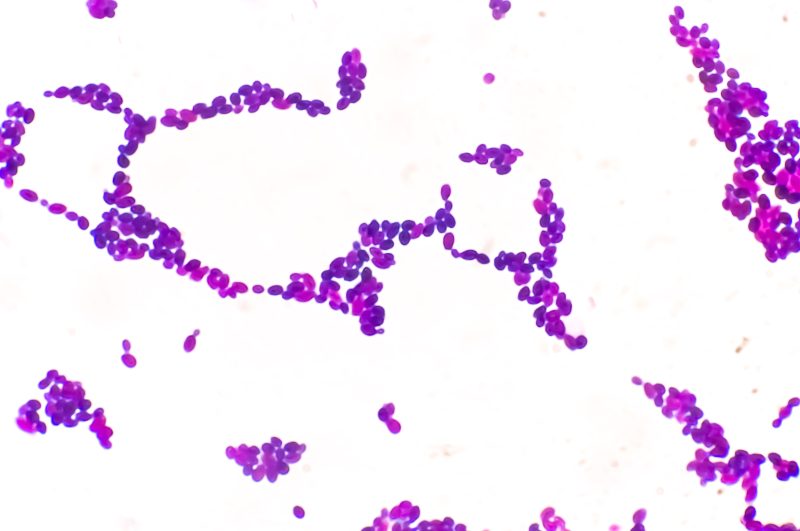
The bacteria Candida Auris, known for its resistance, is being closely monitored by health experts working to control its spread.
This fungus was first identified in the U.S. about ten years ago, and since then, the number of reported cases has risen each year.
According to data from the Centers for Disease Control and Prevention (CDC) for 2025, new cases of Candida Auris are mirroring last year’s figures. However, the distribution of cases varies significantly by state.
Out of 1,052 reported cases to the CDC so far in 2025, around 25% have been found in Texas, with 241 cases in the Lone Star State as of late April, based on the latest available data.
Other states with notable case counts include Michigan (185), Ohio (125), Virginia (99), and Arizona (98). Additionally, states like Colorado, Delaware, Illinois, Indiana, Iowa, Louisiana, Maryland, Montana, New Mexico, Pennsylvania, Utah, and Wisconsin are also seeing new cases this year.
It’s important to note that these case counts are preliminary and may change as more information is gathered.
The CDC has categorized this fungus as an “urgent antibacterial resistance threat” because it has developed resistance to treatments designed to eliminate it. When antifungal medications fail, the fungus can spread easily, complicating the treatment of related infections.
While individuals with healthy immune systems might combat infections effectively, Candida Auris primarily targets patients in healthcare settings who are already vulnerable.
Those at greatest risk include people with catheters, breathing tubes, feeding tubes, and PICC lines, as these devices can allow pathogens to enter the body.
The fungus can persist on various surfaces, including countertops and doorknobs, and can even exist on skin, making it easier to spread to susceptible patients.
“In general, they are very good at existing in environments,” noted Melissa Nolan, an assistant professor of epidemiology at the University of South Carolina, in a comment to Nexstar. “For instance, it can be present on a patient’s bed or on the railings.”
Historically, the CDC estimates that between 30-60% of those infected with C. Auris have died, though many of these individuals had other serious underlying health conditions that contributed to their risk of death.