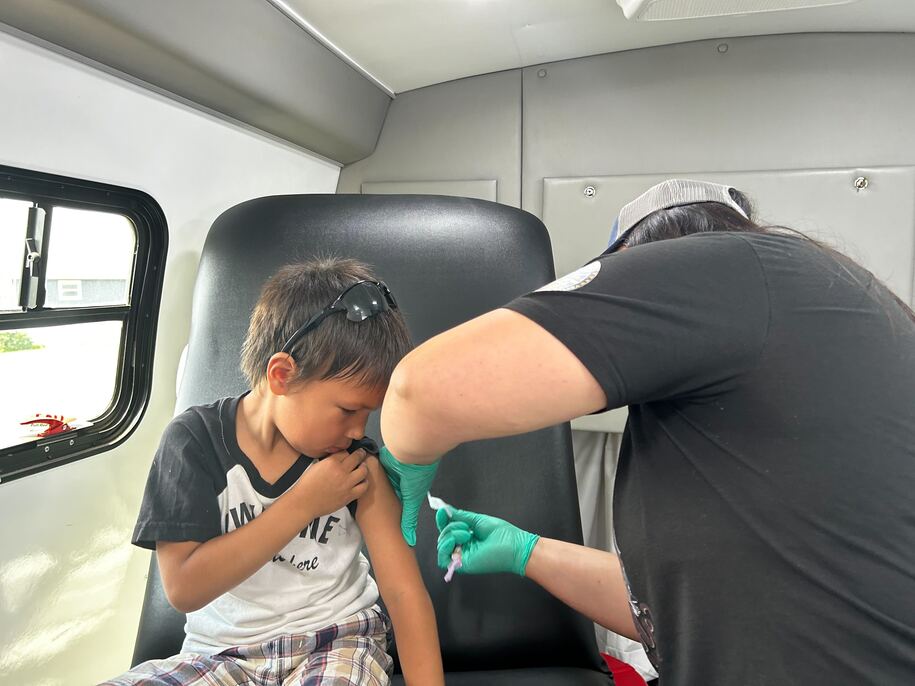
Cassandra Palmier intended to get her son his second and final measles vaccine dose, but car troubles made things tricky. So when she discovered a mobile clinic was coming to her area, she jumped at the chance to take him.
“I was really worried about the outbreak and measles,” Palmier, who is part of the Oglala Sioux Tribe, shared during the June event. “I felt it was important to help.”
Her son, Makaito Cuny, echoed that sentiment. “I’m not going to be scared,” the 5-year-old declared as he confidently boarded the clinic bus and settled into an exam chair.
Makaito stayed still while a nurse administered the shot. “I did it!” he exclaimed, flashing a big smile at his mom.
The vaccination clinic was organized by the Great Plains Tribal Leaders’ Health Board, which serves tribes across Iowa, Nebraska, and the Dakotas. This is one way Native American tribes and organizations are tackling the challenges of low measles vaccination rates and the difficulties people face in accessing health care as the disease spreads nationally.
Meghan O’Connell, the board’s chief public health officer, mentioned they are also collaborating with tribes interested in hosting similar vaccine clinics.
Additionally, tribal health organizations have begun social media campaigns, ensured their health providers are vaccinated, and reached out to parents of children who have not yet received the vaccine.
This spring, Project ECHO at the University of New Mexico offered an online video series about measles aimed at healthcare providers and organizations serving Native American communities. The sessions covered the essentials of diagnosing and treating measles and discussed culturally relevant communication strategies while sharing how different tribes are dealing with the outbreak.
Participants brainstormed methods to boost vaccination rates, according to Harry Brown, a physician and epidemiologist for the United South and Eastern Tribes, a nonprofit working alongside 33 tribes in the Atlantic Coast and Southeast regions. “It’s a pressing issue in Indian Country, and I think many people are becoming proactive,” he commented.
Measles can linger in the air in spaces where an infected individual has been—sickening up to 90% of those unvaccinated—according to the CDC. The United States recorded 1,319 confirmed measles cases this year as of July 23, marking the largest outbreak since 1992. Notably, 92% of those cases involved unvaccinated individuals or those with uncertain vaccination statuses. Tragically, three deaths and 165 hospitalizations were reported by the CDC up to that date.
O’Connell stated that while data on Native Americans’ vaccination rates might not be entirely accurate, it often indicates a lower percentage of vaccinated individuals compared to the overall U.S. population. The national data relies on small survey samples of self-identified Native Americans. Some data suggest slightly lower measles vaccination rates among Native Americans, while others indicate more significant gaps.
For instance, some states, such as South Dakota and Montana, have shown that Native American children are less likely than their white peers to receive vaccinations on time.
The national measles vaccination rate is particularly low for Native Americans who rely heavily on the primarily rural Indian Health Service. Approximately 76% of children aged 16 to 27 months had received their initial shot, according to data collected by the agency during recent patient visits at 156 clinics. This represents a 10-percentage-point decrease over the last decade.
Nonetheless, the IHS data indicates that its patients are at least as likely as others to have completed their measles vaccinations by age 17. It remains uncertain whether currently unvaccinated individuals will catch up on their shots in the future or if they will stay unvaccinated.
Immunization rates are probably higher among older children since schools require vaccinations unless exemptions are in place, Brown noted. He emphasized the importance of parents getting their children vaccinated promptly when they are younger, as they are at greater risk of hospitalization or death due to the disease.
O’Connell highlighted that Native Americans may face barriers to receiving vaccinations and health care in general, especially those on rural reservations that can be over an hour away from a clinic. Some, like Palmier, may struggle with unreliable transportation.
Another factor, O’Connell mentioned, is the mistrust some Native Americans have towards the Indian Health Service, which is often underfunded and understaffed. If the nearest health facility is operated by the agency, patients may postpone or forgo care.
O’Connell and Brown noted a growing vaccine skepticism and mistrust of the entire health care system within Native American communities, a trend seen nationwide as well.
“Before social media, our community had generally trusted childhood vaccinations. Historically, American Indians have faced severe impacts from infectious diseases,” Brown explained.
The arrival of European colonizers in the late 1400s introduced new diseases, including measles, that led to the death of millions of Indigenous people in North and South America by the early 1600s. Native Americans have also experienced high mortality rates during recent pandemics, such as the 1918-20 Spanish flu and COVID-19.
The Great Plains Tribal Leaders’ Health Board quickly responded as measles cases began surfacing near its South Dakota headquarters this year. Nebraska health officials reported in late May that a child in a rural area had measles, close to the Pine Ridge Indian Reservation. Later that month and into mid-June, four individuals from the Rapid City region also fell ill.
“Our phones were inundated” with inquiries once the news broke, according to Darren Crowe, a vice president at the Oyate Health Center in Rapid City. Parents were eager to confirm if their children were up to date on their measles vaccinations.
Crowe revealed that the health board ordered additional masks, created a measles response team that meets daily, and contacted parents when their database indicated their children needed shots.
Brown commended this outreach strategy. “It really requires a focused effort that engages people individually,” he remarked, noting his organization assisted the Mississippi Band of Choctaw Indians and the Alabama-Coushatta Tribe of Texas in similar initiatives.
However, reaching specific families can be challenging in low-income communities, where phone numbers often change due to the use of temporary prepaid plans. Once health workers contact a parent, Brown recommended they listen first before explaining the importance of vaccination against measles, mumps, and rubella.
“Instead of just lecturing, it’s better to understand their perspective first. Ask them, ‘What has your experience with vaccination been like? What information do you have about it?’” he advised. Most parents tend to agree to vaccinate their children when approached in a supportive and nonjudgmental manner, Brown noted.