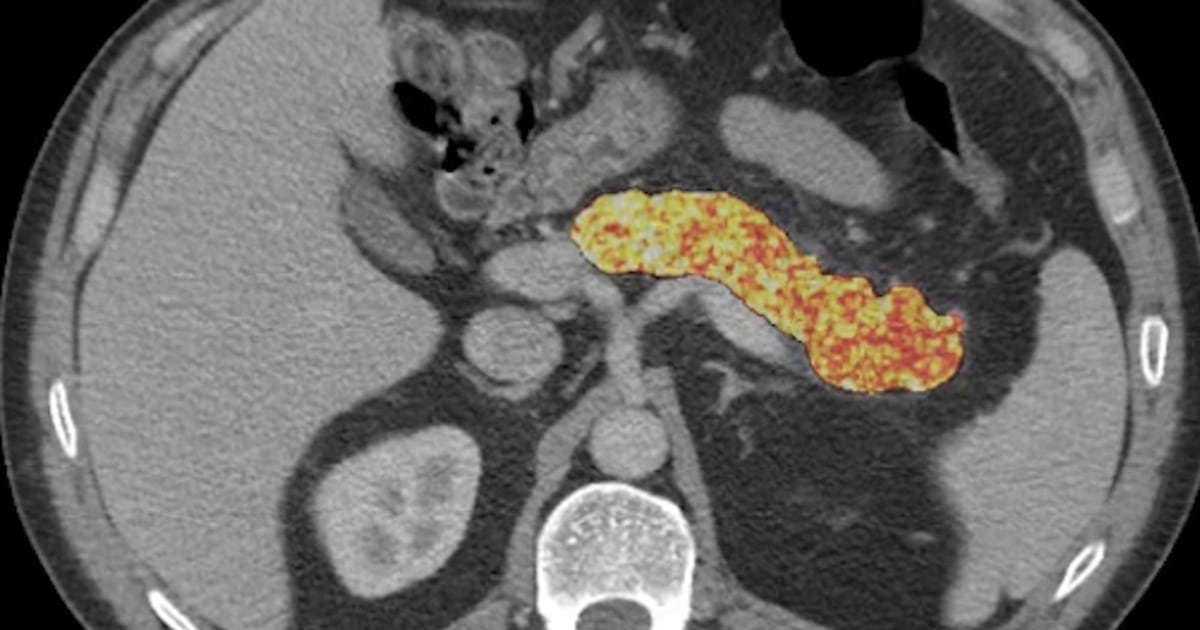
AI May Help Detect Pancreatic Cancer Early
Doctors often find pancreatic cancer only after it has become quite advanced, making effective treatment difficult. However, recent research indicates that artificial intelligence might help identify indicators of this disease even before tumors become visible on scans.
An AI model created by the Mayo Clinic in Rochester, Minnesota, revealed abnormalities in patients’ CT scans up to three years prior to their pancreatic cancer diagnosis. This finding was recently published in the journal Gut.
The development team trained the model using CT scans from patients who were initially screened for unrelated conditions but were later diagnosed with pancreatic cancer. Radiologists then reviewed these scans, comparing their ability to detect early signs of cancer with that of the AI model. Remarkably, the AI was found to be three times more effective at noticing those early indicators.
Dr. Ajit Goenka, a Mayo Clinic radiologist and author of the study, noted, “We understood that this disease doesn’t suddenly appear within three months… There was a signal there; we just had to uncover it.”
With a five-year survival rate hovering around 13%, pancreatic cancer is projected to become the second leading cause of cancer-related deaths by 2030. Alarmingly, about 80% of patients are diagnosed only after the disease has progressed significantly.
Unlike other cancers, like those affecting the colon or breast, there is no routine screening for pancreatic cancer in healthy individuals. Detecting a lump isn’t practical because of the pancreas’s location in the abdomen. By the time symptoms such as stomach pain or unexplained weight loss manifest, the cancer often has already spread to other organs.
Many early warning signs are too subtle to be detected with the naked eye. For instance, scans can look normal just six months before a diagnosis is made.
Dr. Daniel Jeong, a diagnostic radiologist not involved in the Mayo Clinic study, remarked, “I analyze these images daily. We’re often looking for a measurable mass, and those tumors need to grow to a visible size.”
One notable thing the AI model detected was abnormal cells in the pancreas that help protect cancer from the immune system. Although scientists have known about these cells, identifying them on scans has proven challenging.
Goenka believes this model could assist individuals who have risk factors for pancreatic cancer — like family history or diabetes — but haven’t shown any symptoms yet. From there, further blood tests and imaging would likely follow.
“If they do have symptoms and it turns out to be pancreatic cancer, AI wouldn’t be necessary,” he added.
This AI model is part of a series of recent advancements in the field of pancreatic cancer research. For instance, last month, early trial results showed that an mRNA vaccine helped extend survival in eight patients. Another drug, daraxonrasib, had promising results in a later-stage trial, potentially doubling some patients’ life expectancy. Recently, the FDA allowed its developer, Revolution Medicines, to expand access for patients in controlled settings who have already tried other treatments, although it is not yet FDA-approved.
Additional research is also focused on advanced blood tests that could help in earlier detection.
Dr. Tamas Gonda, director of the pancreatic disease program at NYU Langone’s Perlmutter Cancer Center, remarked that they’re making significant progress, though the disease hasn’t been turned around yet.
Other specialists not affiliated with the Mayo Clinic study emphasized that if the AI model successfully identifies signs of cancer before it spreads to major organs, it could increase the number of patients eligible for surgery, chemotherapy, or radiation.
Dr. Pam Hodul, a surgical oncologist at Moffitt Cancer Center, expressed hope: “This could really be a game changer for us in terms of early detection.”
AI is also showing potential in diagnosing a variety of other health conditions. A recent study published in the journal Science highlighted that AI performed on par with or even better than doctors in diagnosing emergency room patients.
Goenka mentioned that it could take some time before the Mayo Clinic’s model becomes available to the public, as the clinical trial will need to follow participants for three to five years to understand who develops cancer and who does not.
“In a field where we’ve felt lost for decades, this represents a milestone, but we still have to reach the finish line,” he concluded.