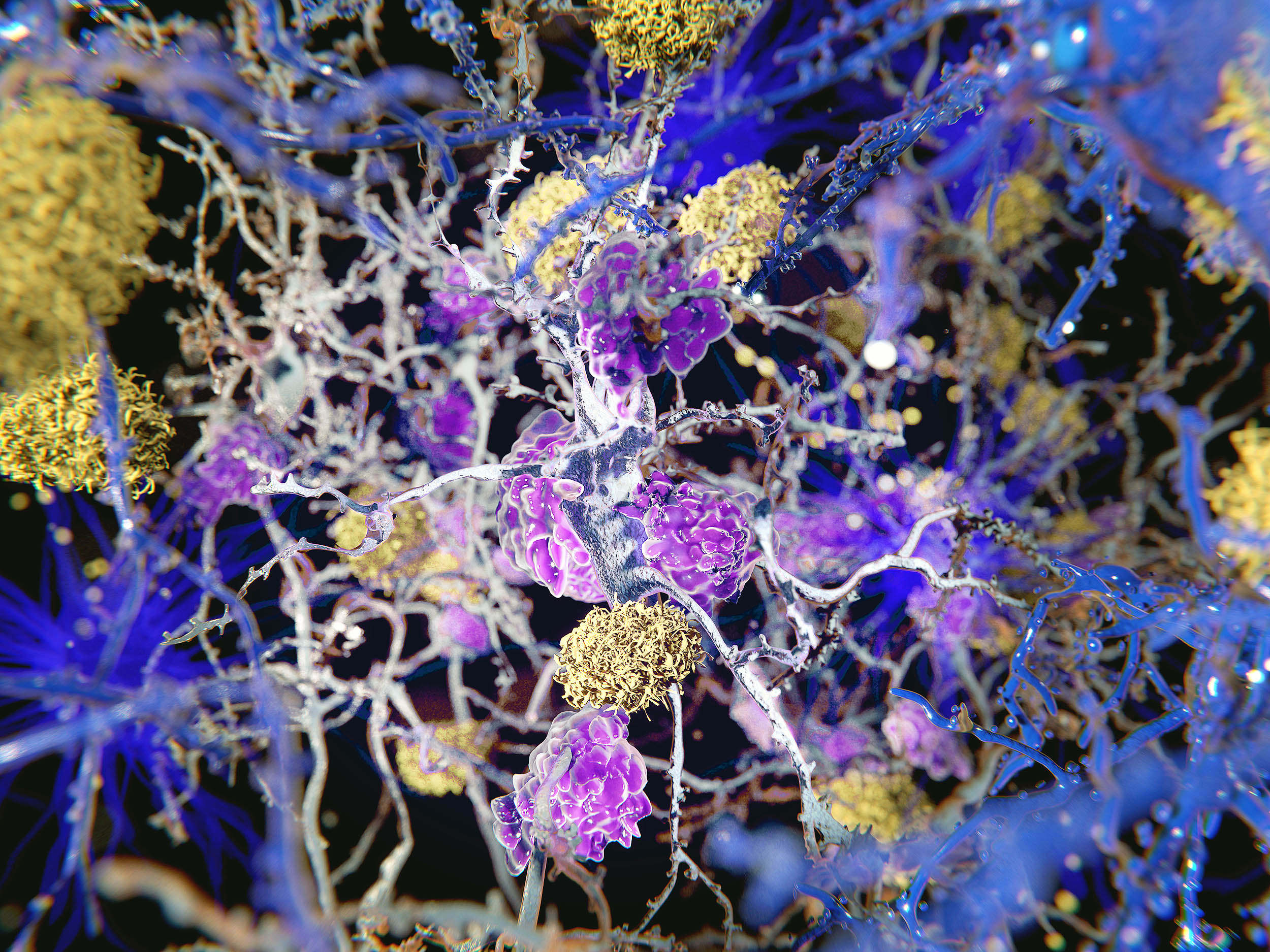
Alzheimer’s is typically seen as a disease that primarily affects the brain: with misfolded proteins accumulating, neurons being damaged, and memory deteriorating. However, a new genomic study suggests a different origin.
Rather than starting in the brain, initial triggers for Alzheimer’s might come from inflammation in “barrier” organs like the skin, lungs, or gut.
