Link Between Type 2 Diabetes and Schizophrenia Risk Found
A researcher from the University of Haifa has discovered that individuals diagnosed with Type 2 diabetes might face a 50% greater risk of developing late-onset schizophrenia compared to those who do not have diabetes. Interestingly, this risk appears to be even higher for women.
Lead researcher, Prof. Stephen Levine of the School of Public Health at Haifa, discussed these findings during a recent teleconference. “Type 2 diabetes is already linked to numerous health issues, such as heart disease and dementia,” he noted. “Our research indicates it also elevates the risk of schizophrenia in middle and older ages.”
These insights could facilitate the early identification of individuals at high risk, potentially leading to new healthcare protocols that integrate psychiatric monitoring into diabetes care.
The study monitored over 99,000 Israelis aged 51 to 71, all members of Meuhedet Health Services and without a history of either Type 2 diabetes or schizophrenia, from January 2005 to February 2020. It found that those with Type 2 diabetes were 50% more likely to develop schizophrenia, with the risk escalating to 64% in women and 39% in men, according to Levine.
This research was a collaboration with Prof. Arad Kodesh from Haifa’s Department of Community Mental Health and Meuhedet Health Services, alongside Prof. Abraham Reichenberg from the Department of Psychiatry at Mount Sinai Hospital in New York.
Published last month in the peer-reviewed journal Schizophrenia Bulletin, Levine offered a hopeful perspective: “The research might help prevent considerable suffering for patients and their families.”
Understanding the Connection
Levine proposed several reasons why Type 2 diabetes and late-onset schizophrenia may co-occur. One possibility is a shared genetic factor. For instance, a gene associated with diabetes, TCF7L2, has also been linked to an increased risk for schizophrenia.
Additionally, it’s noted that people facing their first episode of psychosis often present with abnormal blood-sugar levels. Lifestyle choices can also play a part; those with diabetes might struggle to maintain healthy habits, which could negatively impact their overall health and potentially lead to schizophrenia. Some research indicates that stress responses might raise the risk for both conditions.
Prof. Mark Weiser, a psychiatric division head at Sheba Medical Center, pointed out that certain medications prescribed for schizophrenia are known to increase diabetes risk. “So, when people with schizophrenia develop diabetes, we typically attribute it to the medication,” said Weiser, highlighting that these findings offer a different perspective, which is fascinating.
Interestingly, siblings of individuals with schizophrenia show a higher likelihood of developing Type 2 diabetes, hinting at shared familial risk factors. In women, declining estrogen levels post-midlife could also contribute to later-onset schizophrenia.
Levine thinks that diabetes care teams could incorporate brief psychological screening tests for their patients.
Exploring a Complex Relationship
Having devoted two decades to studying schizophrenia, including its risks among Holocaust survivors, Levine notes significant evidence suggesting that those with schizophrenia face a higher diabetes risk. Certain antipsychotic medications can alter metabolism, increasing the likelihood of developing Type 2 diabetes.
Levine expressed his belief that the relationship could indeed work both ways. “Nobody had ever researched that before,” he said, having moved to Israel from Scotland in 1988. “I wanted to turn the research on its head.”
