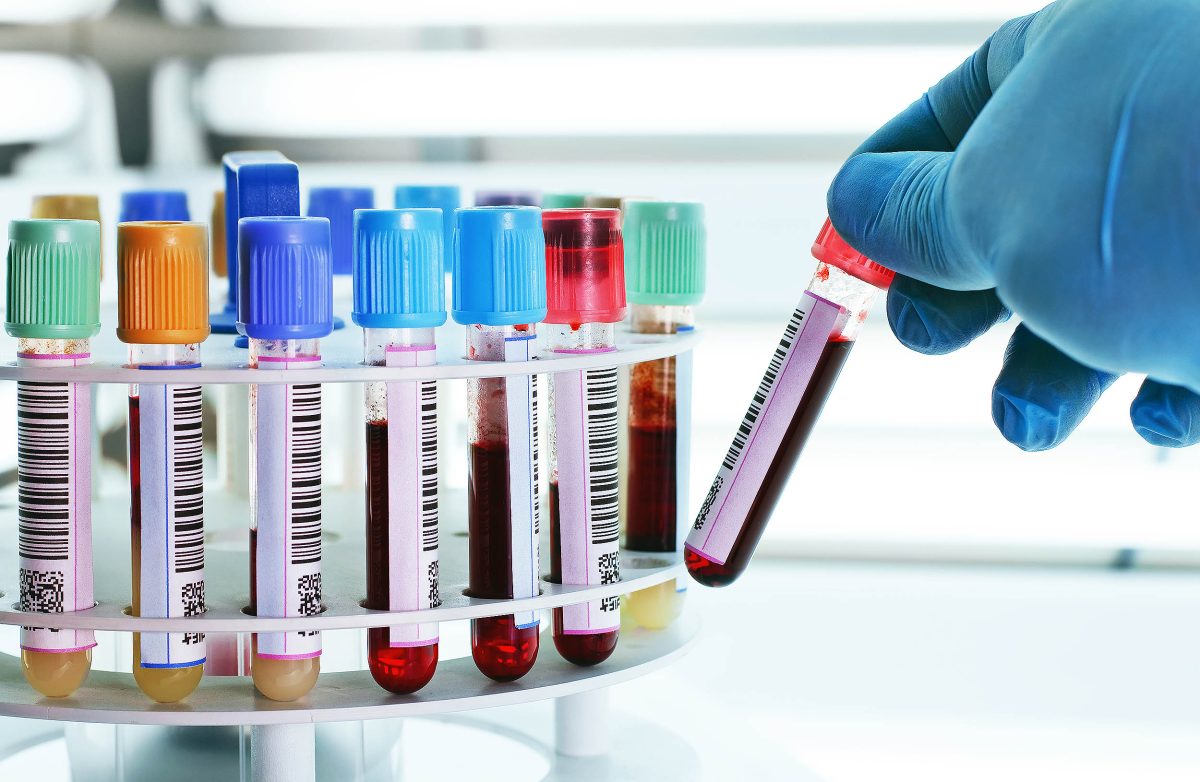
Memory issues can be quite unsettling, and finding clear answers often takes time. Traditionally, assessing patients for Alzheimer’s involved either PET scans or spinal taps, with no blood tests included.
While these methods can be effective, they also tend to be costly, invasive, or hard to access. This can leave many individuals waiting anxiously, shuttling between various appointments.
A new blood test is aiming to change the initial step in Alzheimer’s care. This test looks for the same biological markers associated with Alzheimer’s and translates them into a single score, indicating the likelihood of Alzheimer’s biology being present.
This development could provide doctors with a quicker, more straightforward way to determine the next steps in patient care.
Significance of the Alzheimer’s Blood Test
Many individuals with early memory concerns begin their journey in primary care settings, which are typically busy and lack advanced imaging technologies.
A reliable blood test could help in identifying patients sooner. Some might be directed to specialists right away.
Others might be monitored as doctors examine for sleep issues, depression, thyroid concerns, medication side effects, or other common cognitive symptoms.
