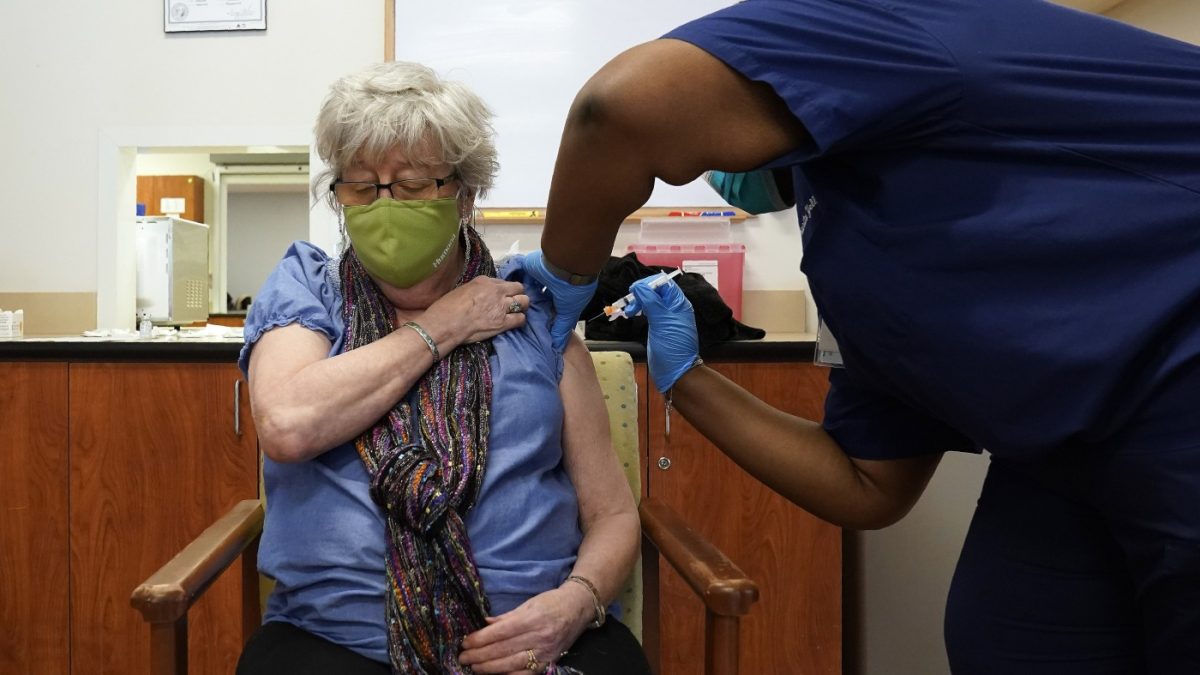
The recently approved Large Republican Tax and Expenditure Bill is expected to lead to cuts in federal support for health insurance markets created under the Medicaid and Affordable Care Acts. The Congressional Budget Office anticipates that these reductions may result in approximately 10 million Americans losing their health coverage by the year 2034.
Lawmakers have framed these cuts as essential for addressing growing budget deficits, which are, to some extent, worsened by recent increases in tax cuts and expenditures. However, they seem to overlook how these decisions could escalate costs across society, ultimately affecting hospitals, clinics, individuals, and, in turn, the federal budget.
Where will people turn for care without insurance?
Healthcare isn’t like other products—people can’t just stop needing it. So, what options do people have for medical care if they lack health insurance?
One avenue is through Federally Qualified Health Centers (FQHCs). These clinics offer a wide range of primary care, dental services, mental health resources, and specialized care for those with limited income. They typically charge a subsidized fee based on the patient’s ability to pay, focusing on individuals earning under 200% of the federal poverty level. FQHCs play a crucial role for the uninsured, operating roughly 15,000 locations that cater to over 31 million patients in 2023.
While cutting Medicaid might reduce taxpayer spending, it could also jeopardize FQHCs, which depend heavily on Medicaid income to subsidize care for uninsured patients. Without significant increases in federal grant funding, essential services offered by these centers might be at risk. Even with an anticipated grant of $5.6 billion in 2023, it may not be enough to offset the financial strain caused by declining Medicaid enrollments following the pandemic.
Hospitals as last-resort insurers
Hospitals face a variety of pressures, which compel them to treat patients regardless of their payment capabilities. For instance, federal laws require emergency departments to offer care to all individuals seeking help. Moreover, to retain their tax-exempt status, non-profit hospitals are obligated to provide community benefits through charity care or discounted services.
However, cuts to Medicaid won’t just affect clinics; they’ll also compound challenges for hospitals. A significant number are already operating at a loss, particularly in rural areas. The cuts threaten an additional 300 hospitals according to analysis, with some receiving a supplementary $50 billion to offset losses incurred from these Medicaid reductions.
Research highlights that hospitals often end up acting like “last resort insurance companies.” If Medicaid enrollment drops, the financial implications mainly fall on hospitals. In fact, in 2021, hospitals provided an estimated $22.5 billion worth of care to uninsured patients, with overall charity costs nearing $40 billion. This translates to an average of $11,000 per visit for uninsured hospital care.
As the number of uninsured individuals continues to grow, hospitals report increased costs for uncompensated care. Interestingly, for-profit hospitals note minimal impacts from these changes.
Medical Debt
Expanding the uninsured population significantly strains community health clinics and non-profit hospitals, but the financial burden also directly impacts patients themselves.
Even those with insurance can face crippling medical costs, high deductibles, and potential bankruptcy due to medical debt. According to an analysis, approximately 20 million adults—a significant 8% of the population—are dealing with some form of medical debt. Shockingly, 6% of adults owe over $1,000. Cumulatively, Americans are grappling with about $220 billion in medical debt, particularly affecting uninsured individuals, those with low income, and people with disabilities.
Studies emphasize that hospitalization dramatically increases the chances of financial ruin for patients, even for those who are insured, with an almost 40% increase in bankruptcy risk during hospitalization. Interestingly, historical data shows that extending Medicaid eligibility can significantly lower rates of bankruptcy, offering a pathway to greater financial stability for many.
Poor health has broader implications
Uninsured individuals face not just health issues but greater economic challenges; they, on average, receive less preventive care and struggle to access essential medications and specialized treatment. Their situation raises concerns beyond personal health, as a less healthy population can spell trouble for the economy at large. Research indicates that children who receive Medicaid are more productive adults, generating higher incomes and requiring fewer government benefits later in life.
Though government efforts to tighten Medicaid eligibility might yield initial savings, they threaten to destabilize other sectors. The ripple effects extend to community clinics, hospitals, and patients, highlighting the interconnected nature of healthcare and economic well-being.