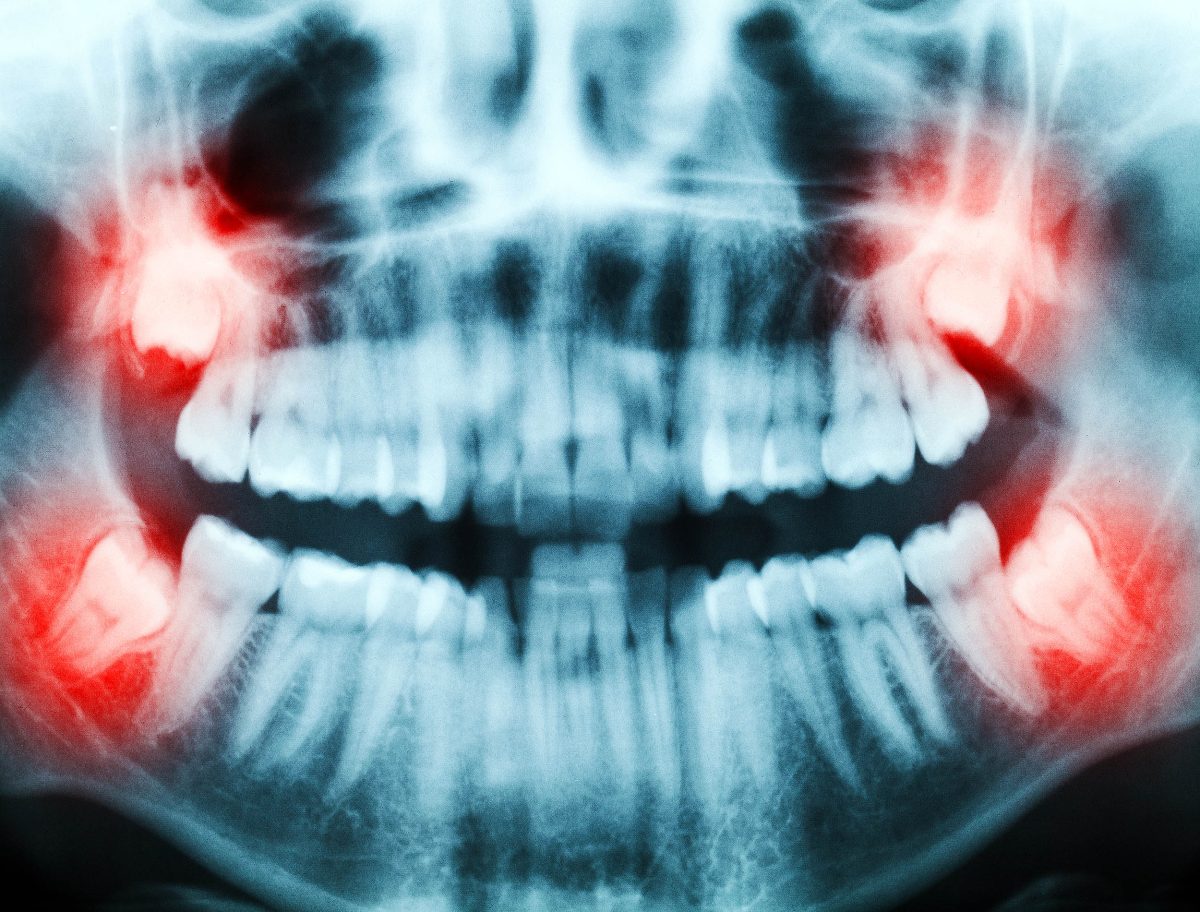
Each year, millions of Americans undergo wisdom-tooth surgery, often considering these third molars as just excess biological matter. Yet, it turns out that they actually contain valuable dental stem cells, which could play a crucial role in treating various serious health conditions.
Your routine dental check-up might soon evolve into the beginning of a custom medical strategy, as researchers have discovered that wisdom teeth house stem cells capable of regenerating bone, cartilage, and even nerve tissue.
The study was led by Dr. Gaskon Ibarretxe, an associate professor at the University of the Basque Country.
