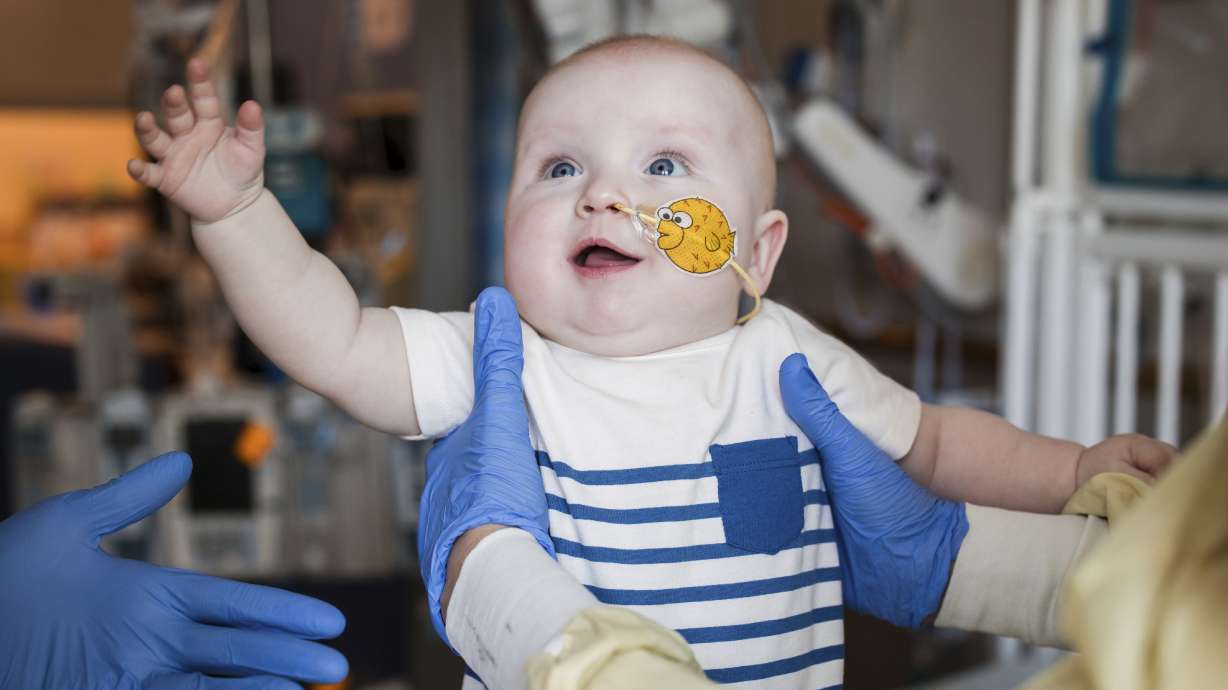
Baby Thrives After Experimental Gene Editing Treatment
PHILADELPHIA — A baby diagnosed with a rare and serious genetic condition is thriving thanks to a groundbreaking gene editing therapy tailored specifically for him.
In a new study, researchers reported that this baby is one of the first to undergo a personalized treatment aimed at correcting a crucial error in his genetic code. This error leads to severe outcomes, as it affects about half of infants diagnosed with the condition. Although it may take time before similar therapies are accessible to others, medical professionals are optimistic that this technology could eventually assist the millions still awaiting solutions for their rare conditions.
“This marks a significant initial step toward utilizing gene editing for a variety of rare genetic disorders that currently lack effective medical treatments,” mentioned Dr. Kiran Musunuru, a gene editing authority from the University of Pennsylvania, co-author of the study published in the New England Journal of Medicine.
The infant, KJ Muldoon, hails from Clifton Heights, Pennsylvania, and is part of the estimated 350 million people globally who suffer from rare diseases, many of which are genetic. Shortly after his birth, he was diagnosed with severe CPS1 deficiency, a condition believed to occur in roughly 1 in a million infants. This deficiency means these newborns do not produce an essential enzyme for ammonia removal from the body, leading to toxic build-up. Some of these cases may require a liver transplant.
Understanding KJ’s dire situation, his parents, Kyle and Nicole Muldoon, both 34, were understandably anxious about losing their son.
“We were weighing our options, asking a lot of questions about the liver transplant, which is quite invasive, or this untested treatment,” Nicole explained.
“We prayed, consulted with others, gathered information, and ultimately decided this was the right path for us,” Kyle added.
Within half a year, the team at the Children’s Hospital of Philadelphia and Penn Medicine partnered to develop a therapy aimed at fixing KJ’s genetic mutation. They employed CRISPR, the highly acclaimed gene editing tool that earned its inventors a Nobel Prize in 2020. Rather than cutting the DNA strand like earlier CRISPR methods, the doctors used a technique called “base editing” to flip the faulty DNA “letter” to the correct one, minimizing the likelihood of unintended genetic alterations.
The rapid development of KJ’s therapy is indeed “very exciting,” remarked Senthil Bhoopalan, a gene therapy researcher at St. Jude Children’s Research Hospital in Memphis, who was not part of the study. “This really sets a new standard for these types of treatments.”
KJ received his initial IV infusion of the gene editing therapy in February, delivered in tiny lipid nanoparticles that liver cells can absorb.
On that day, the excitement in the room was palpable, although “he slept through the entire procedure,” remembered Dr. Rebecca Ahrens-Nicklas, a gene therapy specialist at the hospital.
After follow-up doses in March and April, KJ has begun eating more normally and has recovered effectively from minor illnesses, such as colds, which can aggravate CPS1 symptoms. Now nine and a half months old, he also requires less medication.
Given his grim prognosis earlier, “every small milestone he meets—like waving or rolling over—is a significant moment for us,” his mother shared.
However, researchers caution that it has only been a few months since treatment, and they will need to monitor KJ for several years.
“We are still at the early stages of understanding what this therapy has done for KJ,” Ahrens-Nicklas advised. “Yet, every day, he provides evidence that he’s growing and thriving.”
The hope is that insights gained from KJ’s case can benefit others suffering from rare diseases.
Gene therapies are usually pricey to develop, mainly targeting more common disorders due to financial reasons: a larger patient pool can lead to more sales, helping cover development costs and generating profit. For example, the first CRISPR therapy sanctioned by the U.S. Food and Drug Administration addresses sickle cell disease, a widespread and painful blood disorder.
Musunuru noted that his team’s research, partially funded by the National Institutes of Health, demonstrated that crafting customized treatments need not be excessively costly. He mentioned that the expenses for KJ’s therapy were “not far off” from the average cost of a liver transplant and associated care, estimated at over $800,000.
“As we continue to improve our techniques and shorten development times, we expect costs to decrease as economies of scale come into play,” Musunuru predicted.
Bhoopalan added that researchers won’t need to repeat all preliminary work each time they create a custom therapy, suggesting that this research lays groundwork for addressing other rare conditions.
Carlos Moraes, a neurology professor at the University of Miami who did not participate in the study, noted that research like this paves the way for further innovations.
“Once a breakthrough like this emerges, it won’t take long for other teams to build on these findings,” he asserted. “There are hurdles, but I believe they will be overcome within the next five to ten years, propelling the entire field forward.”