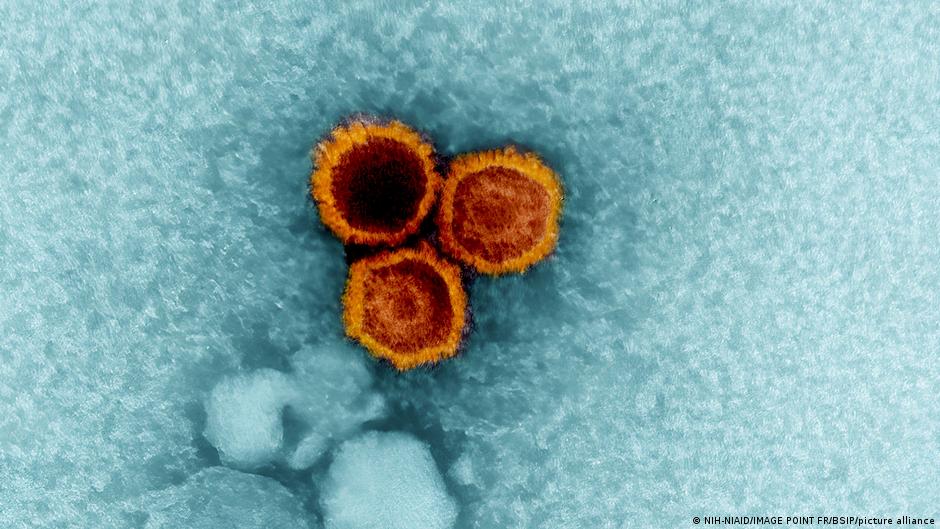
The Epstein-Barr virus, a type of herpes virus, is linked to various cancers and autoimmune diseases. It spreads through droplets, like saliva, which is why one of its related conditions, Pfeiffer’s disease—also called the “kissing disease”—is often associated with kissing.
For quite some time, there’s been awareness that Epstein-Barr virus (EBV) may contribute to multiple sclerosis (MS). Yet, here’s the tricky part: nearly everyone carries EBV, but only a small fraction, less than 1%, actually develops MS. So, what’s going on?
Scientists might be inching closer to understanding this puzzle, with hints nestled in our genes.
MS: A Misguided Immune Response
Individuals with multiple sclerosis experience a confusion within their immune system. Instead of defending against outside threats, it mistakenly turns on its own body. Parts of the immune defense begin to attack the myelin sheath—the protective layer around nerve fibers that helps in communication between nerves.
This can lead to a range of troubling symptoms, such as vision problems and difficulties controlling abdominal and bladder functions. Over time, even the muscles responsible for breathing can be impacted.
Current treatments for MS often focus on suppressing the immune system, but ideally, preventing the disease from manifesting would be much better.
EBV and the Heightened Risk of MS
Researchers from several countries, including China, Germany, Switzerland, and the UK, have revealed how the presence of the Epstein-Barr virus, combined with specific genetic traits, raises the likelihood of developing MS.
A key player seems to be a molecule called HLA-DR15, which is part of the immune system. It acts like a signal, indicating to the immune response what’s happening within cells.
When B cells—white blood cells that produce antibodies—get infected with EBV, they show parts of the virus to other immune cells. This is meant to prepare the immune system against the virus, but there’s a catch: these viral components closely resemble certain proteins found in the myelin sheath. So, the immune system ends up misdirected, attacking myelin instead.
A Disturbingly Similar Situation
The connection between EBV and MS isn’t new, but recent findings suggest a more elaborate scheme. When B cells express the HLA-DR15 molecule, EBV manipulates them to present myelin proteins. This means the body of an MS patient isn’t just mistakenly attacking itself; it’s being actively tricked into doing so.
Still, HLA-DR15 alone doesn’t encompass the entire picture. Only about half of those with MS carry this genetic variant. Meanwhile, many in northern Europe have this marker, yet very few actually develop MS. It suggests that while this gene increases risk, it’s not the sole factor responsible.
Timing is Everything: The Vulnerable Years
When a person encounters an EBV infection appears to be crucial in MS development, especially during late childhood and young adulthood. Factors like poor diet, low vitamin D levels, smoking, pollution, shift work, and obesity might worsen the situation.
Why is an EBV Vaccine Elusive?
Experts believe that developing a vaccine to prevent initial EBV infections may be unlikely because the virus is highly adapted to humans. However, crafting a vaccine to prevent Pfeiffer’s disease after someone has been infected seems feasible, according to researchers. A preventative vaccine administered early in life could significantly reduce the risk of MS later on.
Vaccines Against Epstein-Barr: What’s on the Horizon?
Some initial candidates for vaccines are currently being tested. There’s renewed interest in this area, especially after years of stagnation. Researchers hope to apply recently uncovered mechanisms to develop potential treatments, specifically targeting immune cells that react to EBV. It’s still uncertain if these methods will be effective, but there’s optimism about the tools now available.
These treatments would be applied to MS patients with the HLA-DR15 genetic profile, which, if successful, could represent a significant step forward in combating MS.