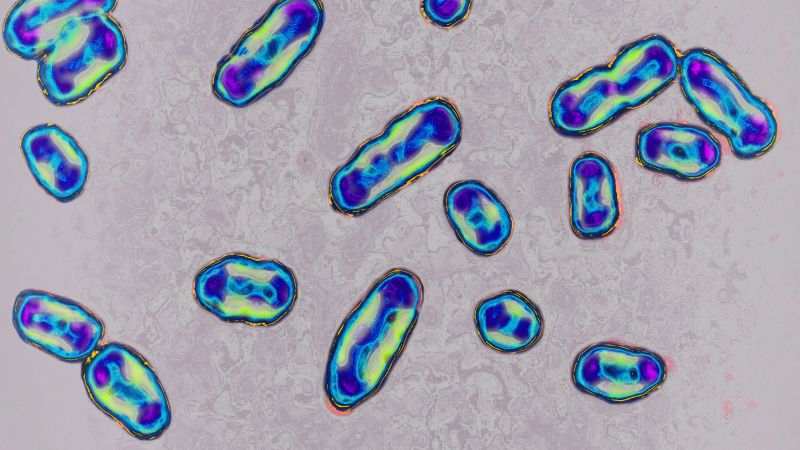
One of the darkest times in medieval Europe was marked by the plague pandemic known as the Black Death, which claimed at least 25 million lives in just five years. But the story didn’t end there. The plague made some adaptations to ensure its survival, allowing it to continue infecting people for centuries. Researchers have recently uncovered how this adaptation occurred.
The disease stems from the bacterium Yersinia pestis. It’s been around in human populations for at least 5,000 years and has caused three major plague pandemics since the first century AD. Although its most lethal years are seemingly behind us, cases still arise sporadically in Asia, South America, and the U.S., and more frequently in parts of Africa. Fortunately, it can be treated with antibiotics, according to the Cleveland Clinic.
Scientists are actively researching how Y. pestis evolved over time, and a recent analysis of both ancient and modern specimens has provided insights. It appears that, following a surge in infections and rapid deaths—where symptoms could lead to death within three days—mutations in a single gene produced new strains that were less lethal but more transmissible. This was detailed in a study published in the journal Science.
Interestingly, the original weaker strains eventually disappeared. The study indicated that today’s prevalent lineage of Y. pestis is the more virulent variety. Nevertheless, understanding how these historical adaptations occurred could be crucial for managing modern-day plague outbreaks.
Bubonic plague, the most familiar form of the disease, leads to painful lymph node swellings and spreads through flea bites from infected rats. The outbreak from 1347 to 1352 in Europe famously wiped out about 30% to 50% of the continent’s population. Yet, the earliest recorded bubonic plague outbreak, known as the Plague of Justinian, affected the Mediterranean region between AD 541 and AD 544. Another major outbreak originated in China in the 1850s, leading to an epidemic in 1894. Today’s plague cases are often viewed as part of this third pandemic.
In the new study, researchers gathered ancient Y. pestis samples from human remains dating back around 100 years after the first two pandemics. They sampled remains from Denmark, Europe, and Russia. The genomes of these strains were reconstructed for comparison with older, ancient ones.
The team also analyzed over 2,700 genomes from modern plague samples across various continents. One coauthor, Jennifer Klunk, who is affiliated with a Michigan-based biotechnology company, noted that while they provided synthetic materials for the research, there were no financial interests involved.
Their findings indicated that the strains reconstructed from the earlier pandemics had fewer copies of a gene known as pla, which has long been recognized as a key factor contributing to the plague’s lethality, according to Ravneet Sidhu, a doctoral student involved in the study.
The pla gene encodes for an enzyme that interacts with host proteins, assisting Y. pestis in spreading to lymph nodes, where it replicates before moving on to infect the rest of the body. Interestingly, not all aspects of this gene’s functions are completely understood, but prior research has linked it to the severity of both bubonic and pneumonic plague, the latter affecting the lungs.
While their findings showed fewer pla gene copies, researchers were unsure about the direct implications for the disease’s deadliness. To investigate, they experimented with strains of bubonic plague that had reduced pla levels on mice and found that survival rates increased by 10 to 20 percent compared to those infected with strains that had standard levels of the gene. Furthermore, the modified bubonic strain took about two additional days to be lethal.
Dr. Deborah Anderson, a professor of veterinary pathobiology at the University of Missouri’s College of Veterinary Medicine, remarked that the study effectively illustrates how the depletion, rather than total loss, of the Pla enzyme during evolution might explain the decline of plague during the second pandemic commonly referred to as the Black Death. Her research dives into the virulence of plague, and this new information could enhance our understanding of transmission in current cases.
She explains how their lab studies the flea-rodent cycle and collaborates with field researchers in areas experiencing annual or occasional plague outbreaks. Nearly 300 rodent species can transmit Yersinia pestis, with burrowing rodents like prairie dogs currently viewed as primary hosts for outbreaks.
Mathematical models have suggested how these dynamics might have played out in human populations centuries ago, leading to what is termed “epidemic burnout” approximately a century after a bubonic plague outbreak.
In the beginning, infections spread rapidly, resulting in quick deaths among both rats and humans. Over time, as extremely dense rat populations thinned, evolutionary pressures favored less harmful strains of Y. pestis, which carried fewer copies of the pla gene. This meant that infected rats lived longer, allowing them more time to transmit the disease to others—potentially humans as well.
Anderson mentioned that these findings offer a model that could be further explored in lab settings to help explain modern plague spread in the wild.
Ultimately, the weaker strains of the disease fizzled out. In contemporary samples, researchers identified just three strains with reduced pla genes, found in Vietnam—one from a human and two from black rats.
Sidhu expressed excitement about the interdisciplinary nature of the study, combining modern and ancient data to draw insights from the plague’s long evolution. It could pave the way for future researchers to uncover similarities between modern and ancient pandemics, although such well-documented ancient pathogens are rare.
One unique aspect of plague pandemics is their ability to persist over time. Understanding how Y. pestis shifted its infection patterns could provide insights into the adaptability of contemporary pandemics like Covid-19, she noted. Even though the situation isn’t as severe as it was in 2020 or 2021, the pathogen continues to evolve and persist in the background.