Unlocking hidden cells
Wisdom teeth contain a soft core known as dental pulp—a vascular inner layer that ensures the tooth stays alive.
Researchers have managed to isolate cells from this pulp that act like young builders in the body, showing potential to become neurons, heart muscle, or bone when cultivated in the lab.
Ibarretxe’s team even transformed these pulp cells into neuron-like cells that can generate electric signals similar to those in real neurons. “This transition from expressing markers to showing real electrical activity is vital, since damaged brain pathways require cells capable of sending signals,” Ibarretxe highlighted.
Harvesting stem cells from teeth
In the U.S., about 10 million wisdom teeth are extracted annually. Most of these teeth go straight to biomedical waste, but each tooth removed represents a painless source of live tissue.
Typically, dentists operate on teenagers or young adults when the pulp cells are still actively dividing and have fewer DNA errors.
Some labs collaborate with oral-surgery clinics to store teeth on dry ice before sending them to facilities where the pulp is processed and stored in liquid nitrogen.
One such service, Stemodontics, refers to this practice as “biological insurance.”
Dental stem cells as medical assets
Often, extracted wisdom teeth are discarded without much thought. However, several companies now offer preservation kits that can turn these seemingly useless teeth into long-term health resources.
These kits include everything necessary to keep the stem cells in the pulp viable during transport and are sent to dental offices ahead of time.
Unlike embryonic or cord-blood stem cells, dental pulp stem cells come with minimal ethical dilemmas since the tissue would otherwise be thrown away. This makes them a more accessible option for expanding personalized regenerative therapies, especially as the costs for stem cell banking decrease.
Dental stem cells and disease
Pre-clinical studies suggest that dental pulp cells could alleviate motor issues in mouse models of Parkinson’s disease by replacing lost dopamine-producing neurons.
In research focused on Alzheimer’s, these cells are noted for secreting growth factors that protect synapses and might aid in slowing down the buildup of harmful proteins. A 2024 review discussed how pulp-derived cells help eliminate amyloid plaques and reduce brain inflammation.
Clinical progress is underway. Recent reports indicate early-phase trials where stem-cell implants successfully produced dopamine in Parkinson’s patients, even though those trials utilized embryonic stem cells. Dental stem cells could potentially offer similar benefits without the ethical complications.
Building a personal biobank
Storing one’s own dental stem cells could mitigate concerns over immune rejection, speeding up treatment timelines that typically necessitate donor matching.
The extraction is fairly straightforward: the oral surgeon places each tooth in a sterile container, and couriers promptly deliver this to a lab where the pulp cells are thawed, isolated, and frozen within 24 hours.
The initial costs are comparable to that of cord-blood banking, but the potential return spans decades since adult stem-cell lines can be expanded repeatedly for various therapies.
Stem cells used in multiple health issues
Apart from nervous system applications, dental stem cells can regenerate mineralized tissue quicker than those from bone marrow, which is particularly useful for jaw repairs following tumor surgeries.
Cardiologists have explored using dental-pulp secretions on mice with heart issues, discovering improved heart function, which hints at the potential for creating cardiac patches from a patient’s own molars.
Orthopedic researchers are also keen on these stem cells: in lab settings, they lay down collagen and calcium in organized sheets that mimic healthy cartilage, a prospect that could change joint repair techniques.
Breakthrough therapies for disease
Regulators will require long-term safety data, particularly since transplanted cells need to integrate without leading to tumors.
Plans are in place for multicenter trials that will compare pulp-cell implants to conventional deep-brain stimulation for movement disorders. If dental stem cells can restore function while reducing healthcare costs, it’s possible that dentists may soon start providing preservation kits alongside post-operative instructions.
However, there are equity concerns to address. Access to wisdom-tooth banking shouldn’t become a privilege reserved for those who can afford elective treatments. Community biobanks or insurance incentives could help bridge that gap.
In conclusion, the takeaway is straightforward: before discarding those molars, think about the regenerative potential they might hold. The next groundbreaking treatment for Alzheimer’s or spinal cord injuries could originate from what many view as just an inconvenience at the dentist’s office.
The study is published in Stem Cell Research & Therapy.