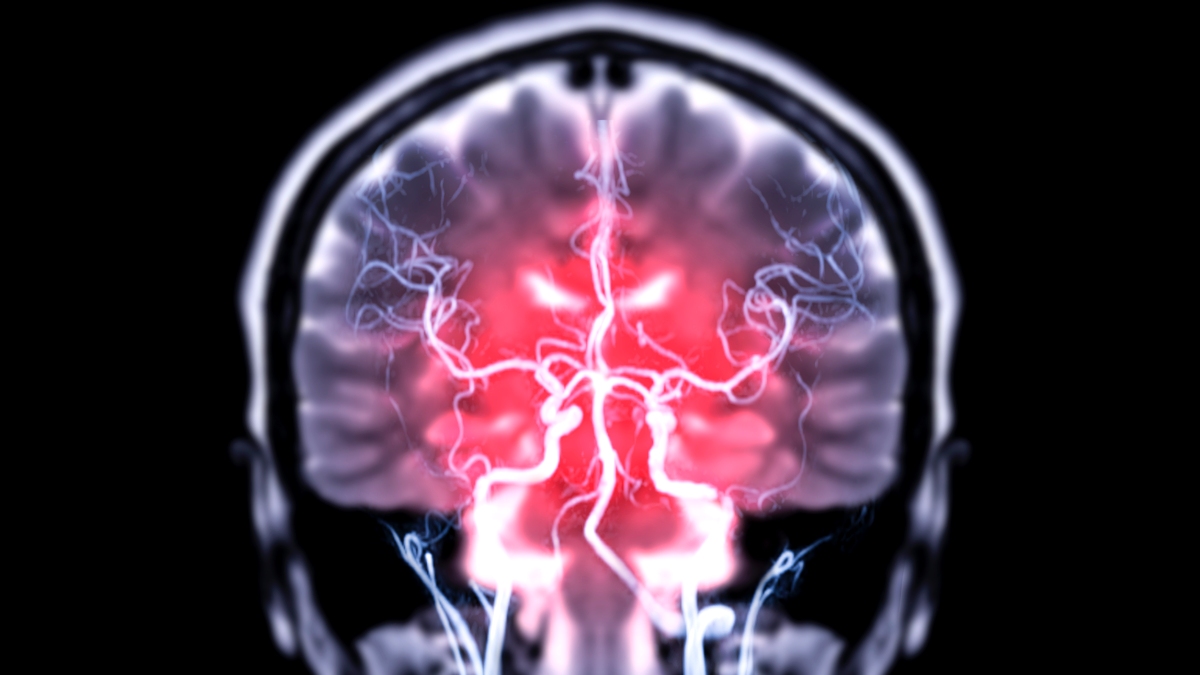
New Research on Gut-Bacteria Connection to the Brain
Previous studies have shown a noteworthy relationship between gut activity and brain function, and vice versa. New research conducted on mice sheds light on how that communication possibly happens: certain live bacteria may travel from the gut to the brain through the vagus nerve.
A team from Emory University in the United States utilized various mouse models to simulate ‘leaky gut’ conditions. This included high-fat diets aimed at triggering atherosclerosis and genetically modified mice resembling those with Alzheimer’s and Parkinson’s diseases.
This gut damage can allow bacteria to enter the bloodstream, leading to infections. However, in this study, researchers discovered minute amounts of bacteria similar to gut microbes in the brain, without any detectable levels in the blood.
Interestingly, these bacteria appeared in the brain regardless of whether the gut leakage was induced by diet or disease models. Further tests indicated that the vagus nerve, which serves as a primary pathway from the gut to the brain, significantly reduced the presence of bacteria in the brain when blocked. This suggests that the vagus nerve could indeed be a conduit for bacteria.
According to the researchers, this data indicates a bacterial translocation route from the gut to the brain that is influenced by both environmental and genetic factors, meriting additional research to see if similar phenomena occur in humans.
The notion that bacteria can access the brain from the gut through the nervous system isn’t entirely new, but this study provides compelling evidence in mice. Traces of bacteria have previously been identified in the brains of individuals who succumbed to Alzheimer’s, yet the current findings show live changes in living mice.
When gut microbes were transferred to mice, the bacteria were found exclusively in the gut and brain, not elsewhere in the body.
However, there are important caveats to consider. Besides being conducted on mice rather than humans, the quantity of bacteria reaching the mice’s brains was very small, leaving questions about whether it could actually trigger inflammation or disease.
Future studies may explore this further. Several past investigations have linked gut inflammation to neurodegenerative disorders like Alzheimer’s, as well as mood disorders, though clear causal relationships remain uncertain.
Looking ahead, it might become feasible to treat certain neurological and mental health issues through drugs designed to alter the gut microbiome, although establishing a clear cause-and-effect relationship is essential first.
A microbiologist from Emory pointed out that one of the significant implications of this study is that the onset of neurological conditions might very well start in the gut. This perspective could pivot the focus towards the gut for therapeutic interventions regarding brain conditions, potentially changing treatment for those with neurological issues.
Researchers are currently exploring various avenues for how the gut and brain communicate, including immune responses, nervous system interactions, and numerous biochemical reactions. This latest study proposes a more direct connection, with bacteria traveling from the gut to the brain under certain conditions.
One positive aspect of the findings is that when mice on high-fat diets returned to normal eating patterns, the bacteria levels in their brains dropped significantly, indicating that damage caused may be reversible by addressing gut leakiness.
This underscores the intricate connections within our bodies—problems in one area can quickly impact another. The gut-brain axis, in particular, exemplifies this phenomenon.
The research prompts further exploration into how dietary changes can profoundly affect human behavior and neurological health, emphasizing the need for more studies in this area.
This research has been published in PLOS Biology.