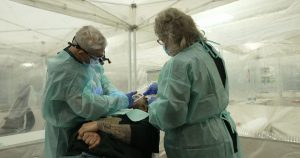
When Michael Adams was researching health insurance options Last year, he had one very specific requirement. That is compensation for prosthetic limbs.
Adams, 51, lost his right leg to cancer 40 years ago and has worn it out countless times. he chose the gold plan Colorado Health Insurance Marketplace It covered a prosthetic leg, including a microprocessor-controlled knee like the one he had used for years. This feature increases stability and helps prevent falls.
But when his foot, which he had been using daily for about five years, needed replacement in January, his new market health plan didn't allow for it. The nearly $50,000 leg with an electronically controlled knee was not medically necessary, the insurance company said. colorado state law That decision rests with the patient's doctor, who has been prescribing versions of that leg for years, even when the patient was covered by employer insurance.
“Electronic knee prostheses are life-changing,” said Adams, who lives in Lafayette, Colorado, with his wife and two children. Without it, “it's like going back to the wooden legs like when you were a kid.” The knee's microprocessor reacts to different surfaces and inclines, stiffening when it detects movement that indicates the user is about to fall.
Alana Adams
People who need surgery to replace a joint usually don't encounter similar coverage obstacles. According to the federal Agency for Healthcare Research and Quality (AHRQ), 1.5 million knee or hip replacement surgeries were performed at U.S. hospitals and hospital-owned outpatient facilities in 2021. of median price One analysis found that an uncomplicated total hip or knee replacement at a top orthopedic hospital cost just over $68,000 in 2020, but health insurance offers the ability to negotiate lower rates. It is often done.
For those in the amputee community, disparities in coverage amount to discrimination.
“Knee replacements are covered by insurance if they're covered by skin, but not if they're covered by plastic,” says a family doctor and the Amputee Coalition, an advocacy group. said Jeffrey Cain, former chairman of the board. Kane lost his prosthetic leg in a plane crash nearly 30 years ago and now has two prosthetic legs.
Health insurance typically provides coverage when a prosthesis is deemed medically necessary, such as to replace a part of the body or function in walking or daily activities, according to AHIP, a health insurance industry group. But in reality, coverage of prosthetics by private health insurance varies widely, said Ashley White, chief strategy and program officer at the Amputee Coalition. Even when a plan includes basic prosthesis coverage, “insurance companies often put device caps and restrictions on the types of devices that are approved,” White said.
In other words, patient costs It can also vary widely based on a person's coverage details, plan limits, and even geographic cost differences.
Ann Estimated 2.3 million people According to an analysis by healthcare consulting firm Abarere, some people in the United States are living with limb loss. The numbers are expected to be About twice as much In the coming years, people will age and more people will lose limbs to diabetes, trauma, and other medical problems.
According to one study, fewer than half of people with limb loss are prescribed a prosthesis. Report by AHRQ. Despite microprocessor-controlled knees like Adams's having been in use for decades, the plan refuses to apply for prosthetic legs, arguing that they are not medically necessary or are experimental devices. There is a possibility that
Cain was instrumental in passing a 2000 Colorado law that required insurance companies to cover prosthetic arms and legs on par with Medicare, requiring coverage with a 20% coinsurance. Since the bill was enacted, about half of states have adopted insurance equity laws that require plans to cover prosthetic limbs on par with other covered medical services or to require coverage of prosthetic limbs that enable sports. passed the law. However, these laws Applies to plans only Regulated by state. More than half of people with private insurance have plans that are not covered by state law.
The Medicare program's 80% coverage of prosthetics mirrors coverage of other services. nevertheless, Government Accountability Office It was found that only 30% of recipients who lost a limb in 2016 received a prosthetic leg over the next three years.
Cost is an important factor for many people.
“Regardless of your insurance, most people will have to pay something for the device,” White said. As a result, “many people end up using payment plans for their devices,” she says. Some people may take out a loan.
The Federal Consumer Financial Protection Bureau has proposed the following rules: Prohibit lenders from foreclosure If you are unable to repay your loan, you will be provided with medical equipment such as a wheelchair or prosthetic limbs.
“This is a replacement limb,” White said. He said his organization has heard of several cases where lenders have seized wheelchairs and prosthetic legs. Foreclosure is “literally a punishment for the individual.”
Mr. Adams ultimately owed approximately $4,000 in coinsurance for the new leg, which covered his portion of the fee negotiated by the insurance company for the knee and foot portions of the leg. It did not include an expensive piece that fits around the residual limb, and there was no need for it. Exchange. Adams said the insurance company approved the prosthesis on appeal, citing a clerical error.
“I'm lucky to be able to afford that 20%,” said Adams, a self-employed leadership consultant.
Again, even if the patient has health insurance and a doctor's prescription, the plan's coinsurance requirements, coverage caps, and other limitations can make out-of-pocket costs prohibitive. Possibly.
Leah Kaplan has no financial flexibility. She was born without a left hand and didn't have a prosthetic leg until a few years ago.
“I didn't want people to stare at me anymore,” Kaplan, 32, said of her decision not to use a prosthetic leg as an adult. A few years ago, the cycling enthusiast got a prosthetic arm specifically designed for use on her bike. The device was covered by her medical insurance through her job with county government in Spokane, Washington, which helps people with developmental disabilities transition from school to work.
However, when he tried to get approval for a prosthetic hand to use in his daily life, he was refused due to health insurance regulations. of Myoelectric hand that she requested It moves its hands in response to electrical impulses in its arms to perform specific actions. Without insurance coverage, it would cost her more than $46,000, which she said she couldn't afford.
She worked with her doctor to appeal this decision to her insurance company, but was denied three times. Kaplan said it's still unclear exactly what the rationale is, other than the insurance company questioning the medical necessity of the prosthetic hand. The next step is to appeal to an independent review agency certified by the state insurance commissioner's office.
Kaplan said a prosthetic arm is not a luxury tool. The prosthetics clinic ordered the hand and created a customized socket that fit the end of her arm. But she can't use it until insurance coverage is sorted out.
At this point, she feels defeated. “I've been waiting for this for a long time,” Kaplan said.
KFF Health News is a national newsroom that produces in-depth journalism on health issues and is one of our core operating programs. KFF — An independent source for health policy research, polling, and journalism.