Concerns Over Evolving Typhoid Bacteria
A long-existing threat, the bacterium that causes typhoid fever, has become increasingly dangerous as it mutates to evade medications.
Known as Salmonella enterica serovar Typhi (S Typhi), this bacterium has developed resistance to commonly used antibiotics.
In 2022, researchers collected over 4,000 strains from blood samples across more than 70 countries, identifying many as extensively drug-resistant (XDR) Typhi.
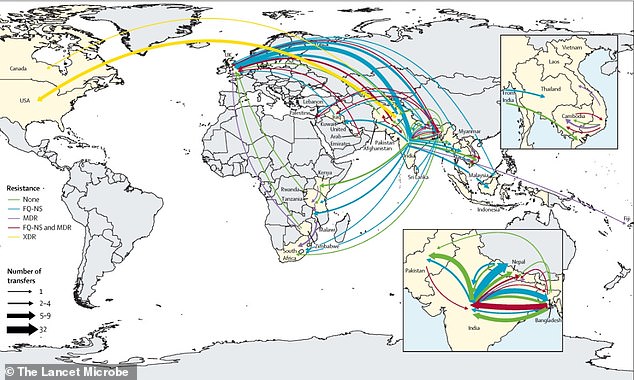
Since 1990, resistant strains have crossed borders approximately 200 times. Infected individuals often transport these strains to new locations, while the global food trade spreads these bacteria to crowded urban areas with inadequate sanitation, compounding the issue.
Experts warn that antibiotics like Ampicillin, Chloramphenicol, and Azithromycin may not be as effective in saving lives as they once were.
Annually, about 5,700 Americans contract typhoid fever, with 620 requiring hospitalization. Fatalities are rare in the United States.
Dr. Jason Andrews, an infectious disease specialist at Stanford University and the lead author of the study, expressed that the rapid spread of S. Typhi is particularly alarming.
Typhoid fever affects 11 million individuals globally each year, leading to symptoms like fever and abdominal pain. If untreated, it can result in intestinal bleeding and sepsis, claiming around 100,000 lives worldwide annually.
Without treatment, about one in five typhoid cases can be fatal.
When bacteria mutate to resist antibiotics, doctors are left with limited options for treating patients who exhibit symptoms of typhoid.
The research team analyzed the genetic profiles of over 7,600 S. Typhi samples, including almost 3,500 from cases in Bangladesh, India, Nepal, and Pakistan between 2014 and 2019.
They examined older samples dating back to 1905, scrutinizing the genetic makeup for changes that allow the bacteria to evade antibiotic attacks.
These adaptations enable the bacteria to produce enzymes that neutralize drugs, expel antibiotics, or utilize alternative biochemical routes for survival.
The researchers cautioned that the rapid mutation rate of typhoid bacteria is outpacing modern medical responses, suggesting that by the time vaccines are developed based on current resistance data, it may already be too late to implement effective measures.
South Asia remains a critical area for the emergence and spread of resistance.
Since 1990, quinolone-resistant strains have developed independently at least 94 times, with 97 percent of these cases linked to South Asia—especially India, Pakistan, Bangladesh, and Nepal.
What was once localized resistance, affecting 85 percent of typhoid cases in Bangladesh in the early 2000s, has significantly escalated, surpassing 95 percent in neighboring countries within a decade.
The situation is similarly alarming for newer antibiotics. Azithromycin resistance has arisen seven times since 2003, with strains from Bangladesh increasing steadily since 2013. Resistance to last-resort antibiotics, cephalosporins, is now emerging as the next significant challenge.
While these resistant strains mainly arise in South Asia and spread to Southeast Asia, East Africa, and Southern Africa, they have also been identified in the US, UK, and Canada.
Dr. Andrews emphasized that the international spread of resistant S. Typhi underscores the necessity to approach typhoid control and antibiotic resistance as a global concern.
The study findings were published in The Lancet Microbe.
Typhoid is rare in the US and usually occurs after international travel. It primarily impacts individuals in regions with poor sanitation, with children under five at greater risk.
In 2018, a daycare in Massachusetts temporarily shut down due to a child’s typhoid diagnosis, likely contracted during international travel.
The typhoid bacterium spreads via fecal-oral transmission, meaning it can be ingested through contaminated food, water, or surfaces that have come into contact with fecal matter. This often results from inadequate hygiene practices after using the restroom.
The study does have some limitations. Researchers pointed out that there was insufficient genetic data from critical regions, particularly Africa and Oceania, where typhoid is prevalent. This gap complicates efforts to monitor the spread of resistant strains.
Even in countries with rigorous monitoring, many samples are gathered from limited locations that may not represent the broader situation.
Moreover, as only a small percentage of typhoid cases undergo genetic testing, the actual extent of antibiotic resistance and its global reach might be underestimated.
This situation highlights the pressing need to enhance genomic surveillance to gain a clearer understanding of the emergence and spread of antibiotic-resistant organisms.