Approximately 165 million Americans rely on employer-provided health insurance, but workers still don't have the coverage they want, especially when it comes to medicines like Wegoby and Novo Nordisk's diabetes drug Ozempic. There is a possibility that there is no.
One in three employees is looking for more resources to combat obesity, according to a recent report from a consulting firm. gallagher. Glucagon-like peptide 1 treatments, such as Wegovy and Ozempic, are being considered, which suppress appetite by mimicking hormones produced in the intestine. game changer In this aspect.
These blockbuster weight loss drugs are soaring in popularity in the U.S., but according to Trilliant Health's “Trends Shaping 2024,'' “Americans today have higher rates of obesity and diabetes than ever before, Despite the fact that the number of health conditions is becoming more common, it is still not widely available. “Medical Economics” report.
Cost is an important issue.
Studies have shown that obesity drugs may have significant health benefits beyond shedding unwanted weight, but an organization representing U.S. insurers says concerns about obesity remain He said it remains. expensive We are involved in covering these drugs, which cost nearly $1,350 per month per patient.
Personal Finance Details:
Social Security benefits will be adjusted by 2.5% in 2025
'Great time' to review bonds as interest rates fall
Consumers are reluctant to pay return shipping costs
Several studies have shown that the price of GLP-1 drugs, along with the large number of workers who could potentially benefit from using them, is a major factor in rising health care costs. . According to a recent report, prescription drug costs have already increased by 8.6% in the last year, due in part to a surge in the use of GLP-1 drugs. mercer.
“Does it matter? Yes,” said Sunit Patel, chief U.S. actuary at Mercer.
Patients taking these drugs You will need to complete months, if not years, of continuous treatment.
“This is a lifelong medicine,” said Gary Kushner, chairman and president of Kushner & Company, a benefits planning and management company. “That's a pretty expensive commitment.”
Cost is an important factor in coverage
Less than half (42%) of companies currently cover these Somewhat expensive weight loss drugs. According to research, an additional 27% are considering adding coverage within the next year. mercer.
Still, “not everyone who wants it can get it,” Patel said.
However, 3% of employers have recently exempted these medicines, and 10% of those currently covering these medicines are considering exemptions for 2025.
To improve access to weight loss drugs, many companies will have to pay even more – and health care costs are already reaching their limits Post-pandemic highsAccording to WTW, the consulting firm formerly known as Willis Towers Watson, employers and employees will be paying significantly higher premiums in 2025. U.S. employers expect health care costs to increase by 7.7% in 2025, compared to 6.9% in 2024 and 6.5% in 2023.
A Kaiser Family Foundation survey found that employers' biggest concern was how to cover weight loss drugs, which are increasingly in demand. was also found.
“Employers face the challenge of incorporating these potentially important treatments into already expensive benefit plans,” Gary Claxton, vice president of KFF, said in a press statement.
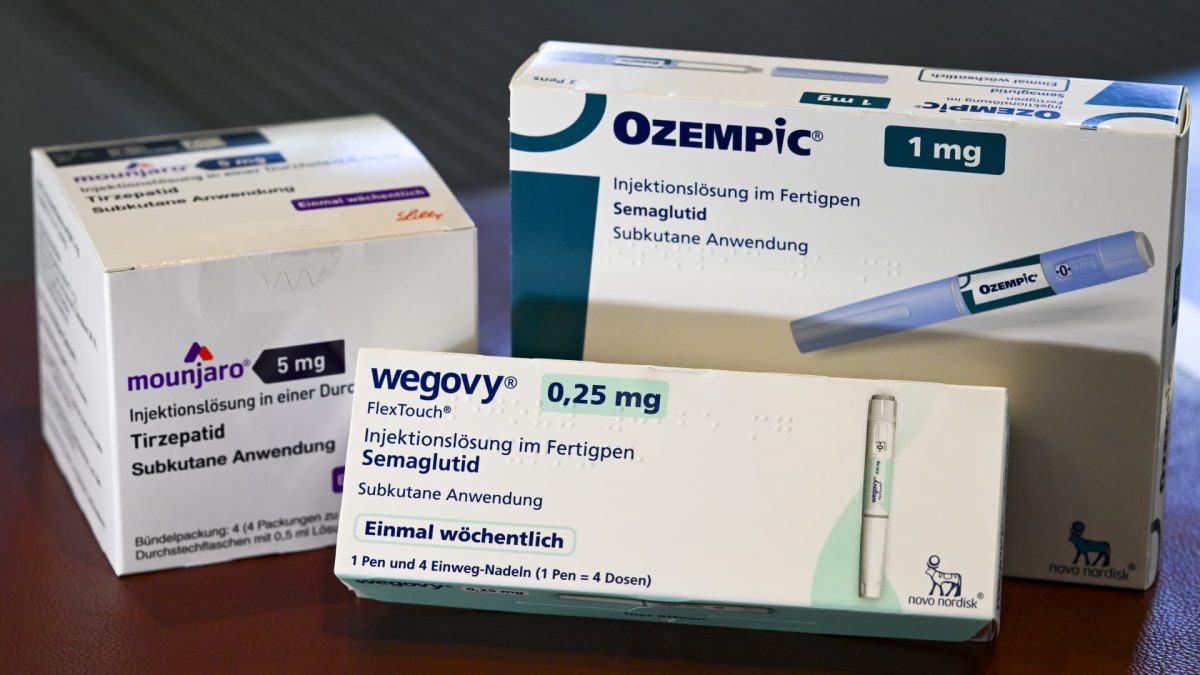
Syringes with weight loss drugs “Wegovy”, “Ozempic” and “Mounjaro”.
Picture Alliance | Getty Images
Access for weight loss is a problem
For now, some employers only cover GLP-1 drugs for the sole purpose of treating diabetes, while others cover certain GLP-1 drugs for weight loss purposes. , excludes Ozempic only if its use is approved by the Food and Drug Administration. just FDA approved for the treatment of type 2 diabetes.
“While most employers cover Ozempic as a diabetes treatment, they don't necessarily cover Ozempic as an anti-obesity drug,” said Seth Friedman, pharmacy and health plan practice leader at Gallagher. speaks.
This makes it more difficult for employees to determine whether the drug is available and covered by insurance. “They know it's covered, but they get denied,” Friedman said.
A 2023 study by the International Employee Benefit Plans Foundation found that 76% of companies surveyed offer coverage for GLP-1 drugs for diabetes, while only 76% offer coverage for weight loss. It turns out that only 27% of workers are locked out.
“There's clearly a demand for it. It's not for diabetes, it's for weight loss,” Kushner said.

“Looking to 2025, about half of large employers will cover weight-loss medications,” said Beth Umland, research director for health and benefits at Mercer. However, “even if they were able to use it, there would be guardrails around it and anyone could use it.”
The demand for these treatments is It is expected that it will increase — But added controls in coverage can also help contain costs.
Almost every employer has some form of “usage control.” limit According to Gallagher's Friedman, as well as prior authorization requirements;
For some companies, this may mean that employees must first try other weight loss methods or consult a nutritionist and enroll in a weight loss management program. Depending on how you plan, you may need to have a body mass index (BMI) threshold of at least 30, Friedman said.
This information is available during the public offering period, which typically lasts until early December.