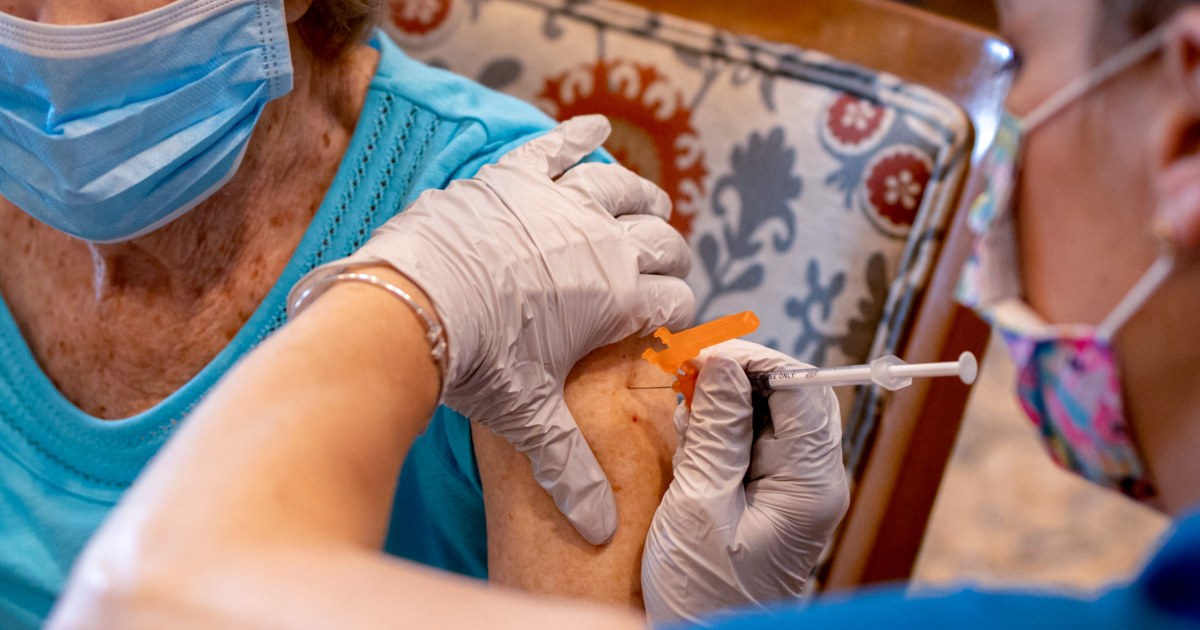
Challenges for Older Americans Seeking Covid Shots
Many older Americans enrolled in Medicare are encountering an unexpected hurdle: the newly approved Covid vaccinations aren’t being covered, leaving them to weigh the option of paying out of pocket.
Allison Engel, who is 74, visited her local CVS in Pasadena, California, just recently and found out the shot would cost her $225 if she paid out of pocket.
“They entered all my information and then handed me a rejection letter,” Engel recounted. “They said it wasn’t in the Medicare system yet and suggested I return in two weeks.”
Not wanting to wait that long, Engel opted to cover the cost herself, hoping that Medicare would reimburse her later.
Brant Mittler, age 78, from San Antonio, shared a similar story. When he and his wife visited their CVS pharmacy, they faced the same issue.
“The pharmacist told my wife, ‘We’ve had Medicare patients coming in all day. Everyone’s upset because we can’t provide them with the shot,’” Mittler explained. Ultimately, they received their Covid vaccinations after the pharmacist confirmed the Medicare system had finally updated.
Their experiences appear to contradict what Health Secretary Robert F. Kennedy Jr. stated during a Senate committee meeting, where he claimed most Americans would be able to get the Covid shot for free at their pharmacies. Kennedy oversees Medicare in his role as HHS secretary.
Last month, Kennedy announced that the FDA had approved updated Covid shots aimed at a more limited, high-risk population: those aged 65 and older and individuals with preexisting health conditions.
This limited approval has raised concerns regarding vaccine access for those outside of the high-risk groups, although it seems to be less of an issue for those who qualify.
“Anyone can get the booster,” he mentioned while addressing questions about restricted eligibility. “Most Americans should be able to get it at their pharmacy.”
Arthur Caplan, who leads the division of medical ethics at NYU Langone Medical Center, expressed concern about the difficulties eligible patients are having getting vaccinated, reflecting shifting policies from Kennedy.
“Medicare should be covering the shots, but it’s not processing people properly,” Caplan noted. “This creates confusion about eligibility and who falls into the risk category.”
The updated Covid vaccinations began arriving at major pharmacy chains last week. However, some states are choosing to hold off until the CDC’s advisory committee provides a recommendation on eligibility.
The CDC’s Advisory Committee on Immunization Practices usually convenes early in the summer to make vaccine recommendations, but this year, its meeting isn’t set until September 18.
Interestingly, Medicare doesn’t have to wait for the CDC’s approval. According to Dorit Reiss, a vaccine policy expert at the University of California, San Francisco, once the FDA greenlights a vaccine, Medicare can cover it.
CVS, one of the largest pharmacy chains in the country, stated that in 13 states and Washington, D.C., Medicare patients will need a doctor’s prescription until the ACIP offers its recommendations. In three states—Massachusetts, Nevada, and New Mexico—CVS won’t provide the Covid shot at all until ACIP acts.
“Some payers are still in the process of updating their systems and might not be ready to cover the updated Covid-19 vaccines,” said CVS spokesperson Amy Thibault regarding the Medicare patients experiencing coverage issues. “If that happens, our pharmacy teams can assist patients in scheduling an appointment for a future date.”
Walgreens did not respond to requests for comment on this matter.
A representative from the Centers for Medicare and Medicaid Services indicated in an email that they are investigating the situation.
“CMS continues to monitor developments related to COVID-19 vaccines,” the spokesperson added.