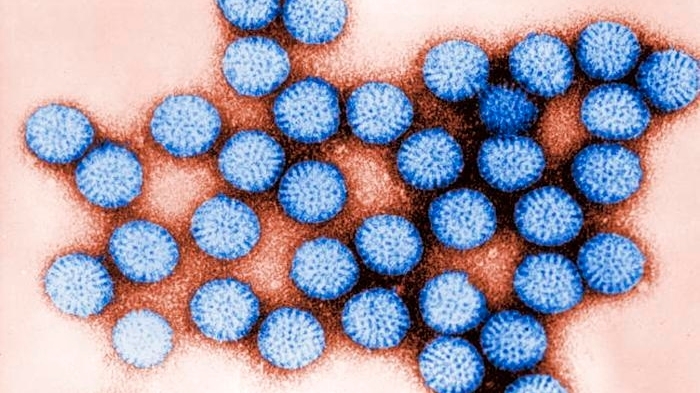
Rotavirus, a highly contagious illness that leads to severe vomiting and diarrhea in infants and young children, is seeing an uptick on Long Island, throughout the metropolitan area, and across the country. Health professionals caution that affected children can become so dehydrated that they might require hospitalization for intravenous fluids.
Earlier this year, federal health authorities removed the rotavirus vaccine from the recommended childhood vaccination schedule. Experts in infectious diseases have expressed concerns that this decision could lead to a decrease in vaccination among parents for their children in the future.
Before the latest vaccine was introduced in 2006, rotavirus was responsible for as many as 70,000 hospital visits and between 20 to 60 fatalities each year among children, according to the National Foundation for Infectious Diseases.
Here, we aim to answer some frequently asked questions about the disease.
Why is there a surge in rotavirus cases right now?
According to data from the Centers for Disease Control and Prevention, the percentage of positive rotavirus cases in the northeastern United States stood at 9.6% for the week ending April 11. This figure is higher than that of the previous two years around this time. Experts mention that rotavirus typically resurfaces in the spring, but various factors could be contributing to the increased cases this year.
“Kids tend to spend more time indoors during long winters,” noted Dr. Asif Noor, chief of pediatric infectious diseases at NYU Langone—Long Island, who’s observed a rise in hospital cases that aligns with regional and national trends.
“Rotavirus can spread quite rapidly,” Noor added. It seems fewer parents are opting for the vaccine for their kids.
What are the symptoms of rotavirus?
The primary symptoms include vomiting, diarrhea, fever, and abdominal pain. It’s important for parents and caregivers to recognize signs of dehydration in infants, which can sometimes be difficult. Signs include lethargy, reduced wet diapers, dry skin, and crying without tears.
How is rotavirus spread?
The virus is transmitted through the stool of an infected person, which can be found in tiny amounts on hands, surfaces, and even food, according to the CDC. Family members often contract the virus from children within the household.
“The virus can be present in stool two days before diarrhea starts and can last up to 10 days after symptoms begin,” Dr. Sharon Nachman, chief of pediatric infectious diseases at Stony Brook Children’s Hospital, explained. “So when kids return to school or daycare, they might still be infectious.”
How can I protect my child and myself from rotavirus?
While practicing good hand hygiene is advisable, it might not be sufficient to curb the spread of the disease entirely, the CDC states. The rotavirus vaccine, given in oral drops starting from two months after birth, is administered one or two more times before the child turns six months, depending on the formulation.
Nachman emphasized that the vaccine provides 98% protection against severe illness and 96% protection against hospital visits and emergency room trips.
A rise in vaccine hesitancy, combined with the recent decision by the Department of Health and Human Services to exclude it from recommended vaccinations, could result in a concerning spike in cases in the upcoming years.
Is rotavirus really a threat to my child’s health?
“This is a serious matter,” Noor stated. “Parents must be vigilant, as babies and toddlers can quickly become dehydrated. They shouldn’t hesitate to begin oral hydration at home and seek medical help if vomiting continues. Gastrointestinal illnesses, including rotavirus, remain one of the leading causes of death in children worldwide.”