This inflammation could begin many years before someone experiences memory loss or disorientation.
If this analysis is accurate, it may shed light on a long-standing question that has puzzled families and researchers alike: why have many Alzheimer’s medications often fallen short?
Many treatments target amyloid or tau proteins once the disease is already advanced. This new perspective suggests we could be responding too late – tackling the symptoms while neglecting earlier causes.
Inflammation and Alzheimer’s Risk
This broader perspective isn’t entirely new. Increasing evidence points to a link between immune system activity and inflammation with the risk of dementia.
What’s novel here is both the depth and precision of this research. The team investigated Alzheimer’s risk genetics across various tissues and cell types, revealing that a significant portion of the relevant signals exist outside the brain.
Led by César Cunha at the Novo Nordisk Foundation Center for Basic Metabolic Research in Denmark, the team analyzed a vast dataset.
They compared genetic information from over 85,000 Alzheimer’s patients with around 485,000 individuals without the disease, utilizing data from the European Alzheimer and Dementia Biobank.
Next, they examined gene activity in approximately 5 million individual cells from 40 body regions and 100 brain regions.
This approach allowed the researchers to ask a straightforward question: where in the body are the genes associated with Alzheimer’s risk more active? They focused on about 1,000 genes linked to increased Alzheimer’s risk.
Risk Genes with Low Brain Signals
Interestingly, many of these risk genes had low activity in brain cells but displayed much higher activity in other organs, such as the skin, lungs, digestive tract, and spleen, as well as in immune cells in the bloodstream.
Cunha noted that he initially thought there must be a mistake due to the weak brain signal. However, upon re-evaluation and further analysis, the findings remained consistent.
A considerable amount of genetic risk for Alzheimer’s seems to be predominantly communicated through the immune system and organs that routinely interact with external factors.
This is significant because many of these genes are linked to controlling inflammation.
Inflammation in Barrier Tissues
The study identified that many of these risk genes were particularly abundant in barrier tissues like the skin, lungs, and gut.
These organs are constantly engaged with microbes, allergens, toxins, and other irritants. They are designed to respond with inflammation, which can sometimes become chronic or excessive.
This suggests that genetic variations might determine how intensely someone’s body responds to infections or inflammatory triggers in these areas, potentially leading to brain involvement over time.
In this context, a person carrying certain genetic risk factors may be more prone to a “chain reaction” initiated by something non-neurological, like a lung infection or gut inflammation.
The cognitive decline could manifest years down the line.
The Inflammation Link to Alzheimer’s
The timing of these findings is intriguing. The highest activity of Alzheimer’s-related variants was observed between ages 55 and 60.
This suggests midlife might be a crucial time when inflammation could have lasting impacts.
This aligns with earlier studies; for example, research in Hawaii indicated men with elevated inflammatory markers in their late 50s were more likely to develop Alzheimer’s later in life.
Cunha posits that a significant inflammatory event in late middle age, such as a viral infection, could trigger processes that only reveal themselves as dementia decades later.
Yet, he emphasized that the exact mechanism remains unclear, leaving many parts of this puzzle unsolved.
Genes Aren’t Destiny
Other scientists are observing similar patterns. Rezanur Rahman from QIMR Berghofer Medical Research Institute in Australia discovered that Alzheimer’s-linked variants also appear to cluster in the skin and lungs.
However, he cautioned that just because there’s a genetic association doesn’t mean those genes are directly causing the disease. The pattern is intriguing, but it’s not definitive evidence yet.
This study reinforces a hypothesis without cementing a conclusion.
Shifting Alzheimer’s Focus to Inflammation
The challenge now is persuading the Alzheimer’s research community to broaden its focus. Cunha describes how amyloid has dominated discussions in the field for years – to the extent that anything outside this narrative can be dismissed as irrelevant.
This scientific inertia makes sense; after all, shifting gears after focusing on one mechanism for decades can be quite challenging.
However, these new findings support an evolving perspective: Alzheimer’s might be less about being a brain-centric disorder and more like a lengthy, systemic issue where the brain is only where the damage eventually becomes noticeable.
If that holds true, the most critical periods for prevention could occur long before any memory tests show abnormalities.
A preprint of the study has been published in MedRxiv.