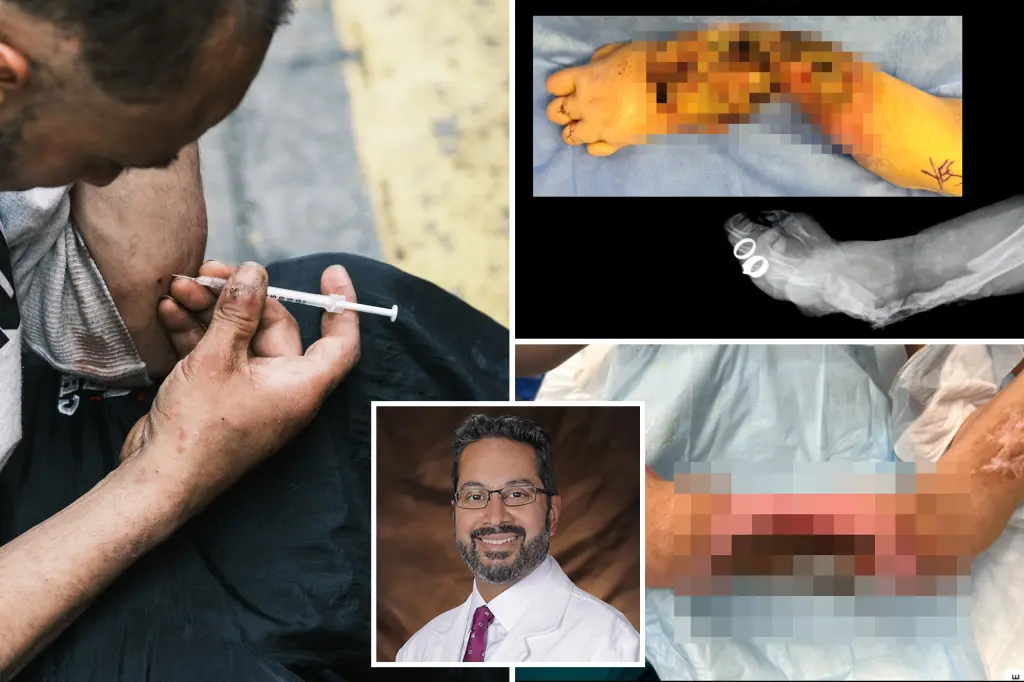
Wounds with exposed bones and tendons. A horrific smell emanating from decaying tissue. It’s a grim scene.
Despite the presence of stronger drugs, the animal tranquilizer xylazine continues to cause serious issues throughout the U.S. This illegal sedative, often called “trunk,” is typically combined with fentanyl to enhance and extend the effects.
In 2023, around 30% of fentanyl powder samples and 6% of tablet samples analyzed by the DEA were found to contain xylazine.
Philadelphia, often labeled “ground zero” for the Trunk Crisis, reported that in 2023, 38% of unintentional overdose deaths were linked to this drug.
A local orthopedic surgeon, highlighting the ongoing crisis, expressed concern that the problem is worsening. Even as fentanyl is increasingly mixed with other powerful drugs like medetomidine and BTMPS, the situation shows no signs of improvement.
“Five years ago, we barely treated patients with xylazine-related issues,” noted Dr. Asif Ilyas from Rothman Orthopedics and Drexel University. “Now, it’s a daily occurrence in major hospitals here.”
Xylazine has been around since the 1960s, originally designed by Bayer to lower blood pressure, but with serious side effects that led to its use exclusively in veterinary medicine. Its presence on the streets began in Puerto Rico in the early 2000s, with its combination with fentanyl specifically intended to prolong the effects experienced by users.
Within moments of injection, xylazine can induce a profound, zombie-like state by relaxing muscles and dulling pain. However, this comes with significant risks; it can lower heart rates and blood pressure, making it dangerous for users. Additionally, xylazine constricts blood vessels, leading to the severe skin lesions characteristic of its abuse.
Dr. Ilyas explained, “Xylazine causes local tissue damage and reduces blood supply, making tissue more susceptible to death.” This can lead to wounds resembling those caused by flesh-eating bacteria, sometimes necessitating amputation.
Most users inject in their arms or legs, where the damage is most pronounced. “The worst cases can lead to limbs becoming effectively detached due to extensive tissue damage,” Ilyas stated.
The impact of the drug can vary based on the amount of xylazine used and the frequency of injections, along with individual physiological responses to the damage.
One significant issue is that many patients leave the hospital too soon, often missing out on necessary surgical or addiction treatment. “We can clean and, in some cases, reconstruct the wounds, but if the user continues their pattern of injections, any intervention becomes futile,” Ilyas warned.
Yet there are stories of recovery. One individual, a 40-year-old who split time between Philadelphia and St. Louis, overcame their addiction in 2022 after a 45-day rehab program.
Tracy McCann, who struggled with addiction after receiving opioid prescriptions post-accident, ended up with serious infections and wounds. Realizing her needs, she sought treatment and shares her journey on social media, shedding light on the risks of xylazine.
Unfortunately, there’s no way for users to visually inspect whether fentanyl has been mixed with xylazine. While test strips can indicate its presence, they cannot determine the potency, which poses a serious risk to users.
Ilyas cautioned, “If you’re injecting fentanyl, there’s a heightened risk of it being mixed with xylazine, which not only intensifies the high but amplifies the dangers associated with those wounds.”