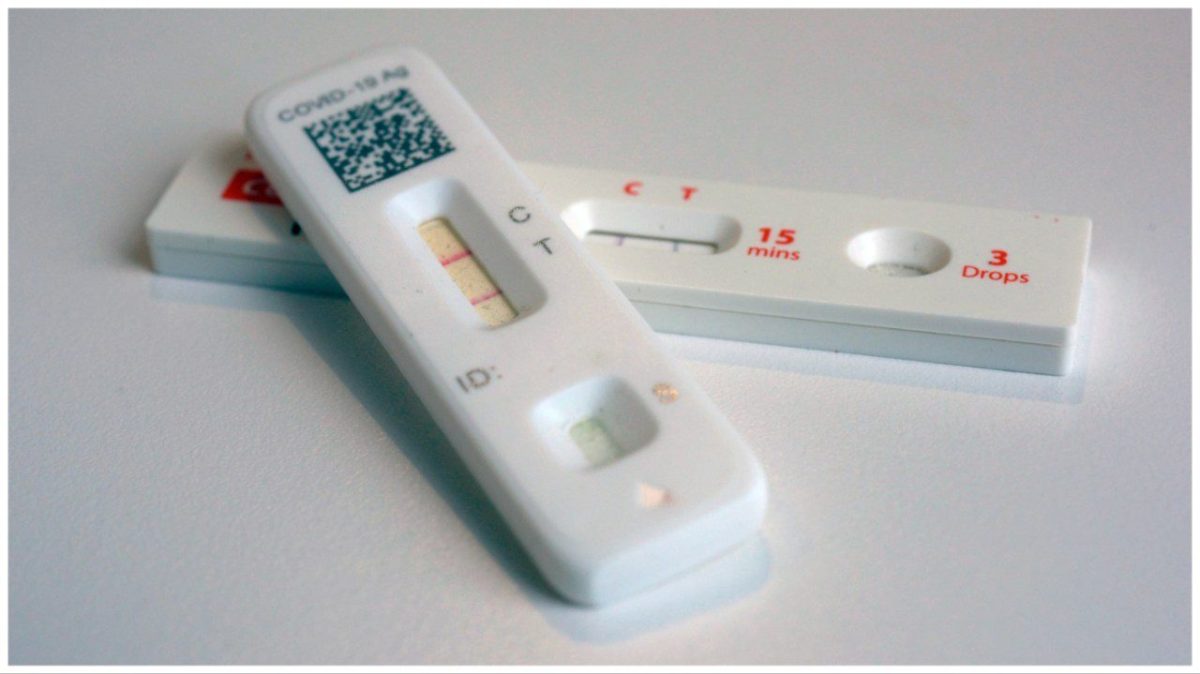
The United States is riding a new wave of coronavirus infections, with infections rising due to holiday gatherings and new variants.
Sewage virus activity levels for COVID-19 are at their highest since the 2022 micron surge, according to the Centers for Disease Control and Prevention (CDC).
At the same time, a new variant called JN.1 became the most dominant strain, accounting for about 44% of infections nationwide by mid-December, up from about 7% in late November.
Infectious disease experts say hospitals have sufficient capacity and many infections are relatively mild. Although the numbers have been gradually rising, the country has not experienced a major spike.
Still, the CDC is unable to track the actual number of people infected, especially since most people test at home or don't test at all. That's why experts say wastewater is one of the more accurate warning signs. Virus activity is highest in the Midwest.
The agency reported 29,000 hospitalizations in the week before Christmas, compared to 39,000 hospitalizations in 2022. The number of emergency department visits during the same period increased by 12% from the previous week.
Since Thanksgiving, an average of about 1,400 people have died each week from COVID-19.
That number has steadily increased this winter, and some hospital systems have reinstated mask mandates. Still, vaccination rates with the latest COVID-19 vaccines are extremely low, leaving infectious disease experts concerned for the most vulnerable.
According to the CDC, only about 19% of adults have received the latest vaccination, but that number could be slightly higher due to data limitations.
“When infections spread to such large numbers in the general population, the virus will infect more vulnerable populations, those who do not have up-to-date, up-to-date vaccines…those people are at higher risk and will require hospitalization. It's more likely.” William Schaffner, an infectious disease specialist at Vanderbilt University Medical Center, said:
The CDC's Dec. 22 report said the virus remains a “serious public health threat,” especially among the elderly, young children, people with compromised immune systems, people with chronic medical conditions, and those who are pregnant. This is especially noticeable for those who do.
A December report from the CDC found that nursing homes are among the most vulnerable to a COVID-19 outbreak, but fewer people have been up to date with COVID-19 vaccinations for a long time. Only about 33 percent of nursing home residents did.
Biden administration Health and Human Services (HHS) officials met with nursing home industry leaders on Wednesday to discuss low vaccination rates.
Katie Smith Sloan, president and CEO of LeadingAge, a nonprofit senior service provider organization, urged HHS to allow nursing homes to order single-dose vaccines. He called for alleviating logistical barriers to inoculation, such as increasing vaccinations and coordinating vaccines provided through hospitals. Allows for more direct communication with residents and families upon discharge.
“It is also important that HHS recognizes and acknowledges that nursing homes are part of a larger community. At a time when vaccination rates among the general public are appallingly low, for the benefit of the entire nursing home sector and surrounding communities, It is critical that public health officials educate the public more broadly,” Smith-Sloan said in a statement.
Schaffner said the high level of virus activity is partly due to seasonality, including holiday celebrations, travel and cold weather that brings people indoors, as well as the possibility that one variant may be more contagious. .
Part of the problem is that people may have the virus but not isolate because they can't or won't get tested. So if someone thinks they have a cold, it could be the coronavirus.
The federal government has largely stopped providing free coronavirus testing once the public health emergency ends, meaning employers may be less willing to cover coronavirus-related absences.
“Now you have to buy tests and they're quite expensive, so I think a lot of people develop symptoms and make assumptions about their illness, but they don't get tested. I think one of the reasons is to not get sick and stay isolated at home,'' Schaffner said.
Copyright 2023 Nexstar Media Inc. All rights reserved. This material may not be published, broadcast, rewritten, or redistributed.