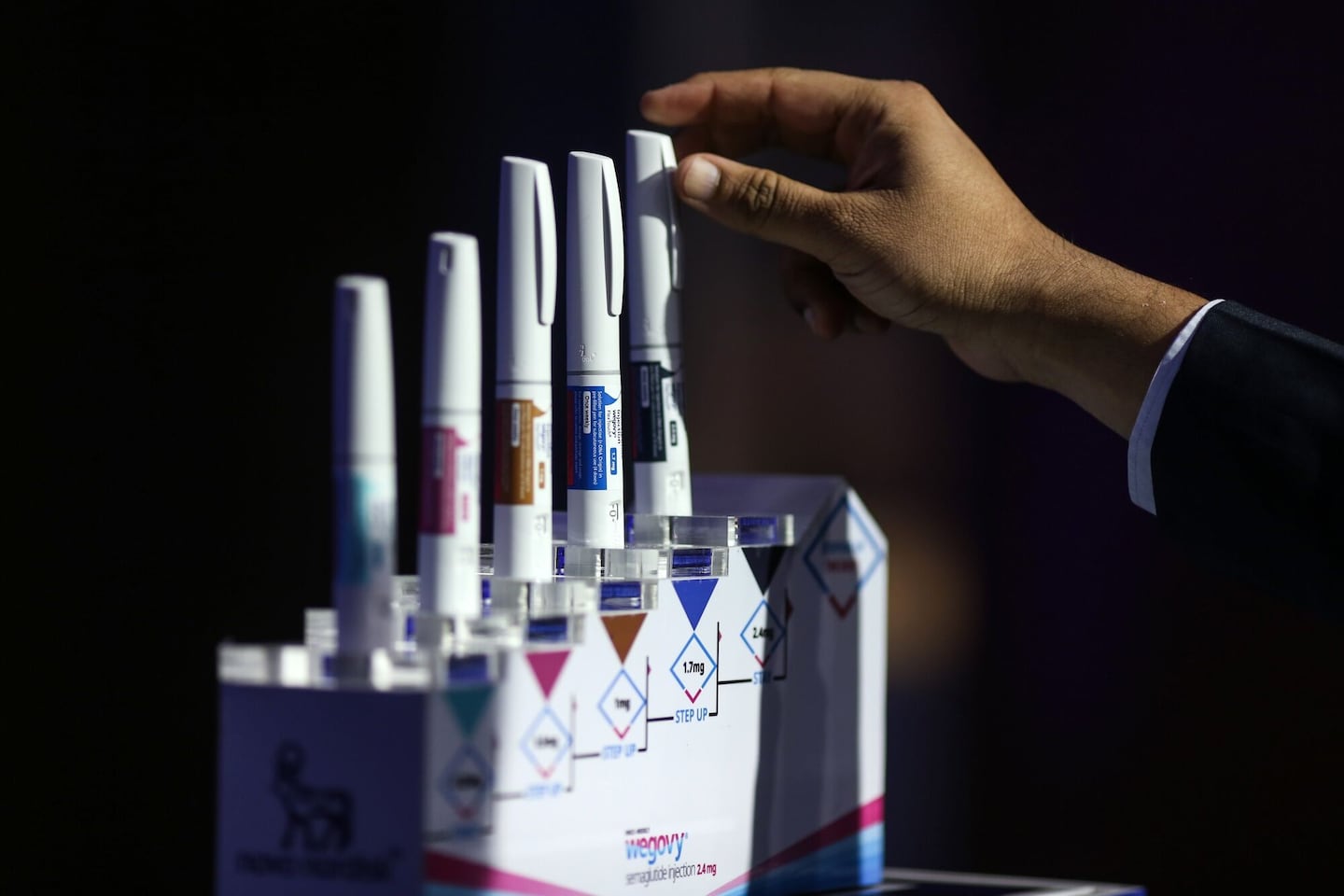
Point32Health and Blue Cross Report Operating Income While Adjusting GLP-1 Coverage
Point32Health, which owns both Harvard Pilgrim and Tufts Health Plans, announced an operating income of $86 million this quarter, a notable improvement compared to a loss of $39 million in the same timeframe last year. The organization serves around 2 million members, whereas Blue Cross of Massachusetts has about 3 million members.
