Increasing Resistance in Fungal Infections
Research released on Wednesday highlights a troubling trend: fungal infections are becoming increasingly resistant to existing treatments, as reported in The Lancet Microbe.
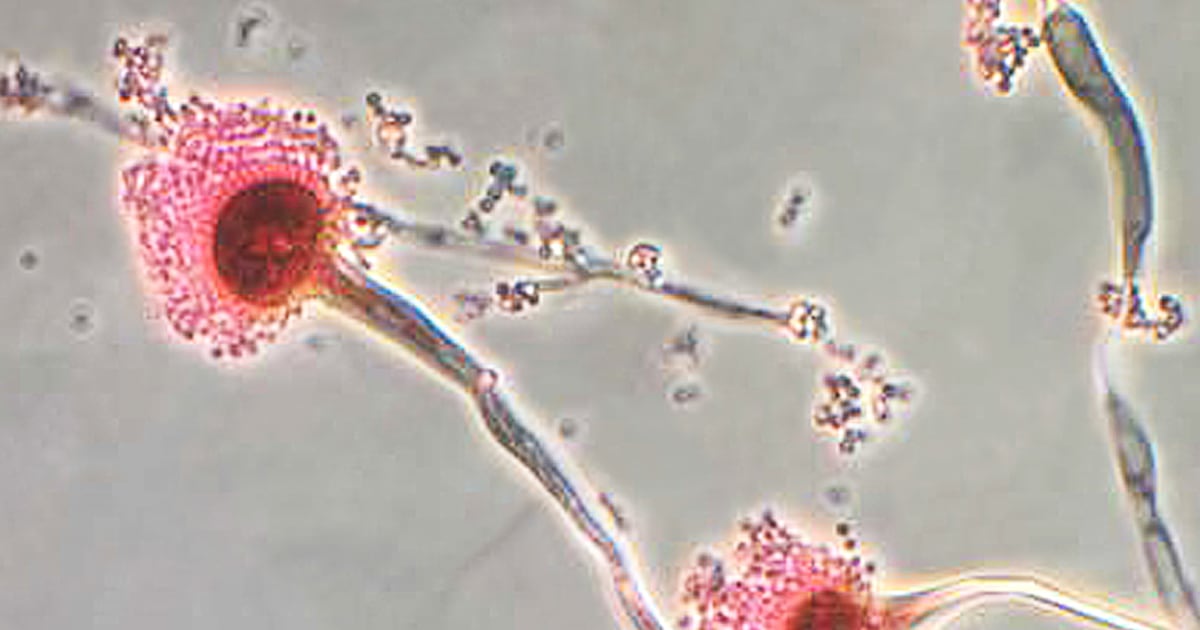
The study specifically examined infections resulting from Aspergillus fumigatus, a fungus commonly found in soil and decomposing organic material globally. Typically inhaled without issue, this fungus poses significant risks to individuals with weakened immune systems or underlying lung issues.
Aspergillus is listed among the World Health Organization’s priority fungi, and the mortality rate for those with drug-resistant infections can range from 47% to 88%.
The new findings indicated a rise in drug resistance among these fungi. Interestingly, many patients also appear to be dealing with multiple strains, some of which harbor different resistance traits.
“This creates significant challenges in treatment,” noted co-author Jochem Buil, a microbiologist at Radboud University Medical Centre in the Netherlands.
Buil and his team delved into over 12,600 Aspergillus samples collected from lung patients at Dutch hospitals over three decades. They discovered about 2,000 samples featured mutations linked to resistance against azoles, a primary class of antifungal drugs. While most mutations were of the well-documented varieties, approximately 17% showcased different mutations.
Of the nearly 60 patients with invasive infections, 13 were found to have azole-resistant strains. Alarmingly, about 86% of these individuals had multiple fungal strains, complicating treatment options.
“As the situation becomes more complex, doctors might struggle to determine whether they are face-to-face with a drug-resistant fungal infection,” said Dr. Arturo Casadevall from Johns Hopkins Bloomberg School of Public Health, who was not part of the study.
In treating Aspergillus infections, physicians typically check for resistance genes, which help in deciding the most effective medications. However, when several strains are involved, this process becomes much less straightforward. Different strains can react differently to treatments.
“Azoles are the first line for strains that are susceptible, but they aren’t effective against resistant strains. In those cases, alternative drugs that may not be as effective and have more severe side effects are required,” said Buil, pointing out that some patients may need a combination of antifungal medications.
This research underscores a broader issue: the limited arsenal of antifungal drugs compared to antibiotics, with only three main classes available for invasive infections.
Resistance to antifungals is rising, and developing new ones is particularly challenging. Given the genetic similarities between humans and fungi—about half of our DNA aligns—it makes it more difficult to find unique drug targets, as many essential proteins for fungi are also vital for human cells.
Jarrod Fortwendel, a professor of clinical pharmacy at the University of Tennessee Health Science Center, remarked on the challenge this poses: “Most resistance mutations affect more than one drug type, meaning you may lose an entire category of treatment.”
Furthermore, much of the azole resistance in Aspergillus fumigatus originates from agricultural practices, where fungicides are widely applied and share molecular targets with antifungal treatments. Farmers use these chemicals on crops like wheat and barley to fend off fungal diseases. This exposure inadvertently fosters resistance before antifungal treatments are even introduced to the market.
Fortwendel observed that this resistance is not confined to one region; it’s a growing concern globally. “Wherever we investigate, we find drug-resistant strains. The rates of azole resistance are on the rise in the U.S.,” he explained.
While the individual risk for contracts with azole-resistant Aspergillus fumigatus remains low, as noted by Casadevall, these infections usually impact those with weakened immune systems and total several thousand cases annually in the U.S. The more significant threat lies in the overall rising trend of drug-resistant fungal cases.
“The pathogens causing these infections are becoming increasingly resistant,” he stated. “While it isn’t comparable to waking up to a fungal pandemic like Covid, this issue is worse now than it was five, ten, or twenty years ago.”