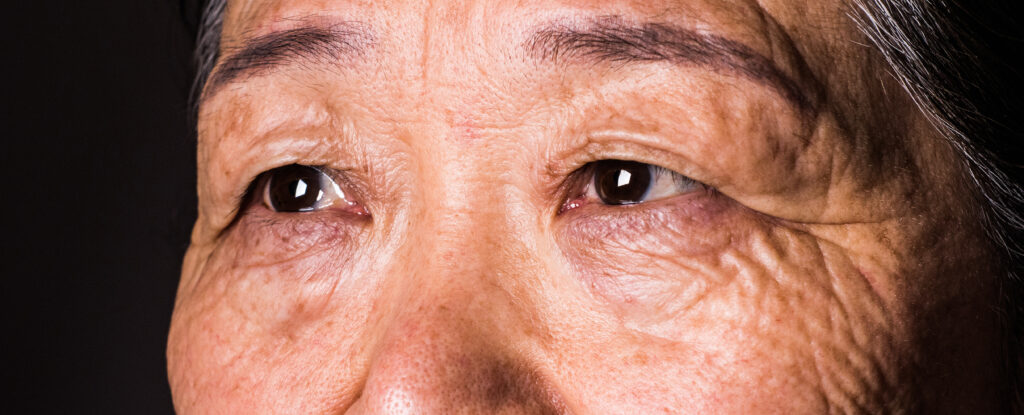
Eyes and Cognitive Health
The health of our brain can often be reflected in our eyes. In fact, eye issues might be some of the first indications of cognitive decline.
Recent research indicates that a reduction in visual sensitivity could predict dementia up to 12 years prior to an official diagnosis.
The study followed 8,623 healthy individuals in Norfolk, England, over multiple years. By the end, 537 participants had been diagnosed with dementia, allowing us to identify possible preceding factors.
Initially, participants took a visual sensitivity test where they pressed a button upon seeing a triangle emerge amid moving dots.
Those who later developed dementia were notably slower in spotting this triangle compared to those who did not.
What could explain this delay?
Visual problems might serve as an early warning sign of cognitive decline because toxic amyloid plaques related to Alzheimer’s disease typically begin affecting visual processing areas of the brain. As the disease advances, it encroaches on memory-related regions, making vision tests likely to reveal issues before memory assessments do.
Other visual processing difficulties associated with Alzheimer’s include challenges in recognizing object outlines and differentiating between colors. For instance, the ability to see blues and greens can be one of the first visual experiences affected, leading to real-life consequences that someone may not immediately notice.
Another early indication of Alzheimer’s is a weakness in the “inhibitory control” of eye movements, where individuals become easily distracted by external stimuli.
It appears people with Alzheimer’s struggle to disregard distractions, which may manifest as challenges in controlling eye movements. If dementia increases susceptibility to distraction, it could escalate the risk of driving accidents—a concern under investigation at Loughborough University.
Challenges in Facial Recognition
Evidence suggests that individuals with dementia may struggle to process new faces effectively. Instead of the usual scanning pattern—from eyes to nose to mouth—this inefficiency might hinder their ability to imprint faces for later recognition.
In fact, some healthcare professionals have noted dementia signs upon meeting individuals, observing that those affected often seem disoriented because they do not systematically search their surroundings or scan new acquaintances.
This early difficulty in recognizing newly met individuals could be tied to ineffective eye movement rather than simply a memory issue.
Can Eye Movement Enhance Memory?
Since visual sensitivity correlates with memory performance—even in non-visual assessments—there’s exploration into whether encouraging more eye movements may aid memory improvement.
Prior studies on this topic have mixed results, though some research indicates eye movements could boost memory. This might explain why individuals who tend to read more or watch television generally exhibit better memory and a lower risk of dementia.
While consuming content, our eyes frequently move back and forth across the text or screen.
Interestingly, those who read regularly usually have pursued more extended education. A solid educational background might provide a sort of brain reserve, allowing for greater resilience when brain connections deteriorate.
Some research has indicated that rapid lateral eye movements could also improve autobiographical memory. However, it seems this benefit may predominantly favor right-handed individuals, although the reason for this remains unclear.
Despite intriguing findings, therapies targeting memory issues through specific eye movements have not gained significant traction yet. Additionally, utilizing eye movement deficits for diagnostic purposes is still not commonplace, even with available eye-tracking technology.
One significant barrier may be the high cost and complexity of eye-tracking systems, which require specialized training for effective use. Until more affordable and user-friendly eye trackers become accessible, employing eye movements as a diagnostic tool for early-stage Alzheimer’s may remain confined to research settings.