Valley Fever Epidemic Across the West Coast
Thousands of people in the U.S. are facing an incurable fungal infection on the West Coast, which has been described as a new ‘epidemic.’
This condition, known as Valley Fever, is predominantly found in Arizona and California. It’s a serious lung infection, with a mortality rate of about one in a hundred for those who contract it.
In California, cases have surged by over 1,200 percent in just 25 years. During the first half of 2025 alone, more than 5,500 provisional cases were reported in the state. Health experts are expressing concern that if the trend continues, it could surpass last year’s peak of nearly 12,500 cases.
Arizona has also seen a significant rise, with over 14,000 reported cases in 2024, reflecting an increase of more than 27 percent from 2023.
On a national level, Valley Fever cases are reaching new highs, expected to approach 30,000 by the end of 2025.
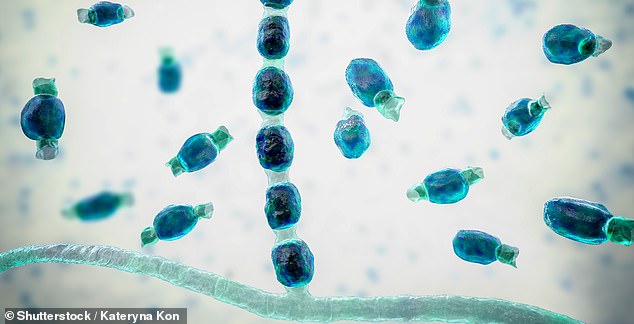
The disease is caused by the fungus Coccidioides, which releases spores into the air when soil is disturbed. Experts suggest avoiding dusty outdoor areas to reduce the risk of inhaling these spores.
Interestingly, the number of cases hit a decade-high in 2021, with 20,970 instances recorded—the most since 2011. Although cases dipped in 2022, they picked up again the following year. This uncertainty about future trends has led to concerns about an increase in infections over the next few decades.
The CDC warns that future projections could see more than half a million Americans infected yearly due to rising global temperatures, which may expand the regions where the fungus thrives.
Dr. Erica Pan from the California Department of Public Health emphasized the seriousness of Valley Fever, noting the escalating case counts. She urges Californians, as well as visitors, to be vigilant about recognizing potential signs and symptoms early.
It’s important to note there is no person-to-person transmission of Valley Fever, and no vaccine currently exists. While many infections resolve without treatment, antifungal medications may be necessary for more severe or persistent cases.
Symptoms can often mimic those of pneumonia—fatigue, cough, fever, and muscle aches, among others—making misdiagnosis a common issue. According to the CDC, the true incidence of infections could be significantly higher than reported data suggests.
Severe cases, approximately 10 percent of infections, can lead to disseminated coccidioidomycosis, where the infection spreads to other parts of the body and can even cause life-threatening conditions like meningitis.
Dr. Pan recommends consulting a healthcare provider if symptoms persist for more than a week, especially after exposure to dusty environments.
Over the years, climate changes—wet winters followed by dry, windy conditions—have been linked to the rise of Valley Fever. Experts believe the current patterns indeed favor the fungus’s proliferation.
While there is no guaranteed treatment, patients typically receive supportive care to manage symptoms. Some antifungal medications may be prescribed, although their effectiveness remains in question.
The Valley Fever Center for Excellence at the University of Arizona was established in 1996 to tackle challenges posed by the Coccidioides fungus. A significant portion of infections occur in Arizona, particularly in urban settings around Phoenix and Tucson.
Recently, the University secured funding to pursue a vaccine, initiated by Dr. John Galgiani, who has been developing a vaccine for dogs, hoping that success could lead to human applications as well.
Dr. Galgiani mentioned, “Taking this through the dog is a useful step to validate the idea for human use, making it more plausible.”