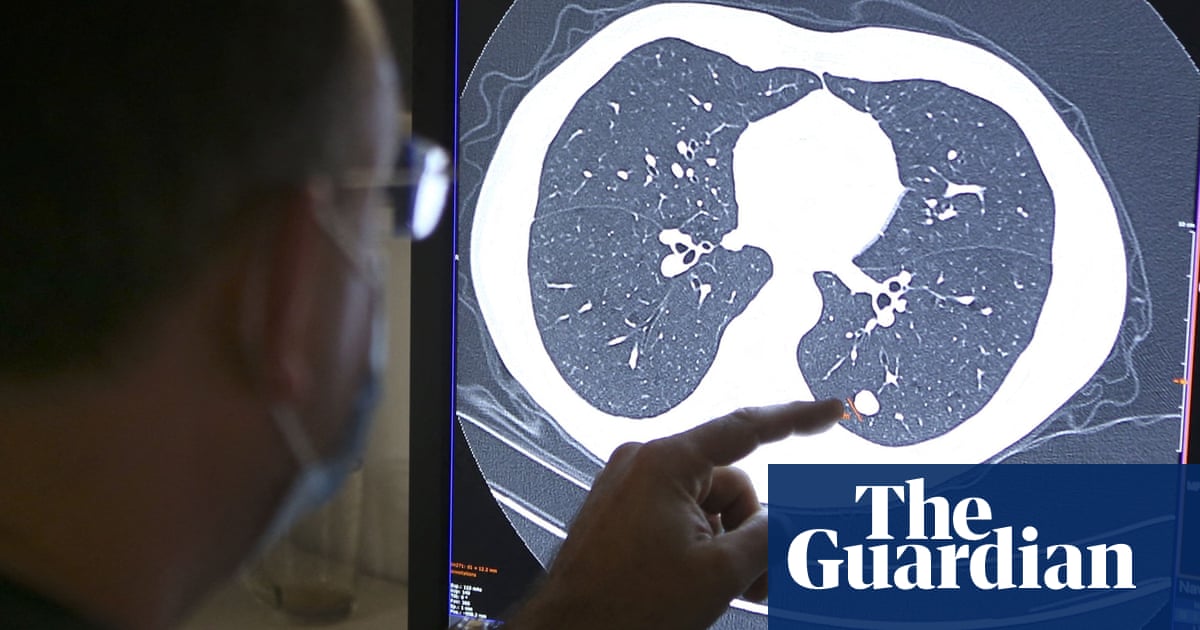
Many individuals might risk becoming a “martyr” by ignoring potential cancer symptoms, fearing they’ll burden the NHS. There are growing calls for early testing to identify those at higher risk.
A recent report by a health consulting firm outlines how the UK’s NHS could identify more cancers earlier, ultimately saving lives by transforming into an “early intervention service.” This push for dedicated cancer strategies has existed since the government’s formation back in 2015.
Interestingly, research shows that in the UK, more people with possible cancer signs hesitate to consult their GPs compared to other nations. It seems there’s a prevailing sentiment of not wanting to waste a doctor’s time.
Cancer specialists are stressing the importance of getting symptoms like fatigue, bleeding, and weight loss checked out urgently. Early treatment can significantly improve outcomes.
This sluggish response seems to contribute to the UK’s poor early diagnosis statistics on a global scale. Although cancer survival rates are on the rise, the UK still lags behind other countries despite initiatives encouraging faster symptom reporting.
“No one should feel they’re bothering their doctor if something doesn’t feel right. They’re not ‘troubling’ GPs or ‘taking money’ from the NHS,” said Naser Turabi from Cancer Research UK.
Addressing this reluctance to seek help is vital for improving cancer diagnosis rates in the UK, particularly for stages 1 and 2, when treatment is more likely to be effective, according to the report. Mike Birtwistle, the author, conducted interviews with cancer doctors and senior NHS staff in his research.
“We don’t want people with symptoms to feel like martyrs for not wanting to overload the NHS,” Birtwistle noted. “Many delay seeking help, leading to later-stage diagnoses that diminish survival chances.”
The report advocates for the NHS to actively engage individuals showing cancer signs, raising public awareness about symptoms, and motivating prompt action. Experts believe people have been conditioned to avoid bothering the NHS.
It also points out that GPs may unintentionally discourage patients from undergoing checkups, fearing to add more pressure on an already strained system. “Primary healthcare professionals sometimes contribute to a culture of restraint when it comes to seeking help,” it suggests.
Moreover, research indicates that the UK takes longer than many other countries to diagnose cancer. Findings last year from Macmillan Cancer Support revealed that survival rates are trailing behind those in other European nations, leading to preventable deaths.
Each year, the number of cancer diagnoses in the UK continues to rise, with around 412,400 individuals diagnosed—one every 90 seconds—due to factors such as an aging population and lifestyle choices like obesity and alcohol consumption. About 167,000 people die annually from cancer, making it the second-leading cause of death after heart disease.
Between 2018 and 2024, the NHS failed to meet its goal of diagnosing 75% of cancers at stages 1 and 2, with only 60% detected by that timeframe, according to the report.
However, there is potential for improving early detection in the future.
- Screening for prostate cancer should be targeted at men at higher risk, including Black men and those with a family history or specific genetic predispositions.
- Lung cancer checks could be expanded to those exposed to passive smoking or residing in polluted areas.
- People with pancreatic cancer and symptoms like weight loss and diabetes should undergo evaluations.
- Liver health checks could be extended to high-risk individuals at GP surgeries, homeless shelters, and sexual health clinics.
- Assessing the health of the esophagus in patients taking proton pump inhibitors, which can increase the risk of esophageal cancer, should also be prioritized.
Birtwistle urges the government to implement more assertive cancer detection strategies in upcoming health plans. Nevertheless, some prioritize improving attendance for current cancer screening programs—breast, bowel, and cervical—before considering the introduction of new initiatives that may lack solid evidence.
Hospitals might benefit from providing home testing kits, convenient online appointments, and specialty screenings, he adds.
Sarah Woolnough, CEO of King’s Fund ThinkTank, highlights that strong evidence supports early cancer detection as crucial for improving treatment and survival rates, stressing efforts should focus on making access easier and more streamlined.
Professor Stephen Powis, National Medical Director of NHS England, emphasized the NHS’s improved ability to diagnose and treat cancers at early stages. About 7,300 additional people are diagnosed at stage 1 or 2 each year compared to pre-pandemic numbers.
“There are various reasons individuals might hesitate to seek screenings, from not recognizing crucial symptoms to concerns about overburdening the NHS,” noted Powis.
Health services are adopting innovative methods to enhance early diagnosis, such as offering lung checks to smokers on mobile scan units in supermarket parking lots—leading to thousands being diagnosed earlier than otherwise possible.