Natalie Reichel Faces Uncertainty Over Cancer Treatment
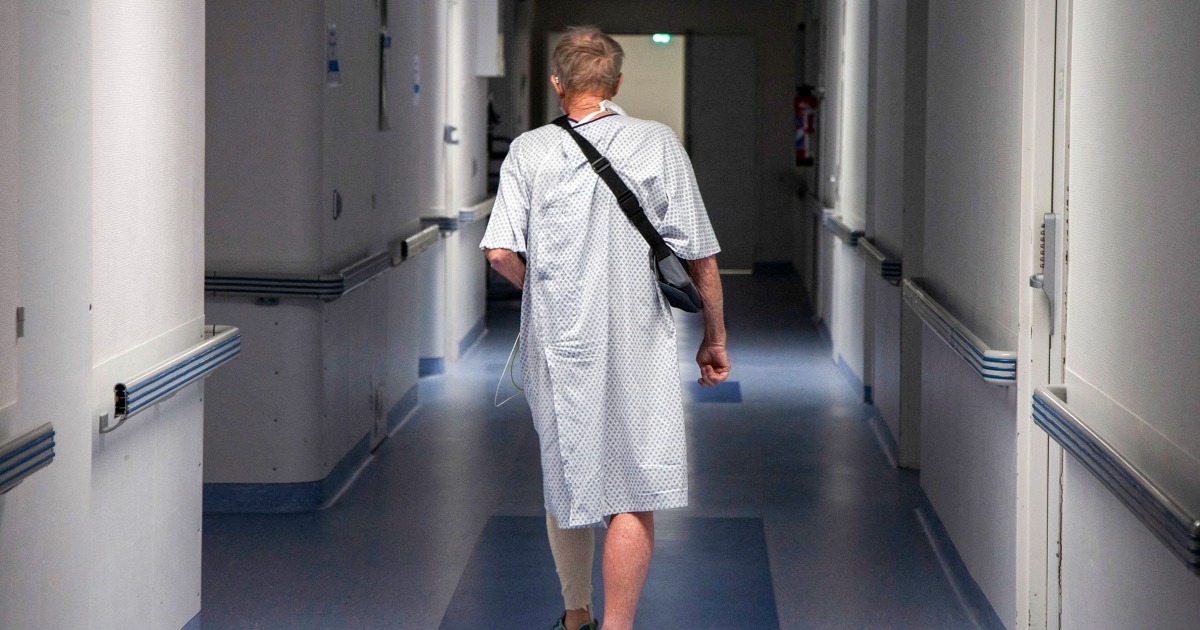
Natalie Reichel is set to begin her next round of cancer treatment in March, but a disagreement over a contract between Mount Sinai Health System in New York City and Anthem Blue Cross Blue Shield has cast doubt on whether she’ll receive her care on time.
“I’m feeling a bit suspicious,” the 40-year-old Reichel expressed.
The root of the issue appears to be financial. Mount Sinai is claiming that Anthem carries over $450 million in debt and is demanding a 50% increase in their rates. As a result of the parties not reaching an agreement, Mount Sinai doctors were removed from Anthem’s network starting January 1, although patients can still access city hospitals and facilities within the network until March 1. It’s estimated that around 200,000 patients at Mount Sinai have Anthem coverage.
This situation places Reichel in a tough spot, as she may need to obtain special approval for continuity of care or potentially find a new set of specialists to ensure her treatment schedule remains on track.
Diagnosed with breast cancer at just 33 years old, Reichel has been in remission for about six years. She continues to receive hormone-suppressing injections to lower the risk of cancer recurring. “My wife is really concerned that it might come back, especially since it was so aggressive when I was younger,” Reichel shared.
Typically, hospitals and insurance companies renegotiate rates quietly, usually reaching a resolution before patients notice any disruption. However, recent years have seen a rise in public disputes, often leaving patients in the lurch.
Jason Buxbaum, a researcher at Brown University, notes that from June 2017 to May 2025, roughly one in five hospitals has faced at least one public issue with an insurer. About 8% of hospitals have temporarily exited the insurance networks during negotiations. Overall, there are about 500 to 600 public disputes annually between healthcare providers and insurers.
“This trend has definitely ramped up recently,” Buxbaum said. “There’s a real chance for things to go awry.”
The dispute also has caught the attention of key figures in the healthcare sector. For instance, United Healthcare informed members that unless an agreement is made, NewYork-Presbyterian could fall out of its network. The insurer recently missed a deadline with Memorial Sloan Kettering Cancer Center but managed to strike an agreement just after the cutoff.
Rising healthcare costs are a significant factor contributing to these disputes, according to Leemore Daffney, a public policy professor at Harvard. The American Hospital Association has reported a projected 5.1% increase in total hospital spending for 2024, considerably more than the projected inflation rate of 2.9%. This reflects an ongoing trend, although it’s expected to slow in 2025.
Relying on tools like prior authorizations and claim denials for cost-control, insurers are facing backlash from the public. Many now see contract negotiations as a primary strategy for addressing rising costs.
“Essentially, it’s a question of whether to lower rates or cut out high-cost providers entirely,” Daffney explained. “Insurance companies aim to provide access to quality care while keeping it affordable, which might mean resisting every price hike request, even if those providers face their own cost increases.”
Buxbaum adds that the introduction of federal transparency rules has increased disputes. Hospitals now need to disclose pricing, leading to competitive pressure on how much they charge.
“No one wants to be the lowest-paid provider in the area,” he remarked.
Daffney anticipates that these disputes will escalate, especially in Medicare Advantage plans, which are governed by private insurers. Unlike traditional Medicare, which allows patients to go to any provider, Medicare Advantage networks are usually smaller.
“There’s no doubt that these complexities are delaying care and causing suffering,” she stated.
Brent Estes, the chief administrative medical officer at Mount Sinai and the lead negotiator in the Anthem conflict, stressed that the hospital system is standing firm on its terms. They are willing to sign a new contract if Anthem agrees to their conditions.
“You can’t expect to maintain the same rates forever,” Estes noted. “We believe our payout rates are lower than what competitors are offering, which hampers our long-term viability.”
An Anthem spokesperson shared that the insurer’s priority is managing costs. They accused Mount Sinai of aiming to eliminate pricing protections that would lead to significant increases in healthcare costs.
Reichel’s insurance is managed by a third-party organization that utilizes Anthem’s network, which means Anthem cannot authorize her treatment directly. This complicates her ability to receive ongoing care amid the current situation.
Reichel mentioned she’s actively working to obtain the necessary approval while also stockpiling a three-month supply of her medication to prevent any potential gaps in her treatment.
As for whether a resolution will come about soon, she expressed doubt, saying, “I have a feeling I’m going to have to navigate more hoops. It just seems like I’ll be jumping through a lot of obstacles again.”