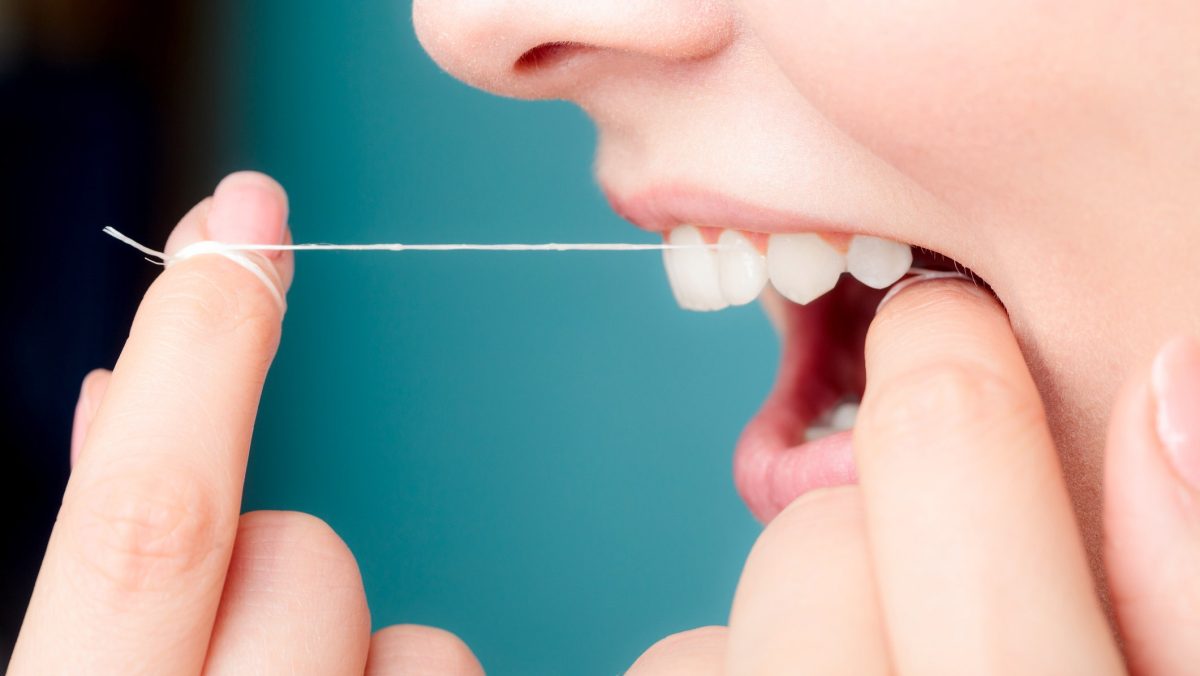
Flossing as a Novel Vaccine Delivery Method
Dental floss might do more than just keep our teeth clean. Recent research from the Texas Institute of Technology and the University of North Carolina indicates that it could potentially serve as a vaccination tool.
In experiments involving animal models, scientists found that dental floss can release vaccines effectively from the tissues between teeth and gums.
The study found that flossing could lead to increased antibody production on mucosal surfaces, such as those in the nose and lung linings. These findings were reported in the journal Nature Biomedical Engineering.
Harvinder Singh Gill, a chemistry and biomolecular engineering professor at North Carolina State University, pointed out the significance of the mucosal surface, noting its role in the entry of pathogens like influenza and COVID-19. Traditional vaccination methods mainly generate antibodies in the bloodstream, while mucosal delivery can enhance immunity right where pathogens might invade the body.
Flossing, in this context, uses the “junctional epithelium,” a thin layer of tissue found in the gaps between teeth and gums, which lacks the protective barriers present in deeper tissues. This means immune cells can be more readily activated.
In their study, researchers applied a peptide influenza vaccine to dental floss before using it on the teeth of lab mice, comparing the effectiveness of this method to nasal or oral vaccine delivery techniques. Results indicated that flossing can lead to much stronger antibody responses on the mucosal surfaces compared to traditional methods.
Interestingly, flossing techniques also provided protection against influenza virus similar to that achieved through nasal administration.
In addition to influenza, the researchers examined three other types of vaccines: protein, inactive virus, and mRNA. All of these tests showed robust antibody responses throughout the bloodstream and mucosal surfaces.
The research team plans to test the delivery of vaccines through human epithelial junctions using floss picks, which they hope will offer a less intimidating alternative to traditional needle injections.
One concern that arose is the feasibility of this approach for very young children or those with no teeth. Gill noted that understanding how this method will work for individuals with periodontal disease or other oral infections is imperative.
Hua Wang, a materials science assistant professor at the University of Illinois, commented on the study’s implications, emphasizing the potential for reducing fear and pain associated with needle injections. He mentioned that further exploration into local and systemic effects of this innovative vaccination method is crucial.
Researchers acknowledged a variety of limitations and emphasized the necessity for additional studies to understand the full scope of effects associated with floss-based vaccines.
Ultimately, while promising, this new approach will require thorough evaluation before it can be seen as a viable alternative to traditional vaccination methods.