BOSTON
Most residents in Massachusetts have health insurance, but a recent study reveals some significant challenges related to accessing care and affordability, particularly with high deductible plans.
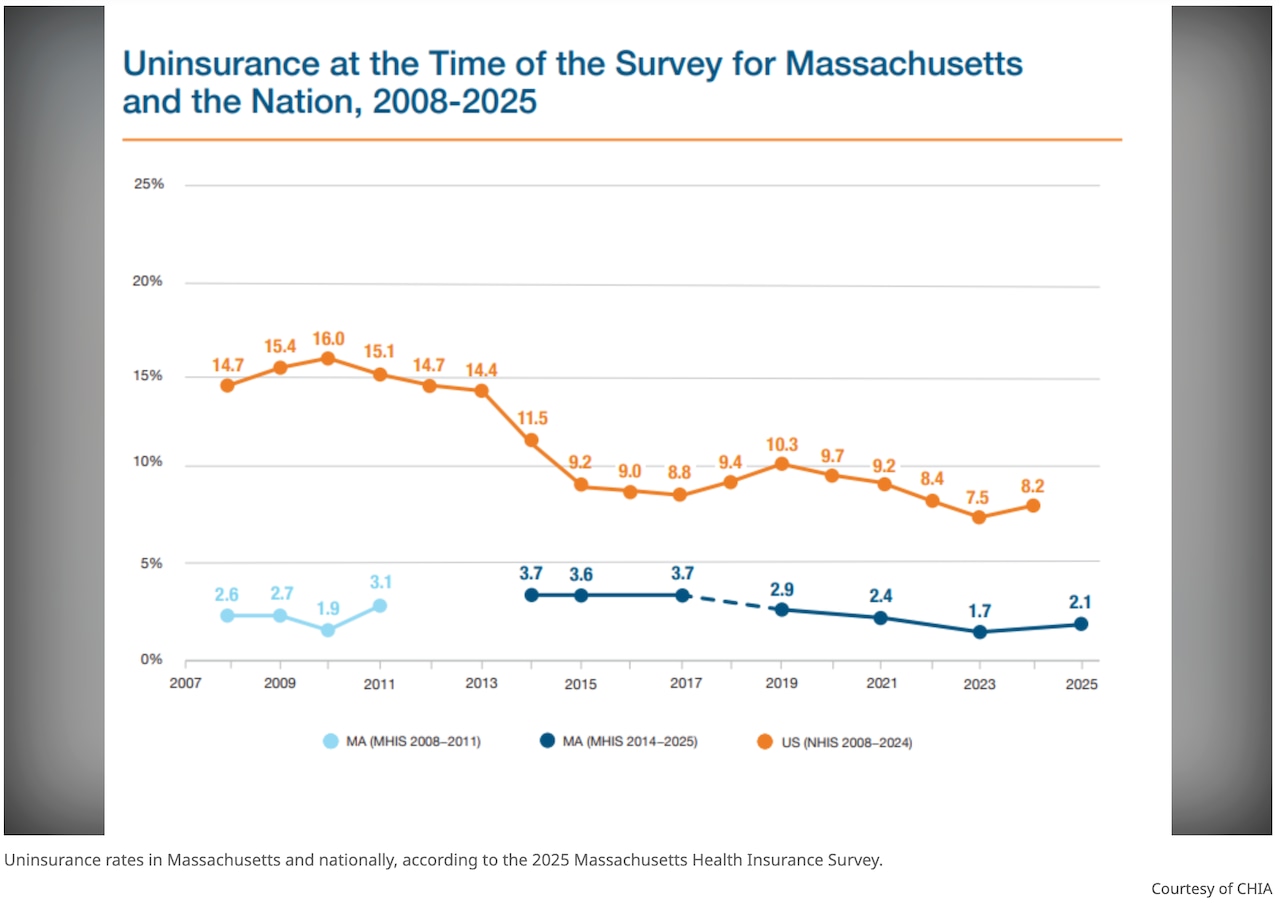
The uninsured rate in Massachusetts stands at 2.1%, significantly lower than the national average of 8.2%, according to the latest Massachusetts Health Insurance Survey published on Thursday. Moreover, about 90% of residents indicated that every household member maintained continuous insurance coverage over the past year.
