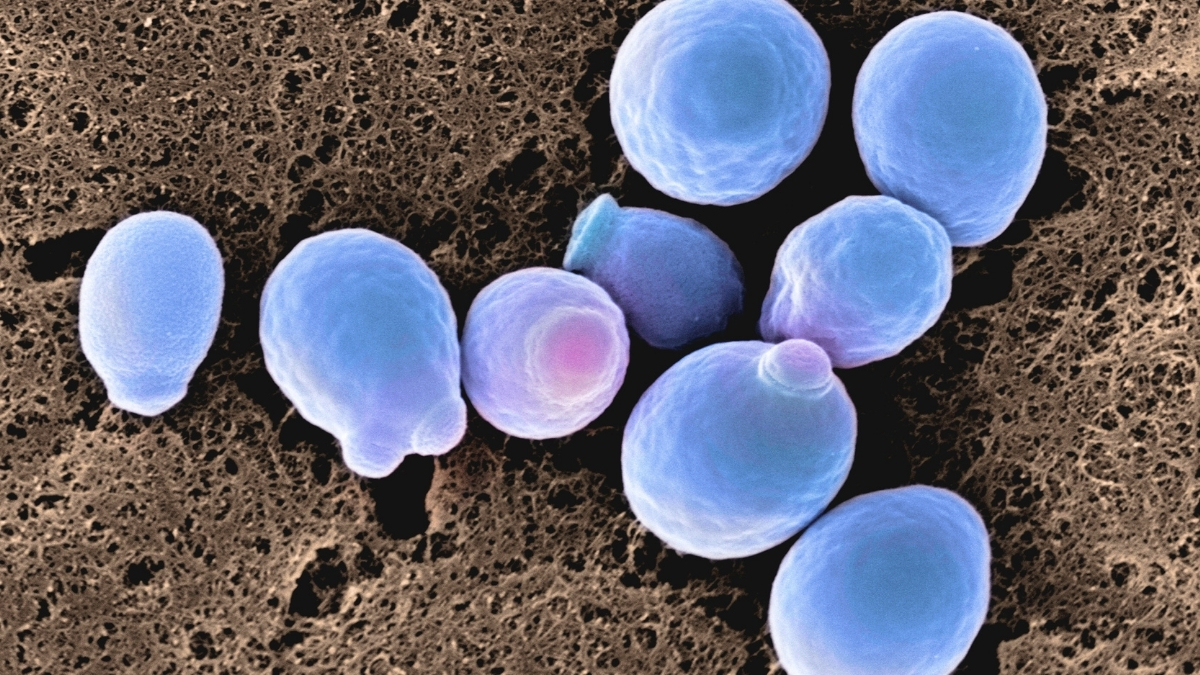
Thrush and Its Growing Resistance
Thrush is among the most prevalent infections globally, caused by fungi known as Candida, especially the yeast Candida albicans.
Typically, yeast infections are easily addressed with antifungal medications. However, an increasing number of Candida species are showing resistance to these treatments, including those responsible for thrush.
The US Centers for Disease Control and Prevention notes that approximately 7% of Candida blood samples exhibit resistance to fluconazole, the primary drug for treating most Candida infections.
This situation results in fewer available treatments for even standard thrush cases, complicating their management. Additionally, individuals with weakened immune systems or those on prolonged antibiotic courses may face more serious Candida infections that are tougher to treat.
There’s also a chance that rising antifungal resistance is linked to the increase in recurrent thrush (infections that keep reappearing), which currently impacts about 138 million women worldwide and is projected to reach 158 million by 2030.
Understanding the Rise in Resistance
The landscape of antifungal resistance has shifted markedly over the last few decades.
In the early 2000s, antifungal resistance was relatively uncommon. Fluconazole effectively treated most Candida albicans infections, with less than 5% resistant to it.
Yet, Candida albicans can easily adapt and develop resistance to antifungals when conditions are favorable.
Research indicates that resistance in Candida albicans has been increasing over the past eight years. A study conducted in Egypt revealed that by 2024, nearly 26% of Candida albicans isolates from blood samples were resistant to fluconazole.
More extensive research is necessary to determine if this trend is consistent worldwide.
Candida can develop resistance through genetic mutations, making it less responsive to antifungals or diminishing the drug’s effectiveness.
Additionally, they form protective biofilms—slimy layers of cells that prevent drugs from entering, help pump out any that do penetrate, and allow some cells to remain dormant until treatment ends.
Another way Candida resists treatment is by altering the structure of the molecules targeted by antifungals, hindering drug binding.
The primary issue is that these fungi are evolving to withstand antifungal medications.
This resistance isn’t random; it stems from several factors, including the misuse and overuse of antifungal drugs in both humans and agriculture, as well as the limited availability of effective antifungal treatments.
Environmental changes, such as rising temperatures and ecological strains, are also fostering conditions suitable for heat-resistant and drug-resistant Candida strains, like Candida auris, known for significant resistance to multiple antifungal classes and posing risks to immunocompromised individuals.
Strategies to Combat Antifungal Resistance
Candida primarily spreads through personal contact, sexual interactions, and contact with contaminated items or surfaces. It can also be transmitted in healthcare settings via contaminated medical devices.
Though airborne transmission is rare, a concerning study recently discovered common antifungal-resistant Candida species, including Candida albicans, in urban air samples from Hong Kong.
The presence of Candida in the air could enhance community spread and increase inhalation risks, particularly in hospitals or crowded spaces with vulnerable individuals.
This suggests a potential exposure pathway that may have been underestimated in the past.
Typically, Candida doesn’t pose significant harm in healthy individuals. Maintaining a balanced microbiome is crucial for protection: beneficial bacteria in the body help control Candida levels and prevent overgrowth.
However, factors like antibiotics, poor nutrition, weakened immunity, or high stress can disrupt this balance, allowing Candida to proliferate and lead to health issues.
Disruption of the microbiome can create a favorable environment for antifungal-resistant strains to thrive, making them more challenging to treat.
Taking care of your microbiome can significantly reduce the risk of Candida and other infections. This involves consuming a varied, fiber-rich diet—incorporating fermented foods—and limiting processed foods.
It’s important to use antibiotics judiciously and consider probiotics and prebiotics to help maintain microbiome balance, especially after antibiotic treatments or recurring infections.
While the majority of Candida infections can be treated effectively, drug-resistant strains present a serious challenge, particularly for susceptible individuals.
Preventative measures are key. This includes adhering to prescribed antifungal treatments, completing the full course, and practicing good hygiene.