Colorado Health Insurance Enrollment Drops Less Than Expected
Connect for Health Colorado has reported a smaller-than-anticipated decrease in enrollment this year—just 2% instead of the projected 30% drop.
COLORADO, USA — This year, losses in Colorado’s health insurance market have turned out to be much lower than initial forecasts. Despite concerns raised by national leaders, who warned that failure to extend the premium tax credit could lead to a sharp decline in Affordable Care Act (ACA) enrollment, the actual drop remains minimal. Although a 2% reduction sounds better, it still translates to around 5,200 affected individuals, according to Connect for Health Colorado.
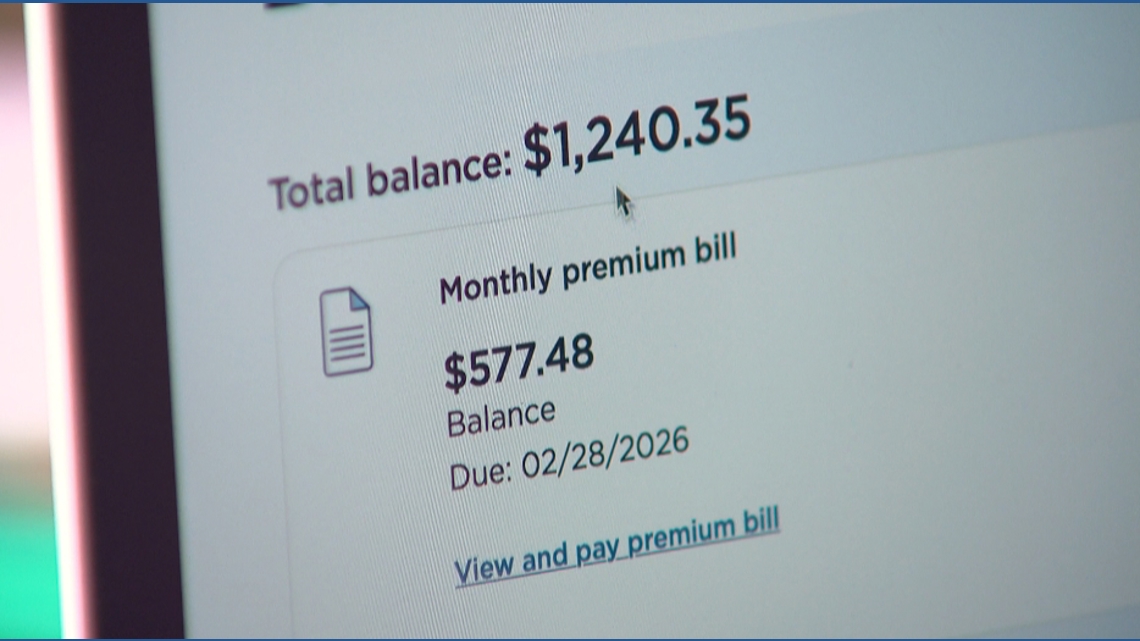
One of those facing the impact is Mercedes von Pichil, a small business owner and mother of two. After the expiration of the tax credit, her family’s health insurance premiums surged from $205 to over $577, forcing them into tough financial choices.
“This means one less person covered,” von Pichil noted.
She added that her husband has opted out of health insurance this year to cut costs.
“It feels unfair,” she said. “I want everyone to have access to health insurance without having to choose between essential needs. It just seems natural for us as humans to have that coverage.”
Von Pichil pointed out the increasing financial strain families are facing as medical expenses rise.
“I’m honestly shocked. I can’t work full time yet, so where am I supposed to find this unexpected money?” she expressed.
Her family does find some relief through Medicaid, especially for her newborn who is receiving treatment for a rare genetic disorder.
Kevin Patterson, the CEO of Connect for Health Colorado, indicated that the limited drop in enrollment can be attributed to a state program introduced last fall, which offered financial support to those losing premium deductions. He mentioned that approximately 69% of this year’s enrollees have received some form of aid.
“Feedback from brokers, assistants, and our own call center suggests this program has made a substantial difference, but it hasn’t entirely compensated for what people have lost,” Patterson explained.
For those benefitting from the program, premiums will be reduced by $80 for the first household member and $29 for each additional family member. Still, Patterson cautioned that this financial assistance might not be available next year.
“We are waiting to see what direction the state takes through the Joint Budget Committee and the budget process,” he stated. “While we celebrate the lower-than-expected losses, we’re aware that we need to address the needs of the 2% who experienced losses.”
Patterson emphasized that attention must be paid to the individuals particularly affected by these shifts in the ACA market.
“Some people are more impacted than others, and we’re looking for tailored solutions for those who are falling out of the ACA,” he said.