The U.S. is grappling with a hefty public health and economic issue: obesity. Over 40% of American adults are classified as obese, which imposes a significant strain on the healthcare system—estimates suggest costs of around $173 billion each year. And honestly, that figure might just scratch the surface. Beyond direct medical expenses, obesity impacts workforce participation, burdens public resources, and hinders economic growth.
As Congress addresses this pressing matter, there’s a clear need for improved tools that can adequately measure the extensive economic and social ramifications of obesity. To their credit, the Congressional Budget Office (CBO) should refine its methodology for evaluating the long-term impact of obesity treatments as discussions about expanding Medicare coverage for weight-loss medications progress.
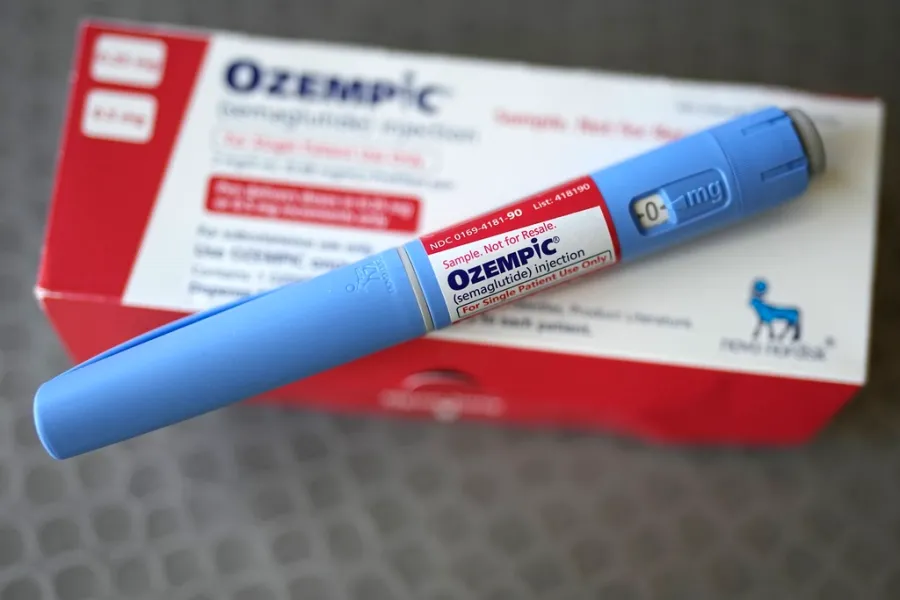
A new class of treatments, known as GLP-1 receptor agonists, seems to hold promise for mitigating the obesity crisis and its associated challenges. Initially aimed at managing diabetes, drugs like semaglutide (Wegovy, Ozempic) and tirzepatide (Mounjaro, Zepbound) have displayed remarkable effectiveness in promoting weight loss and alleviating related conditions like type 2 diabetes and heart disease.
Clinical findings are beginning to make waves in medical practice. The American College of Cardiology, for instance, recently highlighted GLP-1s as a first-line approach for treating obesity in individuals at risk for heart conditions. Studies have illustrated that these medications can outperform lifestyle changes and are generally safer than surgical options. During trials, an average weight loss of about 15% was observed—results traditionally only attained through bariatric surgery. This shift could signify a pivotal moment in obesity treatment.
Up until now, the CBO has depended on static scoring to evaluate weight-loss drug coverage. This method looks at the immediate fiscal impact of a policy over a decade, without factoring in broader economic dynamics, like enhanced participation in the workforce, fewer disability claims, or increased tax income.
The reason for sticking with static scoring seems to stem from a caution against extrapolating uncertain economic feedback effects; the focus has been on direct budget outcomes. However, this means missing the longer-term implications of innovations like GLP-1s.
It’s vital to recognize that obesity isn’t merely a health concern—it also dampens economic performance. Making effective treatments more accessible might cut health expenditures and boost productivity, benefiting various sectors.
A relevant example is the food and beverage industry. Some evidence suggests that the use of GLP-1s could lead consumer preferences to shift away from highly processed foods like snacks and sweets. Though this might disrupt certain markets, it could also pave the way for innovations in healthier food options and their supply chains.
The labor market stands to gain from a decline in obesity rates as well. Conditions tied to obesity negatively affect workforce engagement, increase disability claims, and lower productivity levels. Absenteeism and what’s termed “presenteeism” (when individuals aren’t fully engaged at work) are ongoing, costly challenges for employers. In 2023 alone, the financial toll of obesity-related absenteeism on U.S. businesses reached approximately $82.3 billion, with an additional $160.3 billion attributed to presenteeism. Enhancing health outcomes on a large scale could bolster the workforce and potentially augment tax revenues, but such macroeconomic consequences are overlooked in the CBO’s current scoring models, showcasing a need for more comprehensive tools that assess the far-reaching effects of obesity.
To accurately gauge the economic implications of specific treatments, dynamic scoring could be beneficial. Unlike static scoring, this approach considers macroeconomic feedback effects and observes how policies evolve over time, impacting behaviors and production among other key indicators. The CBO has had instances of dynamic scoring in major laws.
For example, after the 2017 Tax Cuts and Jobs Act adjusted corporate and personal tax rates for growth stimulation, models were developed to predict how tax policy shifts would influence GDP, employment, and federal revenue. Presently, dynamic scoring is mandated for legislation expected to have a fiscal impact of 0.25% of GDP (roughly $75 billion) or more.
However, the economic threshold shouldn’t solely dictate whether such a model is applied. Consider policies like GLP-1 coverage: they might not meet this financial threshold yet could yield substantial broader impacts. For instance, while a proposal to expand Medicare coverage for GLP-1s might appear costly under static scoring, dynamic scoring could provide a more holistic view of future healthcare savings, productivity enhancements, and cross-sector economic gains.
It’s essential to acknowledge the uncertainties and assumptions inherent in dynamic scoring, as with all budget predictions. However, the greater risk lies in overlooking wide-ranging economic consequences, which could lead to underfunding of treatments that could bring about considerable social and economic improvements.
To clarify, GLP-1 isn’t a catch-all solution. Accessibility, careful clinical management, and integration with lifestyle support remain crucial. Nonetheless, when strategically utilized, these treatments present a promising opportunity to tackle chronic illnesses while also fortifying economic resilience.
This discussion goes beyond weight loss; it’s about unleashing economic potential by lowering long-term healthcare expenses, strengthening the workforce, and alleviating stress on essential public systems. The federal budget process must mirror this reality. If the U.S. is serious about combating obesity, it needs to evolve its approach to scoring related policies.