Immunologist Jacob Glanville stumbled upon some intriguing media stories in 2017 about a man who had injected himself repeatedly with the venom of some of the world’s most dangerous snakes—think cobras, mambas, and rattlesnakes—and even allowed himself to be bitten.
“The articles were a bit sensational. ‘Crazy guy gets bitten by snakes,’” Glanville recalled. “But when I looked deeper, I felt like there was something valuable here.”
That valuable insight was Tim Friede, a self-taught snake enthusiast from California, who spent almost 18 years exposing himself to snake venom, effectively building up immunity to various neurotoxins.
“We had this conversation, and I mentioned, I know it’s a bit odd, but I’d really like to look at your blood,” Glanville remembered. To his surprise, Friede responded, “Finally, I’ve been waiting for this call.”
They decided to collaborate, and Friede provided a 40-milliliter blood sample. Fast forward eight years, and Glanville and Peter Kwong, a professor at Columbia University’s Vagelos College of Physicians and Surgeons, have announced details of an antivenom that shows promise against bites from 19 species of venomous snakes—at least in mice—based on the antibodies in Friede’s blood combined with a venom-blocking drug.
“Tim has an incredible history. He used a variety of species from every continent with snakes, and he meticulously kept records throughout his nearly 18-year journey,” Glanville noted.
But, he was quick to add, “We strongly advise against anyone attempting what Tim did. Snake venom is incredibly dangerous.”
Friede stopped his venom immunization in 2018 after experiencing some close calls and now works for Glanville’s company, Centivax. Glanville is the CEO and chairman there.
Their research was published recently in the journal Cell, and while CNN reached out to Friede for an interview, he hasn’t responded.
If, heaven forbid, you find yourself bitten by a venomous snake, antivenom is your best bet, but the traditional methods of making it have not changed much since the Victorian era.
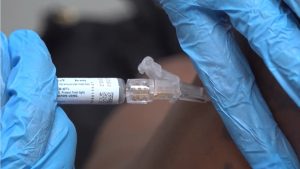
Typically, the process involves milking snake venom and injecting small doses into animals like horses to create an immune response. Their blood is then drawn and purified to get the required antibodies.
This method can be messy and quite risky, prone to errors, and sometimes the resulting serum leads to serious side effects.
Experts have been urging for improved snakebite treatments, as these incidents unfortunately claim around 200 lives each day, especially in less developed countries, with nearly 400,000 people left with disabilities each year. The WHO even categorized snakebite as a neglected tropical disease back in 2017.
Glanville, who grew up in rural Guatemala, was acutely aware of the health risks posed by snakebites and quickly realized that Friede’s unique experience could lead to something significant.
By subjecting himself to snake venoms for nearly two decades through injections and bites, Friede had developed antibodies that were effective against multiple snake neurotoxins.
Researchers isolated antibodies from Friede’s blood that reacted to neurotoxins from the 19 snake species studied, including various corals, mambas, and cobras.
These antibodies were tested one by one on mice injected with venom from each species, helping scientists determine the minimum components needed to neutralize all the different venoms.
The resulting drug combination included two antibodies from Friede’s blood and a small-molecule drug called varespladib, which inhibits an enzyme found in about 95% of snakebites. This drug is currently undergoing human clinical trials as a standalone treatment.
The first antibody, LNX-D09, was effective in protecting mice from a lethal dose of venom from six snake species.
Adding varespladib helped shield against three more species, and then a second antibody, SNX-B03, extended protection to include all 19 species tested.
The researchers found that the antivenom offered complete protection for 13 species and partial protection for the remaining six in mice.
Steven Hall, a snakebite pharmacologist at Lancaster University, called the approach a “very clever and creative way” to develop antivenom. However, he was not part of the research team.
Although the cocktail hasn’t been tested on humans yet, Hall speculated that if it receives clinical approval, the human-derived antibodies might result in fewer side effects compared to traditional methods, which often cause allergic reactions.
“It’s impressive because it uses just one or two antibodies along with a small-molecule drug, increasing the number of species it covers compared to typical antivenoms. It really emphasizes the potential of combining a small molecule with antibodies,” he added.
“If this eventually makes it into clinics and into people, it could be revolutionary and transform snakebite treatment altogether,” he concluded.
Kwong from Columbia mentioned that the research focused on elapids but didn’t include the other major group, viperids, which encompasses rattlesnakes and saw-scaled vipers.
Still, the team is looking into whether other antibodies from Friede’s blood or different agents might cover this viper family.
“The goal is to create a single antivenom cocktail or possibly two—one for elapids and one for viperids—since some regions only have one type,” Kwong remarked.
They also plan to start field research in Australia, which features only elapid snakes, allowing veterinarians to use the antivenom on dogs bitten by snakes.