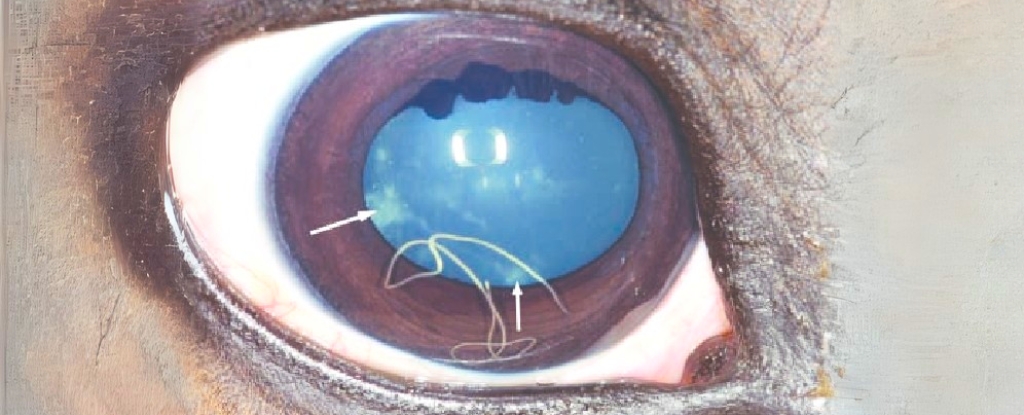
The Perils of Brain Worms in Moose Populations
A moose wandering in Minnesota finds herself lost on the road. She seems dazed, unable to grasp her surroundings, especially as a large semitruck approaches. It’s the crash that ultimately takes her life, but the reasons behind this tragedy are much more complex. A parasitic worm, often termed the brain worm, has made its way through her brain, sealing her fate and that of the truck as well.
The creature in question, Parelaphostrongylus tenuis, is a parasitic nematode that targets a wide array of wild and domestic herbivores, including moose and elk. Once it infiltrates the brain of an unsuspecting animal, it can lead to severe neurological issues and, tragically, death.
Though this specific moose is hypothetical, the effects of this worm have been profoundly damaging in real-life instances. Symptoms can vary considerably; some animals might show disorientation, while others might struggle with paralysis or even an inability to stand.
As parasitologists, we’re delving into how these worms impact moose populations in Minnesota. Understanding the spread of such parasites is crucial for wildlife managers, as it helps them protect these populations and limit transmission to other creatures, including livestock.
Interestingly, white-tailed deer can carry these worms without showing any signs of illness. This scenario creates a tricky situation for vulnerable species like moose and elk, which lack the necessary adaptations to cope with the parasite. However, monitoring the disease in wild populations proves to be a complex task.
Understanding the Disease Cycle
White-tailed deer are known to shed the parasite into their environment through their feces. Snails and slugs then become hosts, harboring the larvae until they’re capable of infecting other animals, such as deer, moose, elk, and even cattle.
For researchers like us, the major hurdle is identifying the disease before it severely damages its host. Since only white-tailed deer shed the parasite, we can’t simply analyze feces from moose or other animals to detect it.
By the time an animal shows visible signs of illness, it’s usually too late for recovery. Diagnosing typically requires examining the body post-mortem to find where the parasite has embedded itself within the brain or spinal cord. However, locating a single, threadlike worm amidst the vast nervous system of a moose can be very challenging. Often, biologists base their diagnosis on microscopic evidence that suggests a parasite’s migration, along with analyzing any DNA fragments left in its wake.
Challenges in Diagnosis
Complicating matters, signs of diseases caused by other parasites, like the arterial worm Elaeophora schneideri, can resemble those of brain worm disease, potentially leading to confusing diagnoses. This particular worm typically resides in the necks of specific deer species. It, too, can inflict damage in hosts that aren’t adapted to it.
For biologists trying to identify the issue based solely on visible symptoms, it’s easy to mix up these parasites and mistakenly deduce which one is responsible for the animals’ illnesses. Given the differences in how the parasites spread, employing the right mitigation steps becomes crucial.
Even when relying on microscopic analyses, there’s still a risk of misidentification. The most reliable method for accurate diagnosis involves genetic analysis, which can determine if the infectious agent is P. tenuis or E. schneideri.
Advancements in Testing
While genetic analysis is valuable for monitoring disease presence in populations, it isn’t effective for diagnosing living animals. However, our team, along with experts from the University of Tennessee’s molecular diagnostic lab, has developed a serological test to help identify affected animals while they are still alive.
This innovative test detects specific antibodies produced in the blood of moose or elk that have contracted brain worm. When wildlife health specialists collect blood samples from sick or recently deceased animals, these samples are analyzed for the presence of antibodies against P. tenuis, minimizing the chances of misdiagnosis.
This test, currently in use for samples sent from various regions, has significantly improved our ability to monitor moose and elk populations for infections. Not only can it detect the presence of the parasite in live animals, but it also avoids the high costs associated with genetic testing.
Wider Implications of Testing
After the incident involving the moose in Minnesota, wildlife officials collected her blood for testing. This sample, along with many others from across North America, aids researchers in refining their diagnostic procedures.
These tests can also screen blood from animals in areas not previously associated with P. tenuis. A positive result might indicate that the parasite is spreading and facilitate management decisions for animal populations.
If the tests reveal the parasite in a new region, wildlife managers gain a crucial window of time to intervene and attempt to prevent further spread. This might involve strategies such as reducing local snail and slug populations or adjusting hunting regulations for white-tailed deer.
Looking ahead, we hope other researchers adopt the approach behind this serological test to devise similar solutions for other infectious agents containing RNA or DNA.