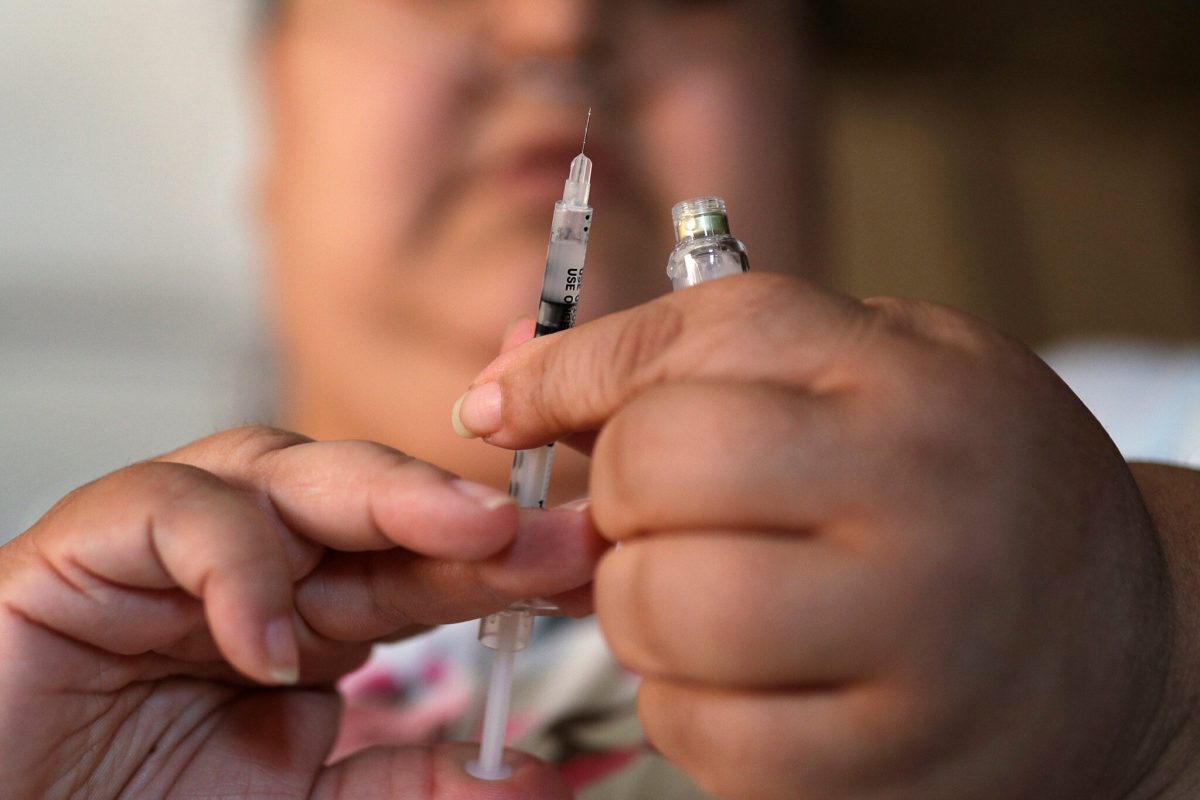
Type 2 diabetes, often linked with obesity and inactivity, is one of the most prevalent chronic diseases globally. Characterized by high blood sugar, it poses multiple health risks, from heart issues to kidney problems.
As diabetes rates grow, Israel has seen a slight increase, from 6.6% of the population in 2012 to 7.4% in 2023, according to Health Ministry statistics.
Globally, nearly 600 million people were living with diabetes as of 2024, a figure projected to exceed 850 million by 2050, with the highest rates anticipated in the Middle East and North Africa, per the International Diabetes Federation.
Levine noted, “The most concerning aspect is the clear global rise in diabetes.” Many contributing factors, particularly related to lifestyle choices, are preventable.
Schizophrenia affects about 1% of people worldwide, including those in Israel, typically beginning in a person’s early 20s. “Individuals with this disorder experience hallucinations, delusions, and cognitive impairments,” Levine explained, emphasizing the lifelong challenges and societal stigma associated with it.
While it’s uncommon to see schizophrenia emerge in midlife, the study’s findings indicate a significant increase in cases among those with Type 2 diabetes. Levine noted there were about 1.2 cases per 100,000 people annually without diabetes, whereas among diabetics, this figure rose to approximately 2.6 cases.
“Given that individuals with diabetes often experience higher rates of depression,” he stated, “it may benefit doctors to include a few additional questions to address potential psychotic experiences.” Identifying psychosis early in diabetic patients could alleviate some suffering for both the patients and their caregivers.