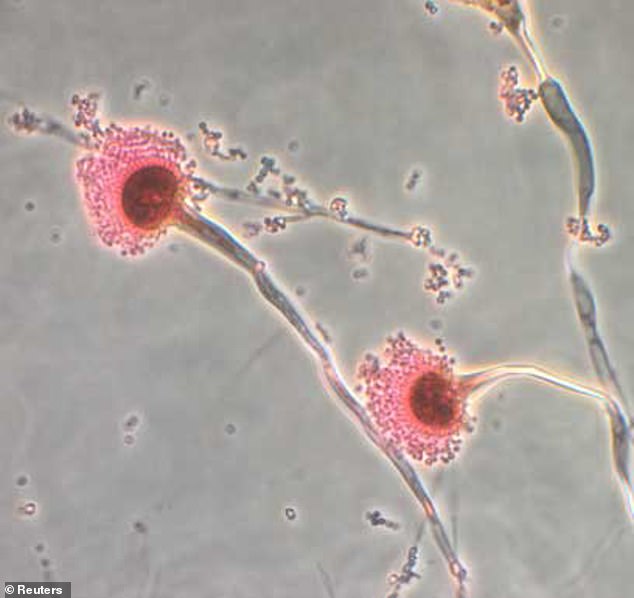
A dangerous fungus capable of damaging human tissue is rapidly spreading across the United States, and experts are concerned that the situation may worsen as temperatures rise.
Aspergillus fumigatus is an airborne fungus that’s nearly impossible to avoid—its spores are so minuscule that people can inhale them without even realizing it.
This fungus can lead to a severe lung infection known as aspergillosis, which, especially in vulnerable individuals, can result in organ failure or even death.
Those with weakened immune systems, such as cancer patients or individuals with asthma or HIV, are particularly at risk.
Recent studies have identified the fungus in various regions of the US, particularly in states like Florida, Louisiana, Texas, Georgia, and California where hot, humid climates and agricultural practices create ideal conditions.
Major urban centers such as New York, Houston, and Los Angeles are also under threat due to high population density and aging facilities.
It’s worth noting that aspergillosis isn’t classified as a reportable disease in the US, which means there’s a lack of tracking concerning infections, hospitalizations, and fatalities—making it difficult to understand the problem’s scope.
Doctors recommend that people with weakened immune systems steer clear of soil, gardening activities, and moldy environments, wear masks in dusty areas, and ensure good air quality in hospitals and homes. Hospitals have increased mold inspections and antifungal strategies.
Norman van Rhijn, a co-author from the University of Manchester, expressed in an interview that this issue could impact hundreds of thousands of lives, suggesting that the distribution of species and what poses an infection risk may change dramatically in the next 50 years.
Currently, around 400,000 cases evolve into chronic pulmonary aspergillosis, a long-term lung infection; however, invasive aspergillosis is rarer but significantly more lethal, primarily affecting those with weakened immune systems. This form can spread from the lungs to other organs, like the brain, heart, and kidneys.
One study highlighted that only about 59% of organ transplant patients survive a year after an infection, while just 25% of stem cell transplant patients do.
The number of hospitalizations related to invasive aspergillosis has seen an annual rise of approximately 3% from 2000 to 2013, with nearly 15,000 stays recorded by 2014, accumulating costs of about $1.2 billion.
Autopsies in ICUs indicate that aspergillosis is among the top four infections leading to fatalities.
The World Health Organization has labeled Aspergillus fumigatus as a “critical priority” fungal threat due to increasing drug resistance and high mortality rates.
This fungus thrives in warm and moist conditions, with the ability to survive temperatures exceeding 120 degrees Fahrenheit in compost heaps.
Climate change is making it easier for this fungus to thrive inside the human body as global temperatures continue to rise. A study from the University of Manchester warns that if fossil fuel consumption remains at current levels, the fungus’s prevalence could increase by over 75% by 2100, putting millions more at risk, especially in the southern US.
Additionally, azole medications commonly used for treating fungal infections in humans are heavily utilized in agriculture, which may lead to drug resistance that can transfer to humans and diminish treatment efficacy.
A study published in Applied and Environmental Microbiology detected azole-resistant Aspergillus fumigatus in farm soil across at least seven US states, with various strains resistant to typical antifungal treatments.
Scientists indicate that the mixing of various fungal species is accelerating the spread of resistance, highlighting that the issue is likely already deeply entrenched in US soil.
The WHO is calling for immediate investments in safer treatments, faster testing, and improved training for healthcare workers. They also urge pharmaceutical companies to prioritize research on fungal infections and include children in clinical trials.
Dr. Vyas, an infectious disease expert at Columbia University, remarked, “This isn’t science fiction. These infections are real, and we’re not prepared.”