Scientists have long been plaguing the brain for ways to treat Alzheimer's disease, the most common type of dementia.
We see that the answer may lie within our own brains. Proposals from Northwestern University Enhancing the immune cells of the brain may better equip them to clean up harmful masses of the toxic protein amyloid beta, a characteristic of Alzheimer's disease.
“Our research is very novel, because we had a rare opportunity to analyze one of the largest postmortem brain cohorts of Alzheimer's patients treated with Alzheimer's disease, as well as those approved by the FDA for Alzheimer's disease.”
Researchers looked at 13 brains vaccinated with six Alzheimer's brains that were not treated and six disease-free brains.
Amyloid beta is a small protein fragment that forms plaque-like deposits when abnormally accumulated in the brain. Vaccination is supposed to trigger the immune system to produce antibodies to remove plaque.
However, clinical trials for amyloid beta vaccines against Alzheimer's disease have repeatedly failed. Dangerous brain swelling is a major side effect.
The challenge for vaccine developers is to create an immune response that can fight amyloid beta without attacking healthy cells.
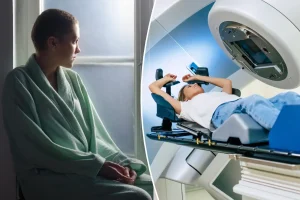
The US Food and Drug Administration has approved several antibody treatments to target amyloid beta in Alzheimer's disease. They are given as intravenous infusions.
“These drugs stimulate immune cells in the brain to remove amyloid beta, but we believe that data from our publications can be used to make these drugs even better,” the corresponding study author said. David GateNorthwest Assistant Professor of Neurology.
The Northwestern team discovered that when these types of treatments work, brain immune cells (known as microglia) can help clear the plaque and restore a healthier brain environment.
Of the 13 vaccinated brains, there were seven levels of plaque clearance. The other six people had limited clearance.
“Our study first identified the mechanisms of microglia, a brain immune cell that helps limit the spread of amyloid in certain brain regions after treatment with amyloid-targeted drugs,” he said. Abrams Research Center on Neurogenomics.
The Gate team found that only some microglia are effective in removing plaque. Factors of success include brain regions, type of vaccination, and genetic activity.
The good news is that microglia are not always focused on amyloid removal.
“They remove the amyloid and then they go back to good condition and actually seem to help their brain heal,” Gate said.
The bad news is that targeting Microglia directly remains a challenge.
“If we can define mechanisms related to pathological clearance and find the genetic makeup of immune cells associated with people who are really responsive to drugs, we can probably one day get around the entire drug process and target these specific cells,” says Gate.
Gate's conclusions were published on Thursday Natural Medicine.
He told the Post that the team is investigating the effectiveness of brain tissue in patients receiving new anti-amyloid antibodies, and is investigating how these findings can be applied to other neurodegenerative diseases such as Parkinson's disease and ALS.
Alzheimer's Disease affects an estimated 7 million Americans Approximately 1 million Americans I am suffering from Parkinson's disease. Less than 30,000 Americans are believed to have ALS.