Recently, both insurers have changed their policies on GLP-1 weight loss drugs like Wegovy and Zepbound, which were specifically designed for obesity treatment. These medications can be quite expensive—often reaching into the hundreds or thousands of dollars monthly without insurance. Although these drugs have become increasingly popular, individuals managing diabetes still retain coverage.
Officials from both companies pointed out that alterations in the coverage of GLP-1s contributed significantly to their financial performance. Mike Malone, CFO of Point32Health, indicated that the modifications to GLP-1 coverage could result in savings exceeding $100 million in 2026.
Meanwhile, Mike Guerriere, Blue Cross’s chief actuary, mentioned that while these savings are promising, customers might not see major reductions in rising premiums. Factors such as escalating medical and drug costs are likely to keep pushing premiums upward. Guerriere expressed skepticism about the likelihood of significant changes in these trends, saying it’s challenging to envision a scenario where this persistent high-cost environment diminishes.
Marrone, another executive, suggests that while he remains optimistic about the latter half of the year, the volatility in healthcare and drug pricing remains a concern.
It’s worth noting that just because current results look good, it doesn’t necessarily guarantee that either organization will conclude 2026 positively. Umesh Krupad, director of the Massachusetts Health Policy Commission, pointed out that insurance performance can vary with the seasons, often doing better in the first quarter.
Guerriere also mentioned that quarterly results were influenced by unique circumstances, such as a milder flu season and severe winter weather that kept many patients at home rather than utilizing emergency services.
Krupad, who was previously CFO at Point32, remarked on how the companies have made some effective moves, though he cautioned that the tightening of GLP-1 and other benefits may not be in consumers’ best interests.
Patients have expressed frustration over the decision to exclude GLP-1 from weight loss treatment, leading to a sharp increase in their out-of-pocket expenses. Although some direct-to-consumer programs have emerged offering these drugs for under $499 monthly, many still find them unaffordable.
Additionally, Guerriere noted other steps that have helped Blue Cross achieve positive operating income. These include aligning premiums with rising healthcare costs, steering behavioral health patients to in-network providers, and cutting internal costs. Recently, Blue Cross has offered buyouts to hundreds of its staff, a move it hadn’t made since the late 1980s.
Over the last two years, Blue Cross has experienced record operating losses, totaling around $380 million. In contrast, Point32 faced its fifth consecutive year of millions in losses and has downsized its workforce by more than 450 positions since March 2025 to improve financial health.
It’s not just these two organizations facing challenges; Fallon Health, a smaller player in Massachusetts, has also limited coverage for GLP-1 drugs to curb expenses beginning January 1. Fallon, serving over 200,000 members, reported an operating income of $1.5 million for the first quarter of 2026, a turnaround from a loss of $8.1 million the previous year. While they did not specify GLP-1 changes as a reason for their financial restructuring, other adjustments have been implemented.
Moreover, the Group Insurance Commission, which provides health insurance for public employees and retirees in Massachusetts, has also restricted GLP-1 funding. The City of Boston recently announced a deal with union groups to cease the use of non-specialty GLP-1 drugs, a move expected to save the city around $11 million.
Massachusetts has been grappling with escalating healthcare expenses for some time. According to a report, the state’s health spending is projected to exceed containment standards for the fourth year in a row in 2024. Spending is anticipated to rise by 5.7% this year, driven mainly by costs associated with prescription drugs and outpatient hospital services.
With insurance premiums already on the rise, they’re set to increase further. For instance, the Group Insurance Commission authorized an average premium hike of 7.5% for many public employees for the 2027 fiscal year. Meanwhile, decisions on individual and small group plans will be made by the Massachusetts Department of Insurance later this year, following the anticipated proposals.