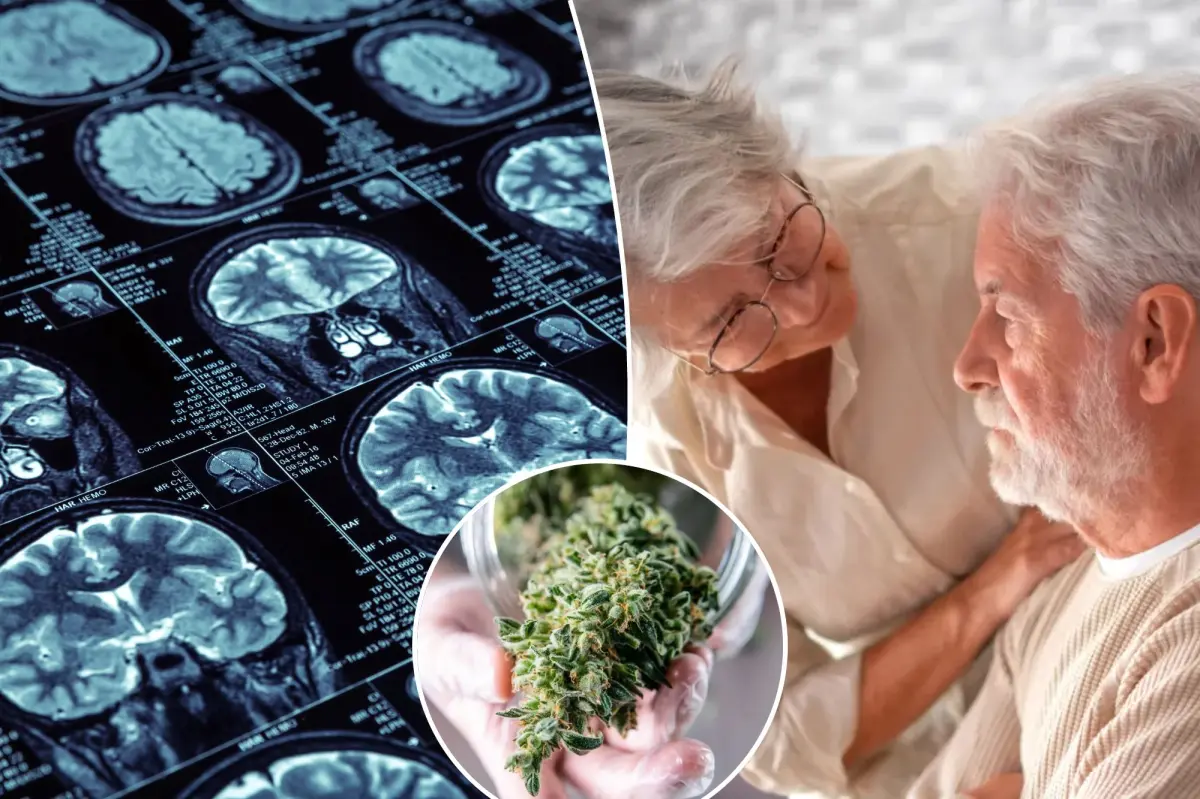
The term “pothead” might soon have a more serious connotation.
Recent studies indicate that low doses of THC, the primary psychoactive component in cannabis, could potentially safeguard memory and lessen brain damage linked to Alzheimer’s disease, especially when used alongside anti-inflammatory medications.
Although these findings are based on mouse models, researchers believe that since these drugs are already widely used, human trials could be initiated more quickly.
“Developing a new drug can take a decade or more,” remarked Dr. Chu Chen, a professor at UT Health San Antonio. “In this case, both components are already approved, giving us a significant advantage.”
This is particularly significant given that more than 7 million Americans currently live with Alzheimer’s, a number that could nearly double by 2060 unless new preventive or treatment methods emerge.
high expectations
In recent years, investigations into THC have revealed its medical properties, including anti-inflammatory and neuroprotective benefits.
The FDA has previously authorized a synthetic drug for managing nausea and appetite loss in cancer and HIV patients.
Of course, it’s not all positive. Research has shown THC could adversely impact learning and memory, but the rationale behind this remained unclear, prompting Chen to delve deeper.
In 2013, he pinpointed COX-2, an enzyme that connects to inflammation and pain, as a significant factor. Normally low in a healthy brain, COX-2 levels rise during various challenges, including injury or illness.
This enzyme has a unique function in learning and memory, but excessive COX-2 activity can lead to cognitive issues.
Chen discovered that THC can unexpectedly increase COX-2 levels in the brain, which correlates with learning deficits.
While past attempts to treat Alzheimer’s patients with COX-2 inhibitors did not improve cognitive function and resulted in harmful side effects, Chen is approaching the issue from a different angle.
Small amount, big effect
Endocannabinoids, which the brain produces naturally, interact with the same receptors as THC but often counteract its effects. One important endocannabinoid, 2-AG, diminishes COX-2 activity and reduces neuroinflammation.
Chen raised a straightforward query: Can we neutralize THC’s inflammatory effects while keeping its advantages?
The answer seems to be affirmative, especially when paired with celecoxib, a well-known anti-inflammatory drug typically used to treat arthritis pain.
The study utilized low doses of THC extract and celecoxib—much lower than those previously associated with heart complications in Alzheimer’s trials.
Mice received 3 mg/kg of THC and 1 mg/kg of celecoxib daily, roughly equating to a human taking 18 mg of THC and 6 mg of celecoxib.
The researchers examined this combination in two Alzheimer’s mouse models, one focusing on beta-amyloid plaques and the other on tau tangles, both of which are key indicators of the disease in the brain.
Treatment began prior to the mice exhibiting memory issues, allowing for the possibility of preventing or delaying the condition. They were dosed daily for a month.
Individually, low doses of THC showed some cognitive improvement but also heightened inflammation. In contrast, the combination of drugs provided stronger outcomes: enhanced learning and memory, decreased beta-amyloid plaques and tau tangles, and reduced brain inflammation markers.
Further analysis revealed that genes involved in brain function, inflammation, and Alzheimer’s risk returned to healthier levels post-treatment.
“What really matters is effectiveness,” said Chen. “If there’s no improvement in cognitive function, the treatment’s value is questionable. In this area, the combination clearly outperformed THC alone.”
what happens next
The research team intends to conduct further studies to determine if this drug pairing can slow Alzheimer’s progression or reverse damage once symptoms appear.
“This work has taken considerable time, but we’re at a stage where our fundamental neuroscience insights exhibit real potential for clinical translation,” Chen stated.
Experts suggest that even a slight delay in the onset of Alzheimer’s could significantly alleviate burdens on patients, families, and the healthcare system.
Alzheimer’s is more than simple memory loss; over time, it can erode a person’s personality, thinking, and ability to manage everyday activities.
The average survival span post-diagnosis is 4 to 8 years, and it has been projected to be the sixth leading cause of death for Americans aged 65 and older by 2022.
The stakes are high, with over one in nine individuals aged 65 or older developing Alzheimer’s. By 2025, approximately 42% of Americans over 55 may face dementia in their later years, with Alzheimer’s being the prevalent form.
Polls indicate that 92% of Americans are open to accepting a moderate or high risk associated with a drug that could decelerate the disease’s progression.