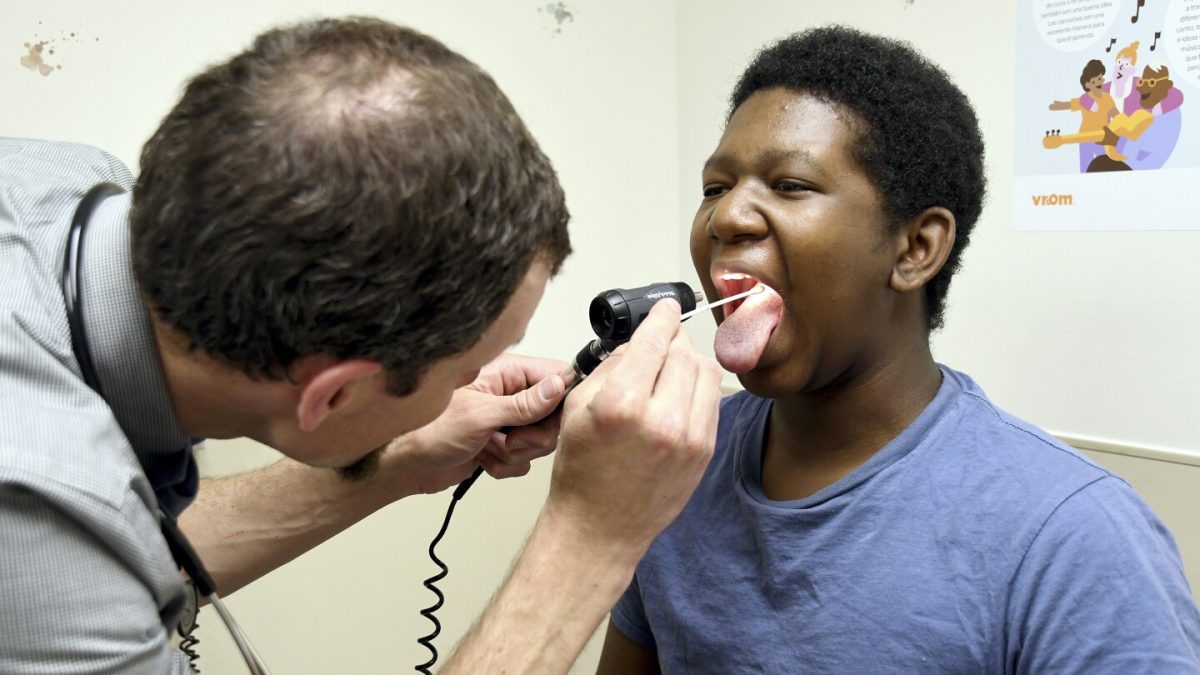
Dr. Joshua Williams, a pediatrician at Denver Health, engages in daily conversations with parents who have concerns or confusion about vaccines. Some even worry that they could be removed from his practice for refusing immunizations.
But Williams reassures them: Trust is built over time.
“The most gratifying interactions I have are with families who, after significant concern, eventually came to trust me through years of care for broken bones and ear infections—and ultimately decided to vaccinate their child,” he explained.
In this digital age, Williams pondered whether stories shared through video could assist in vaccine decision-making. He picked flu vaccines for this test—just under half of U.S. children received theirs this season, and Black children face higher risks from influenza.
With funding from the National Institutes of Health, Williams collaborated with Denver’s nonprofit Center for African American Health to organize workshops where volunteers could discuss their personal experiences with influenza and the flu vaccine. Professionals supported those who wanted to create 2- to 3-minute polished videos.
After engaging with the community for two years, five videos were included in a pilot study that sent text messages to 200 families visiting two Denver Health clinics.
In one video, a mother shared how she made the decision to get her first flu shot alongside her young daughter, breaking free from a controlling relationship. Another featured a grandmother vowing never to miss a vaccination appointment after her grandson was hospitalized due to the flu on his fourth birthday.
“Seeing people who look and sound like you, who share similar experiences, saying, ‘I felt as you did, but this changed my life,’ that’s incredibly impactful,” noted Busby, who chose to vaccinate her kids after engaging with Williams during multiple checkups.
The study’s unexpected cancellation means Williams can’t determine whether the videos swayed families’ decisions about vaccinations—resulting in lost data from over two years of effort and NIH funding. It also puts researchers’ careers in jeopardy. As they consider their next steps, Williams has sought permission from community members to use some videos in his practice while discussing vaccinations.
Williams also shares personal anecdotes, mentioning how his children are vaccinated and how his 95-year-old grandmother recalls the fear of polio in her childhood before vaccines were available.
“We’ve lost touch with the collective memory of living with these diseases in our communities,” Williams lamented, highlighting the ongoing measles outbreak. “I believe it will require a united voice from the community emphasizing the importance of vaccination to remind those in power about the need for resources in infection prevention and vaccine research.”