New Insights on Thymic Health and Its Impact on Adult Mortality
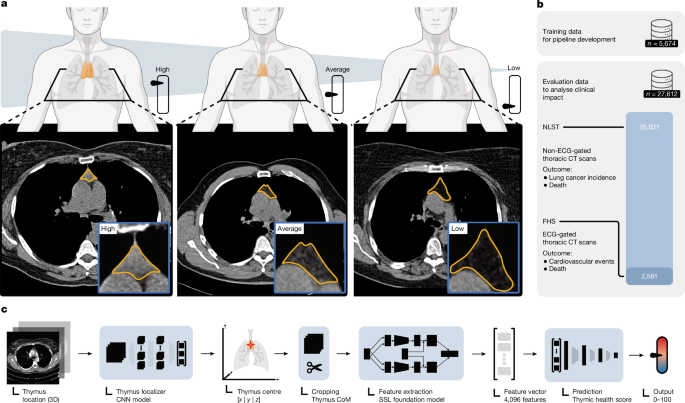
Recent research reveals that thymic decay in adults varies greatly from person to person, and that weakened thymic health correlates with increased mortality and higher rates of diseases, including cancer and cardiovascular issues. This study used data from two independent clinical trials involving asymptomatic adults: the NLST and the FHS. In the NLST, which had over 25,000 participants, those with better thymic health had a significantly lower risk of death from various causes, lung cancer, and heart disease, regardless of factors like sex, age, smoking status, or past health issues. The FHS showed similar results, confirming a lower risk of cardiovascular-related deaths among participants with good thymic health, reinforcing the importance of the immune system in maintaining long-term health.
The data suggests that individuals deemed healthy in the NLST, with optimal thymic health, had about a 50% lower risk of dying, were 36% less likely to develop lung cancer, and nearly 50% less likely to die from it compared to those with poor thymic health. Furthermore, the impacts of enhanced thymic health on cardiovascular diseases were consistent across both cohorts, with reductions in mortality risk from heart disease ranging from 63% to 92%. The findings underscore the thymus’s essential function in producing diverse T cells, which is vital for a robust immune system and increased longevity.
This study challenges the common belief that the decline of thymic output in older adults is unimportant, as it had previously been thought that peripheral T cell expansion could offset this loss. Instead, the research indicates that loss of thymic tissue may predict greater risks of illness and mortality. While the importance of T cell diversity is well-established in youth, these findings imply that the thymus continues to play a notable role in adult T cell production. A decline in thymic function is linked to poorer health outcomes.
Additional studies have pointed towards a connection between thymectomy, or thymus removal, and a reduced lifespan alongside a higher cancer risk. Though thymectomy is uncommon, the findings of this research suggest that thymic health can also decline significantly in individuals who have not undergone surgery, which has broader implications given the age-related decline in immune function. This aligns with existing literature that has modeled decreasing T cell output as a major risk factor for increased cancer rates with aging.
Lifestyle and metabolic indicators, such as smoking habits, physical activity levels, and lipoprotein levels, showed notable links to thymic health. Chronic inflammation—often tied to stress, unhealthy diets, and obesity—was correlated with lower thymic health in longitudinal blood evaluations of participants.
Among seemingly healthy people in the FHS, poor thymic health was linked to inflammatory modifications in blood plasma. A pro-inflammatory profile was characterized by increased levels of cytokines like IL-6 and IL-18, which are relevant in systemic inflammatory diseases and age-related conditions. This supports previous findings that thymic involution is connected to inflammation and related illnesses.
Moreover, the increase in early-onset cancers may be linked to accelerated thymic decay, which might be exacerbated by unhealthy lifestyle factors, contributing to greater inflammation. Understanding thymic health could improve disease and cancer screening methods, particularly for those at higher risk.
This research specifically examined the relationship between thymic health and lung cancer rates in smokers and former smokers. Interestingly, results were largely driven by current smokers, presumably due to stronger statistical evidence stemming from higher occurrence rates and the heightened biological significance of thymic function in the presence of ongoing tobacco exposure.
Previous investigations into thymic characteristics through imaging have been limited, not providing strong correlations to outcomes like survival or disease incidence. Studies suggested a complete fatty degeneration of the thymus in a large percentage of subjects—ranging from 60% to 75%—which contradicts biological expectations of sustained T cell output in those instances. However, this study employed deep learning models to assess thymic health, offering insights into the health benefits tied to optimal thymic function among a significant portion of participants.
Although this study highlighted strong associations between thymic health and morbidity across genders and ages, further investigation in diverse populations is necessary. While a link between thymic health and overall survival was found, it didn’t retain significance after comprehensive adjustments in the smaller FHS group. This suggests that lifestyle choices may significantly influence long-term health outcomes in this population.
The study emphasizes the complex relationship between thymic health and various health outcomes, indicating its crucial role in adult well-being. Moving forward, understanding how to improve thymic health could inform healthcare strategies aimed at reducing thymic decay. Even practical lifestyle changes around exercise, diet, and sleep are likely to have considerable effects on thymic health.
This research reveals potential negative implications of diminished thymic health. Aging leads to a decline in thymic function, yet significant variation exists, pointing to a wide range of decay rates among individuals. The analysis linking chronic inflammation to thymic decay supports the idea that there might be genetic factors at play, affecting rates of thymic health decline.
However, a retrospective observational design means we cannot definitively draw causal connections. It’s possible that poorer thymic health leads to increased risk factors, or that existing health issues lead to reduced thymic condition. Future studies are necessary to clarify these associations and assess whether thymic health can be a target for preventive care or treatment approaches.
In summary, this research stresses the highly personalized nature of thymic health and its previously overlooked importance in maintaining a responsive immune system for long-term well-being and longevity. The findings underscore the need for routine assessments of thymic health in clinical practice, as current methodologies lack established standards. By examining a large participant pool, it’s clear that improving thymic health could be actionable through lifestyle modifications, such as reducing smoking and achieving a healthier weight for those who are overweight or obese.