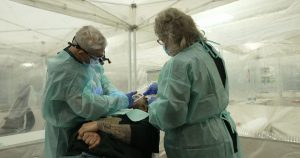
During the COVID-19 pandemic, Erin Booth's 5-year-old son was diagnosed with leukemia. She and her husband qualified for Medicaid under a program enacted during the health crisis, and federal insurance provided all the medical care and therapy Landon needed.
Chemotherapy damaged Landon's still-developing brain and body, requiring an army of specialists to overcome his developmental problems. He went to speech, physical, and occupational therapy almost every day.
But after President Joe Biden declared an end to the public health emergency, the Orlandos' son lost Medicaid coverage, as did about 600,000 other children in Florida. All were eligible under a “special exemption” enacted during the pandemic, but lost their eligibility when it ended under a process known as “rewind.”
The state directed Booth to KidCare. KidCare is a federally funded children's health insurance program run by states that provides low-cost health insurance to families who cannot afford private insurance but earn too much to qualify for Medicaid.
But the Booths also say their incomes are too high to qualify for the program's cheaper, subsidized plans, which puts a strain on their finances as they have to pay the full amount and can only cover basic medical care. Currently, 9-year-old Landon cannot receive all the treatment he needs.
“It only covered eight therapy sessions and they were finished,” his mother said. “He hasn't received the services he needs for a year now.”
Florida's law, which was scheduled to go into effect Jan. 1, would provide better coverage at much lower rates, but would allow the state to exclude children from health insurance if their parents miss out on health insurance. The state has been slow to implement it because it is battling federal regulations that prohibit it from doing so. payment.
Florida could expand KidCare to an estimated 42,000 additional children if it complies with federal rules, but the state announced earlier this month that the administration may not insist on that provision. He announced that any action would be postponed until President-elect Donald Trump takes office.
The rule prohibits states from cutting off a child's insurance for 12 months even if the parent fails to pay premiums. Florida is the only state to challenge it.
During that time, an average of 5,500 children are removed from Kid Care each month due to unpaid bills, state records show.
“Florida has kicked more than 500,000 children off Medicaid, and thousands more now have no health insurance because of this delay,” said Georgetown University's McCourt School of Public Policy, executive director of the Center for Children and Families. Joan Alker says. “Texas is the only state that has had more kids canceling than Florida.”
Florida also has one of the highest rates of uninsured children in the nation, at 7.5% in 2023, according to the Child Health Report Card. Florida ranked 47th out of 51 states and Washington, D.C., according to the report.
Check out the top stories in Tampa Bay
Subscribe to the free DayStarter Newsletter
We'll send you the latest news and information you need to know every morning.
Everyone is registered!
Want more free weekly newsletters sent to your inbox? Let's get started.
consider all options
“While Florida is not the only state to disenroll children from Medicaid during the mitigation process, it has the distinction of being the only state to violate federal law by displacing families,” Alker said. he said.
While other Republican-dominated states, including Arizona, adopted the federal rules and quickly expanded children's health insurance programs, Florida is challenging the regulations and saying they are excluding children from its rolls. she stated.
Erin Booth said the Booths – she a drug store manager and he an electrician – never missed a $260 monthly premium on their insurance, even if it meant deferring their electric bill. He says it never happened.
“Kids like my son need insurance to survive,” Booth said.
Anticipating a large wave of low-income families losing Medicaid coverage during the lifting of mitigation, the state two years ago expanded Kidcare eligibility to people earning between $51,640 and $77,460 for a family of three. enacted a law to expand the
Under the law, Mr. and Mrs. Booth with incomes in that range could qualify for a subsidized plan for just $20 a month that would cover all the special services their son Landon needs.
But expansion has been delayed while the state challenges federal rules. The state of Florida sued to block the continuing enforcement rule, citing $13 million in administrative costs. A judge in Tampa dismissed the case, but Florida continues to exclude children from its insurance plans while it appeals the ruling.
After the Biden administration approved Florida's expansion plan earlier this month, subject to compliance with rules, state health officials decided to wait and see how the incoming Trump administration would respond. They are seeking a 30-day extension of the deadline to expand insurance coverage, and they continue to evict children for non-payment of insurance premiums.
The level of disenrollment in the state's Kid Care program has been so rapid that Amy, Florida's chief economic analyst, said she was listening to state health officials explain the steep decline at a revenue estimating meeting in July. It caught Mr. Baker's attention.
“Our estimates don't show this much of a decline, so that's normal,” Baker told Jeff Dykes, chief financial officer of the state's Children's Health Insurance Program.
He said state officials assumed that if the state disenrolled people from Medicaid, they would turn to KidCare. However, the numbers showed the number of Kidcare recipients had actually fallen by several thousand people.
Brian Blades, president of the Paragon Health Institute, is a conservative policy analyst who served as health advisor during President Trump's first administration and praised Gov. Ron DeSantis for resisting Medicaid expansion. Blaise argued that expanding Medicaid would have a “detrimental impact on health care” and lead to vast numbers of Floridians leaving private insurance and enrolling in the federal system.
Naomi Lublin doesn't think so.
“The state doesn't respect the needs of children who can't speak for themselves,” said Lublin, a funeral director and single mother who grew up in Orlando and recently moved to Plantation.
Lublin has watched her son Taj's symptoms regress after his Medicaid was discontinued six months ago in May.
After he was diagnosed with autism at 16 months old, they received Medicaid, underwent rigorous speech and occupational therapy, and received guidance from professionals, including a nutritionist, she said. He was seeing a therapist almost every day.
“If it's taken away, they only have 30 minutes of work to do,” she said.
Lublin said the therapist helped Taj overcome his aversion to solid foods and move away from eating only pureed foods.
“We started to see some improvement, but after treatment he regressed and stopped eating solid food,” she said.
The state recommended she enroll in KidCare, which would cost $500 a month just for basic medical care and did not require therapy sessions. “It costs that much to pay for a few therapy sessions a month out of pocket. KidCare has no benefit,” she added.
Taj hasn't had health insurance since the state canceled Medicaid in May. She had to wait for the enrollment period at work to enroll him on her insurance starting January 1st. Insurance costs $800 per month for two people.
“That's why I'm working overtime to make ends meet so he can get the treatment he needs,” Lublin said.