This kind of early sorting not only saves time and reduces costs but also minimizes unnecessary procedures. It enables families to shift from uncertainty to action plans—much quicker than before.
How the Test Works
Alzheimer’s is characterized by two primary components in the brain: abnormal amyloid and tau proteins. The new blood test investigates a specific form of tau known as p-tau217 and assesses the ratio of two amyloid fragments: Aβ42 to Aβ40.
These combined metrics capture critical biological aspects that concern doctors. The outcome is a probability score that signifies how closely a person’s blood pattern aligns with Alzheimer’s changes.
Utilizing both markers enhances accuracy—p-tau217 indicates Alzheimer’s-related changes, while the amyloid ratio helps reduce false positives. Together, they clarify whether Alzheimer’s biology is likely present.
Real-World Testing
To evaluate the test’s effectiveness in real-world settings—not just controlled environments—researchers enrolled over a thousand participants in Sweden who had memory or cognitive concerns.
Subjects were assessed both in primary care and specialized memory clinics, receiving the usual clinical evaluations.
Blood samples were processed similarly to how they would be in a hospital lab, handled in batches and on a schedule. This approach is crucial for testing reliability under normal operating conditions.
Comparing Methods
Simply put, the blood test aligned with definitive measures of Alzheimer’s biology about 90% of the time. Its effectiveness remained consistent in both primary care and specialist clinics, which is where it needs to be reliable.
“In primary care, the accuracy of identifying Alzheimer’s disease was 61%, while specialists had a 73% accuracy rate,” noted a neurologist from Lund University.
This highlights the significant need for effective, cost-efficient diagnostic tools, especially in primary care, and suggests that this blood test could greatly enhance diagnosis in healthcare settings.
Fixed Testing Thresholds
The research team predetermined the thresholds for the Alzheimer’s blood test and kept them consistent. This simulates how a diagnostic would be used in a real-world scenario.
There was no adjustment after reviewing results, and no unique cutoffs for clinics. Maintaining a fixed threshold boosts the likelihood that the test will produce similar results across various locations.
This method boosts confidence among doctors who need reliable tools. Consistency between different settings distinguishes a research study from a diagnostic that can be widely implemented.
When standard evaluations were used by themselves, clinicians performed adequately. However, incorporating blood test results improved decision-making precision.
A negative outcome for someone with mild memory concerns gives doctors the assurance to avoid invasive tests and monitor changes over time.
If symptoms escalate, a positive result supports the need for additional testing and, where suitable, therapies targeting Alzheimer’s biology.
It’s important to note that this blood test neither replaces PET scans nor spinal fluid analysis; it merely refines the application of these tests.
Public Understanding
This test is not intended for casual screening among asymptomatic individuals. It serves as a first-line tool when there are genuine memory concerns that require further examination.
When used correctly, it can expedite the process of finding answers for those needing more comprehensive evaluations while shielding others from unnecessary procedures.
It seamlessly fits into regular workflows: routine blood draws, timely lab processing, and a concise, interpretable score. That’s the kind of practicality busy clinics require to operate effectively.
“This test is already available in the USA and is expected to roll out in other countries soon,” stated a senior researcher at Lund University.
“Initially, it will mainly be utilized in specialized memory clinics, and it may take about one to two years before implementation in primary care is fully established.”
As availability expands, specialist clinics are expected to lead the way, with primary care following as training and protocols develop. This phased rollout is typical when new diagnostics become incorporated into everyday healthcare.
The Future of Alzheimer’s Blood Tests
In summary, this new blood test provides primary care physicians with a rapid, evidence-based indicator of Alzheimer’s, boasting a 90% accuracy rate for guiding subsequent steps.
While it won’t cure the disease, it offers clearer guidance earlier in the process for those who need it most.
For families, this could mean fewer obstacles and faster, appropriate referrals. For clinicians, it’s a practical tool that enhances decision-making.
For healthcare systems, it allows for advanced testing to be directed where it can have the greatest impact. This progress is not just measured in lab results but also in real-world experience—faster, more serene, and more straightforward.
The full study appears in the Journal of the American Medical Association.