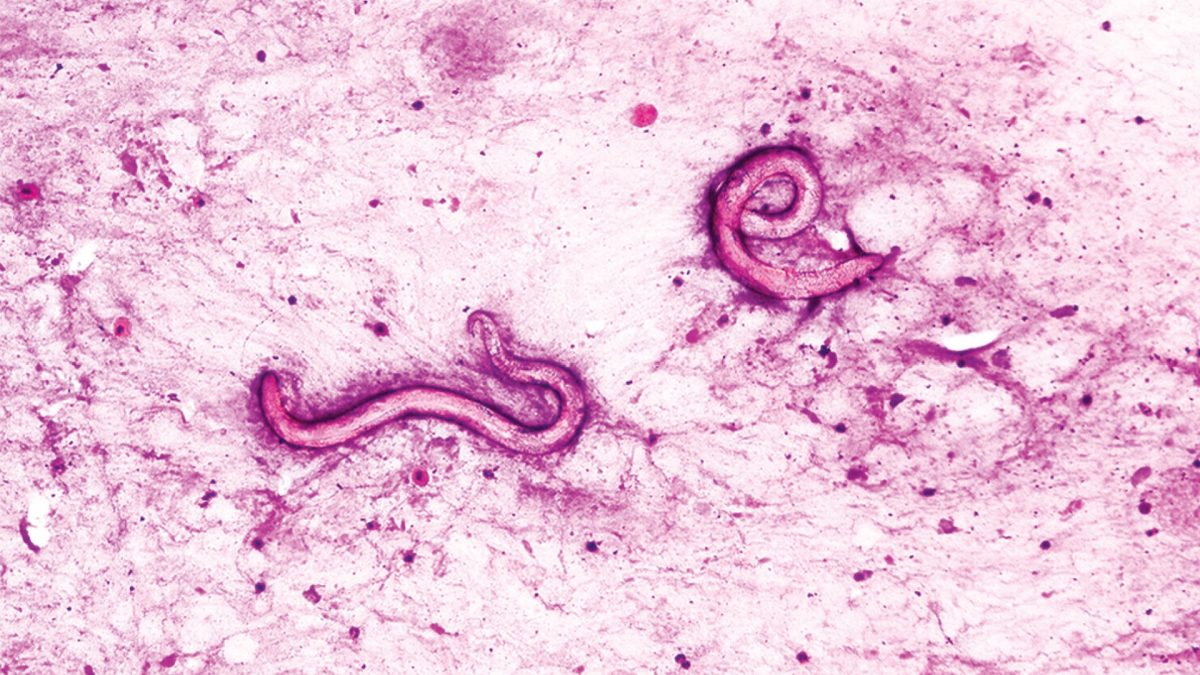
Transplant Recipients Infected with Parasitic Worms
Two men ended up with parasitic worms after receiving infected kidney transplants at U.S. hospitals, as reported in a recent case study. Both kidneys were from the same donor, who had lived in the Caribbean prior to passing away, according to the June 18 report published in the New England Journal of Medicine.
The first recipient, a 61-year-old man, underwent surgery at Massachusetts General Hospital (MassGen). About ten weeks later, he was readmitted to MassGen after an initial stay at another facility. He had been experiencing nausea, vomiting, intense thirst, abdominal discomfort, back pain, and a fever. At the first hospital, medical staff discovered fluid accumulating in his lungs, and he started breathing rapidly, feeling as if he couldn’t get enough air. His oxygen levels fell significantly.
As he deteriorated into respiratory failure and shock—characterized by dangerously low blood pressure—he was transferred to MassGen’s intensive care unit, where doctors noticed a purple rash, resembling bruises, on his abdomen.
The medical team initiated a thorough investigation into his condition, conducting extensive tests to identify the source of his symptoms. The patient was on immunosuppressive drugs to prevent kidney rejection, making him vulnerable to infections. Dr. Camille Kotton, a specialist in infectious diseases and organ transplantation, faced the challenge of narrowing down a long list of potential infections to find what was really going on.
Bacterial infections were ruled out since the patient had received antibiotics without any improvement, and he was also on an antiviral while testing negative for COVID-19. This left the possibility of a parasitic infection, further supported by a spike in eosinophils—white blood cells associated with fighting off parasites. Although spikes can also occur due to drug reactions or transplant rejections, those explanations seemed less likely given the man’s symptoms.
Dr. Kotton remembered cases where kidney transplants had led to infections with a small roundworm known as Strongyloides stercoralis. She contacted the regional organ-procurement organization about possible contamination. Despite the donor’s death, they managed to test a sample of the donor’s blood, which showed antibodies to Strongyloides, indicating prior exposure to the worm.
Blood tests of the patient revealed he lacked these antibodies before the transplant, but they were present afterward. Further examinations showed the worms had spread throughout his abdomen, lungs, and skin.
Infections from organ transplants are quite unusual; a review over more than a decade noted only 14 out of every 10,000 transplants resulted in donor-derived infections. Although U.S. doctors can’t use organs from donors with active infections like tuberculosis, testing for infectious diseases doesn’t always catch everything.
That review noted 13 confirmed or probable Strongyloides infections over ten years, accounting for 42% of all parasitic infections from organ transplants. Before the review, less than a quarter of organ transplant organizations regularly screened for Strongyloides, but in 2023, the Organ Procurement and Transplantation Network recommended universal testing for this parasite.
The medical team at MassGen treated the man with ivermectin, a potent antiparasitic medication. They received special permission to administer it directly under his skin to treat the widespread infection, ultimately leading to his recovery.
Meanwhile, other facilities that had transplanted organs from the same donor were alerted. This also included a 66-year-old man at Albany Medical Center who exhibited fatigue, low white blood cells, and declining kidney function post-transplant.
Coordinating with the MassGen team, medical staff at Albany successfully treated the second patient who had received the other kidney from the donor. A spokesperson for Albany Medical Center emphasized the importance of communication and collaboration in managing such rare cases where transplant infections occur.