The health care reform law enacted in 2006 by former Governor Mitt Romney aimed to ensure universal health care access.
Still, cost remains a barrier, as around 28% of residents noted they or a family member avoided seeking medical care in the previous year due to expenses.
The Health Information Analysis Center (CHIA) carried out this survey between January and April, interviewing 5,365 households. This initiative was partially supported by the Blue Cross Blue Shield of Massachusetts Foundation.
“With potential federal policy changes on the horizon, it is crucial to tackle the intertwined issues of access and affordability in Massachusetts,” stated Lauren Peters, Executive Director of CHIA.
The 2023 survey indicated that 98.3% of residents were insured, a rise from 97.9% in 2025. The survey results revealed that 139,741 residents in Massachusetts are uninsured, according to CHIA spokesperson Emma McNamara.
Health experts expect a considerable reduction in insurance coverage among MassHealth and the Massachusetts Health Connector due to upcoming federal policy adjustments. Interestingly, over 10,000 members of the Health Connector are facing increased premiums, prompting some employers to end coverage during the open enrollment season.
Most of the uninsured individuals are aged between 19 and 64, which reflects the existing safety nets like MassHealth for children and Medicare for seniors 65 and older. The data also pointed out that uninsured residents are disproportionately Hispanic, male, or belong to households earning below 300% of the federal poverty line.
The report identified high premiums and a lack of information on obtaining insurance as the leading reasons people choose not to purchase coverage. Massachusetts law mandates residents to acquire insurance or risk tax penalties.
Audrey Sheldt from the Blue Cross Blue Shield of Massachusetts Foundation warned that the uninsured rate could potentially double due to proposed Medicaid changes included in the One Big Beautiful Bill Act.
“Even with near-universal coverage, many are still struggling to access timely care or facing delays for financial reasons, especially in marginalized communities,” Sheldt remarked. “These findings should help direct policymakers to the barriers preventing timely and affordable care.”
About 46% of residents with commercial insurance reported having high-deductible health plans, which means higher out-of-pocket costs before coverage kicks in. According to the IRS, a high deductible is defined as being at least $1,650 for individual plans and $3,300 for family plans.
Notably, nearly 90% of those with medical debt stated they accrued it despite having insurance. Of those, 72% attributed their debt to deductible costs, while over half reported it was due to copays or coinsurance.
Fortunately, the proportion of residents unable to pay medical bills is declining – from 19.6% in 2014 to 13.7% in 2025.
CHIA reports indicate that individuals earning below 139% of the federal poverty level experience some of the lowest rates of medical debt. This may be linked to MassHealth eliminating all copayment and cost-sharing requirements for those under this income threshold.
However, about one in five residents faced administrative issues related to health care and insurance last year. The most common complaint was about resolving insurance claims, followed by challenges in obtaining information regarding coverage, issues with providers, and difficulties with prior authorization.
On the positive side, 87.5% of residents had a “usual source of care”, while 90.4% had a primary care provider. Among different racial groups, 92.4% of white residents reported having a primary care provider, compared to 87.4% of Black residents and 83.7% of Asian residents.
Despite this, roughly 43% of individuals encountered obstacles while trying to access care. About 30% faced issues getting timely appointments for primary care, managing administrative barriers, or dealing with recent clinic closures.
Looking ahead, there’s talk of a primary care bill being up for consideration in 2026. Advocates have long been pressing lawmakers to pass reforms aimed at strengthening the primary care system to cut down wait times and improve access.
Moreover, over one in five residents sought behavioral health care in the past year. The survey indicated that more than one-sixth of those obtained services fully out of pocket, often because their providers didn’t accept insurance.
Approximately 10% of residents reported unmet needs for behavioral health care in the last year, with 5.4% citing costs as a barrier.
Finally, just under one in four residents went to the emergency room in the past year, a figure that remains lower than pre-pandemic statistics. Almost a third of those visits might have been avoidable had non-emergency care been readily accessible. The CHIA noted no “statistically significant” difference in emergency department visit rates over the last few years.